"All I remember is hearing screeching and then blackness," Anthony Loubet said as he talked about the car accident that changed his life.
Before the accident, Anthony was a busy deputy county attorney and father of 6 who volunteered his time serving on a variety of leadership committees. After the accident, his short-term memory was so severely impaired that he couldn’t really read, much less work or drive. He suffered from depression and severe mood swings. He was aware of things that he needed to do and thought he should be able to do, but he was too exhausted and overwhelmed to deal with them. The symptoms took a heavy toll on both Anthony and his loved ones.
In the months following the accident, Anthony followed the orders of the doctors and his therapists faithfully. He improved in small increments for a while. But his progress quickly plateaued, leaving him frustrated and far from the ‘normal’ he previously knew.
 Then, the chiropractor Anthony saw for his neck pain recommended a nearby concussion treatment clinic: Cognitive FX. A week of intense treatment put him on the road to recovery. Today, he’s working 40+ hour weeks, learning guitar, and enjoying leisure time with his family.
Then, the chiropractor Anthony saw for his neck pain recommended a nearby concussion treatment clinic: Cognitive FX. A week of intense treatment put him on the road to recovery. Today, he’s working 40+ hour weeks, learning guitar, and enjoying leisure time with his family.
In this article, we share Anthony’s story, what therapies he tried before Cognitive FX, and why treatment at our clinic finally made the difference for him. (Anthony Loubet, deputy county attorney and father of six, is photographed on the right.)
If you’re suffering lingering symptoms of a concussion after an accident, you’re not alone. Not all patients recover with rest and time. If you’d like to learn whether we can treat your symptoms, schedule a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
Concussion From a Car Accident
On February 26, 2019, Anthony Loubet, a deputy county attorney in the Civil Division of the Utah County Attorney’s Office, was stopped in a line of cars in the exit lane of the freeway, trying to get home after a day at work. He remembers hearing the screeching of tires, but not what happened next.
He learned from the police report that a semi-truck and a Dodge Durango tried to avoid the line of stopped cars by merging left. However, they merged too closely, hit each other, and then hit Anthony’s car. The impact pushed his car (a Honda Fit) into the car in front of him, and then forced his car out into traffic, where it came to a stop. The airbags deployed and Anthony lost consciousness.
When he came to after the car crash, he couldn’t move. He had a sharp pain in his back and his neck hurt. He was transported by ambulance to the emergency room (ER) where he underwent an MRI of his brain, a CT scan of his ribs, and an x-ray of his hand.
The MRI didn’t show any structural damage or bleeding in the brain (so, no severe traumatic brain injury). The CT scan of his ribs and the x-ray of his hands didn’t show any breaks, though fractures were suspected. He went home from the ER feeling a bit dazed, but thinking that he got off lucky all things considered. He assumed he’d escaped serious injury and would be feeling just fine before long.
A Second Visit to the ER
It wasn’t until the next day that Anthony realized something was very wrong. Trying to work from home, he sat down at the computer.
“As I was looking at my computer trying to read, I realized I couldn’t read,” he said. “It wasn’t that I couldn’t make out the words, but my short-term memory was impacted so I couldn’t keep anything in my head long enough to know what it was.”
Things got worse over the next few days. He’d ask his wife a question but immediately forgot what she’d just said. He’d fall asleep without warning in the middle of the day. His stomach was severely distended from the accident, resulting in uncomfortable symptoms.
So, his wife took him back to the emergency room. Anthony promptly got lost in the ER after visiting the bathroom. Fortunately, the nursing staff found him and realized that he was showing multiple signs of a concussion.
The ER doctor recommended that they find a concussion specialist. He also advised that Anthony get complete rest: no reading, sound, electronics or any kind of stimulation.
 Anthony with his wife and children.
Anthony with his wife and children.
Lingering Concussion Symptoms After the Accident
Anthony followed the doctor’s orders, but there was no quick recovery.
The first couple of months after the accident were extremely frustrating since he was told to rest and to avoid all stimulation and socialization. He couldn’t work or use electronic devices. He had to step down from his leadership positions. So much of what he had done before the accident was now off-limits. He said, “Going from being involved in all these boards and going all these places to all of a sudden doing nothing was a nightmare.”
