Depression After a Concussion or Brain Injury
Depression, one of the five stages of grief, may be the most familiar, and frustrating, feeling experienced after a traumatic brain injury (TBI) or concussion. And it’s not a fun one. Depression is a...
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY
If you’ve experienced a concussion or traumatic brain injury, you may already know that a bewildering array of symptoms can occur days, months, and even years after the injury.
Concussions can cause body temperature regulation problems such as chills, shivering, sweating, hot flashes, and altered core temperature that come and go — and seemingly defy logic.
These symptoms can be elusive and sometimes alarming, but they’re very real. Contrary to popular concussion myths, you don’t have to experience loss of consciousness at the time of injury to experience serious symptoms.
Fortunately, most of these symptoms resolve or noticeably lessen with successful concussion treatment. In the meantime, during your recovery, you can also take steps to feel better.
In this guide, you’ll learn:
Every concussion is unique, but 95% of our patients show statistically verified restoration of brain function by the end of their first week. Our specialty is helping patients recover from persistent and “unusual” head injury symptoms. To discuss your specific injury and symptoms, schedule a consultation with our team of experts.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.

In your body, thermoregulation or temperature regulation is what’s known as a homeostatic process, meaning your body does everything it can to maintain temperature as close as possible to a healthy baseline: Around 98.6 degrees Fahrenheit (37 degrees Celsius).
Normal, healthy body temperatures actually range from about 97-99.5 degrees Fahrenheit and depend on individual factors like metabolism and hormones. Going outside of that range isn’t optimal for long-term health and is usually a sign of underlying problems.
Your body regulates temperature very strictly because:
Some common causes of temperature regulation problems that aren’t traumatic brain injuries include:
Fortunately, your body has multiple fail safes in place to help