The persistent symptoms he experienced were an extension of the nightmare.
Short-Term Memory Loss
The short-term memory loss was one of the most difficult concussion symptoms that Anthony dealt with. Not only did it affect his conversations and ability to adhere to a schedule, it also affected his ability to drive. It took about three months before he could drive even short distances.
“I just didn’t have the endurance to focus long enough on the road,” he said. It took longer to get places using public transportation, but that’s what he had to use if he went anywhere without his wife.
Difficulties with short-term memory also impaired his ability to create long-term memories. There are things he does remember during those months only because of the repetition from talking about them with his wife and doctor. “I talked about it so much that it’s kind of been solidified in my long-term memory,” he said. “But if you start really asking me what happened before that or after that, it’s like, ‘Oh, I don’t know. It’s gone.’”
Extreme Mood Changes
Another symptom that took Anthony and his family by surprise was his extreme, unpredictable mood swings. Before the accident, he’d hardly ever gotten angry. After the accident, little things set him off.
For example, when the refrigerator’s ice maker broke, he wasn’t able to fix it, even though it would have been easy before his head injury. Moments like that made him snap unexpectedly. “I’d just lose it; I’d get extremely angry,” he said. “And in the next moment, I’d feel like ‘I wish I was dead. It would have been better if I had died.’”
“My kids would get scared because of the drastic outbursts that I would have because it would be like zero to 60,” he added.
His alarmed wife called the doctor and was told that a mild traumatic brain injury could cause him to have manic and severe depressive episodes if he got overstimulated with things that his brain couldn’t handle. She was told that he was at risk of suicide during this period and needed to be watched.
It’s something he wished he’d known from the beginning so that they could have prepared for it.
Other Frustrating Symptoms
A variety of other symptoms persisted after the concussion. He experienced light sensitivity. He couldn’t tolerate large groups of people. He got lightheaded and dizzy when he tried to do cardio. He was easily exhausted and overwhelmed.
An Incomplete Recovery
About two months after the accident, Anthony tried to start working from home. He was only able to work about 2 hours a few days a week, but even that little bit of time had to be broken up.
In May, he went into the office for 2 half-days. It was a disaster. “Lights were too bright,” he said. “People would talk and I didn’t know what they were saying because I couldn’t differentiate multiple voices.”
He was also still having trouble remembering anything that he’d read. All his work had to be reviewed. (Looking back at some of the drafts he wrote at that time, he pronounced them, “so bad.”)
At one point, he closed his door to his office. “I was just on the floor, crying, because I didn’t know if I’d ever be back to me,” he said.
In the meantime, he sought medical treatment from multiple specialists and tried his best to get work done in the office.
Neurorehabilitation Specialist
Anthony found a neurorehabilitation specialist who has a lot of experience working with people with brain injuries to direct his treatment. He remembers some of the initial assessments with this doctor that illustrate just how impaired his short-term memory was.
For example, when the doctor listed 5 animals and asked him how many he remembered, Anthony could only recall the last one on the list. When the doctor asked him what kinds of animals he’d see at a zoo, Anthony listed a few primates. The doctor asked about animals other than primates that might be at a zoo. “I can’t think of anything,” he responded. His brain just couldn’t remember anything else.
To work on those deficits, the doctor sent him to a cognitive rehabilitation specialist.
Cognitive Rehabilitation Specialist
Anthony worked with the cognitive rehabilitation specialist every two weeks. She did periodic cognitive testing to check for improvement. He was below average in some categories and deficient in others.
The therapist worked with him to create strategies to cope with his memory problems. He had to take a lot of notes and use a planner.
For example, she gave him a picture of a hand to post in his home. Each of the 5 fingers represented 5 things he was supposed to take to work: his keys, his badge, his bag, his water bottle, and his planner. Unfortunately, even this was not always successful. “I’d get out to my car and go ‘Oops; I forgot my keys,’” he said. “I’d get to work, and ‘Oh! I forgot my badge!’”
The therapist also worked with him on strategies to share his feelings. She encouraged him to talk with his wife so she would know how he was feeling and what was going on.
The therapist didn’t want to give him any homework to do in between visits because his work as an attorney was already so mentally rigorous. She felt that his job would be enough of a workout and didn’t want to overload his brain.
Neuropsychiatrist
Anthony also met with a neuropsychiatrist to help with the mood swings and emotional aspects of his condition and recovery, especially his frustration at reaching a recovery plateau.
They talked through these frustrations, and the doctor helped him figure out positive coping mechanisms. These strategies also helped Anthony to recognize when frustration was building and gave him positive ways to release the emotional energy before it overflowed. Techniques such as watching comedies, joking, crying, and laughing all helped.
Additionally, Anthony was taking Duloxetine for mood regulation to help with his anger and depression.
Chiropractor
Soon after the accident, Anthony started seeing a chiropractor whom he had seen after a previous car accident for the physical aspects of recovery. She uses physical therapy and massage therapy techniques in treatment.
Hitting a Plateau
Anthony improved slowly for a few months, but eventually felt like his recovery had plateaued. He managed to work half-days for five days a week, but that’s the most he could manage — and at the end of the day, he was exhausted. “I wasn’t getting more energy,” he reflected. “I wasn’t getting quicker. I was just kind of blah.”
Cognitive FX: Scared to Hope
It was Anthony’s chiropractor who first told him about Cognitive FX. She had gone to a presentation given by Dr. Alina Fong, Clinical Neuropsychologist and co-founder of Cognitive FX. She was impressed by the presentation and suggested that Anthony check it out.
The attorney representing him in the car accident settlement also knew about Cognitive FX. Many of their clients had been there for treatment and improved significantly.
Despite their recommendations, Anthony hesitated. While making his decision, he asked his acquaintances if they had any positive experiences with Cognitive FX. He was surprised to learn just how many of them had had family members or friends who had gone through treatment, many of whom improved drastically.
One person told him of an aunt who had never been the same after an auto accident 30 years ago. He said that she went through treatment for post-concussion syndrome and everyone in the family could immediately tell the difference.
These stories gave him hope, but he wondered, “Am I going to be one of those people?”
Eventually, he decided to pursue treatment at Cognitive FX. “I was scared to hope,” he explained, “because if this didn’t work, I didn’t know what other options I would have.”
The First Step to Recovery: A Better Brain Scan
Prior to treatment at Cognitive FX, every patient undergoes a functional neurocognitive imaging scan (fNCI). fNCI is a type of MRI that allows our doctors to see blood flow in the brain while patients perform a series of cognitive tasks. We can then determine where and how the brain was affected by the injury and target those areas for treatment. (We’ve written elsewhere about how an fNCI works, and how it’s different from other scans.)
During the scan, patients take six different cognitive tests in a span of about 45 minutes. Anthony had a hard time focusing during the tests and couldn’t remember anything for the final test. His brain was too fatigued.
Overall results of the fNCI are color coded and summarized in a score we call the severity index score (SIS). The green area can indicate some impairment, yellow is worse, and red is (you guessed it) even worse. Scores above the red zone — which already indicates severe dysfunction — indicate significant dysfunction. For reference, non-concussed brains typically score close to zero.
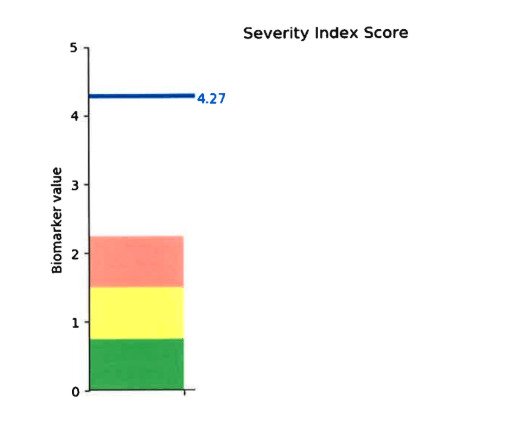
Anthony’s overall score was a 4.27 — far beyond anything resembling an efficiently functioning brain. When he saw the results, all his symptoms and months of frustration started to make sense.
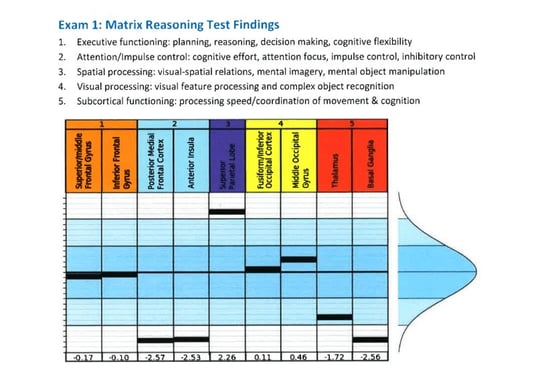 Patients complete six different tests during the fNCI. An uninjured brain region typically falls in the darker blue region. Brain regions that score in the white zone are either hypoactive (the lower part of the picture) or hyperactive (the upper part of the picture). For example, Anthony’s Anterior Insula, which is involved in attention and impulse control, was hypoactive.
Patients complete six different tests during the fNCI. An uninjured brain region typically falls in the darker blue region. Brain regions that score in the white zone are either hypoactive (the lower part of the picture) or hyperactive (the upper part of the picture). For example, Anthony’s Anterior Insula, which is involved in attention and impulse control, was hypoactive.
The areas of his brain that were supposed to be participating in everyday tasks were not doing their part, so the rest of his brain was trying desperately to overcompensate — and exhausting itself in the process. “It took a lot more to do what I used to be able to do,” he said.
Trying an Active Approach
Anthony recalls feeling reassured by the Cognitive FX team, who explained that they’d seen all of his symptoms before, and that they could help him.
His care coordinator explained that the brain is a muscle, just like any other muscle in the body. To help it recover, you need more than just rest.
“If I had broken my leg and did nothing, the bone would heal, but it would never get back to what it was before because I’m not using it,” Anthony said. “I thought it was interesting that their approach was to try to target those areas of the brain that aren’t really firing and start getting them to work again. That way, it’ll start engaging and drawing blood in again, and get stronger.”
Tackling Treatment Week
For most patients at Cognitive FX, the bulk of treatment happens during one intense week of therapy at the clinic, though patients are expected to continue to work at home afterwards with their individualized, post-treatment exercises.
Monday is a lighter day. Patients meet their therapists, take some baseline tests, and get introduced to the therapy modalities they will be doing. Anthony remembers neuromuscular therapy, cognitive therapy, psychotherapy, and Dynavision therapy. “It was pretty tiring,” Anthony said, “but a lot of it was just getting in the flow of things.”
Tuesday started with a cardio session. For treatment to be effective, it’s necessary to get the heart rate up a bit so that the blood is flowing to the brain. One of Anthony’s post-concussion symptoms, however, affected his ability to exercise. “I tried to do it,” he said, “but I got super dizzy.” His therapists helped him breathe it out and keep going.
The last exercise of the day was also memorable for Anthony. It involved balancing on a board while catching either a red or a green ball that was bounced or tossed to him and throwing it back. The added twist is that if the ball was red, he had to say a type of animal in alphabetical order. If the ball was green, he had to say a word that started with the letter 'g'.
Anthony attempted to maintain his balance on the board while trying to do this exercise. The therapists took it slow, but he really struggled. “I was just hanging on words, trying to think of something,” he said. But the words just wouldn’t come.
The First Signs of Change
Anthony went home that night feeling overwhelmed and exhausted. “When I got home that day, I felt like my head was just going to crack open,” he said. He was super tired, but he had a hard time going to sleep. Something felt strange, but he couldn’t say what. He finally fell asleep around 1 a.m. and woke up at 5 a.m.
Something had changed during the night.
“When I woke up at 5 a.m., all these words were just flooding into my head,” he said. “Granite, graphite, grass, green, German, germane… It was like a print queue — like everything had been held up, and now there’s paper in the printer,” he exclaimed. “I was exhausted, but I didn’t feel super tired because things started coming quicker to my head. I hadn’t felt like that since the accident.”
The changes continued. On Wednesday, he was able to do cardio interval training without any problems. There was no lightheadedness. “My test scores on Wednesday were significantly improved,” he said. “Things started coming faster. I was feeling happier.”
Thursday was another exhausting day. He felt his performance dip a little bit that day, but it was still a different feeling. He said, “It wasn’t as much cognitive fatigue as it was physical fatigue. I could feel that things were improving; things were getting better.”
Drastic Improvement on the Post-treatment fNCI
At or near the end of treatment week, every patient undergoes a follow-up fNCI to compare brain activity before and after treatment. Anthony went through his scan at the end of Thursday. On Friday, he got the results.
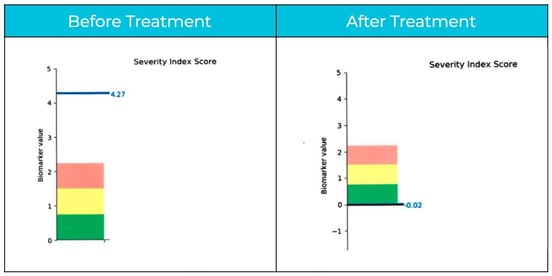
“My score went from a 4.27 to a -0.02,” he said. “They said, I don’t think we’ve ever seen anyone make this drastic of an improvement.” He was thrilled.
He also noticed that he was retaining short-term memories of specific exercises that he did during the week. His care coordinator explained that the treatment process is designed to get those synapses firing and the blood flowing in those areas again. She also explained that those areas of the brain will get stronger and quicker as he keeps engaging them with the therapy exercises he continues to do at home.
Rebuilding His Life in a Healthier Way

When Anthony returned to work after his treatment at Cognitive FX, the change was immediately evident. “I came back to work, and everybody noticed that there was something different because I had been so slow to do things, to communicate, or to think of things,” he said. “I came back, and I was happier; I was faster.”
He was so drastically different that one of his co-workers even jokingly asked if a secret government agency had kidnapped him and reprogrammed his brain!
By December 2019, Anthony was cleared to work 40 hours per week. By January, he had the approval to work more than 40 hours per week without restrictions (more typical work hours for an attorney).
There have been other changes as well.
His mood swings improved so much that he was able to go off his medication, though that came with its own set of withdrawal symptom struggles. “The fact that I’ve been able to be off all medicines has been nice,” he said.
Anthony now plays basketball on Fridays with his co-workers. He still takes public transportation to and from work, but it’s not a necessity; it’s a choice. It allows him to incorporate more walking and exercise throughout the day.
His leisure activities have changed, too.
Anthony took up playing the guitar after treatment as a way to find something productive to do and to engage his brain when he couldn’t handle large groups of people. It now helps by providing a positive, creative outlet when he starts getting stressed or emotional. He also enjoys woodworking, car repair, and reading.
He’s still working with the neuropsychiatrist to help repair some of the relationships that suffered after the accident. The doctor has also helped him to recognize when he’s feeling down or tired, and to find healthy ways to cope.
“If you can find things to do that are a positive reinforcement, like playing guitar, going for a walk, playing basketball, then you’re teaching yourself to stop withdrawing,” he said. “You’re showing your brain that you can do other stuff. You kind of shift gears.”
Other positive strategies that they’ve implemented are things like watching comedies, telling jokes, crying, and laughing. “It helps release that emotional energy that’s building,” he said.
“I’m doing better,” Anthony reflected. “I’m able to function.”
If you’re suffering lingering concussion symptoms after an accident, you’re not crazy. Not all patients recover with rest and time. If you’d like to learn whether we can treat your symptoms, schedule a consultation.

 Then, the chiropractor Anthony saw for his neck pain recommended a nearby concussion treatment clinic: Cognitive FX. A week of intense treatment put him on the road to recovery. Today, he’s working 40+ hour weeks, learning guitar, and enjoying leisure time with his family.
Then, the chiropractor Anthony saw for his neck pain recommended a nearby concussion treatment clinic: Cognitive FX. A week of intense treatment put him on the road to recovery. Today, he’s working 40+ hour weeks, learning guitar, and enjoying leisure time with his family.












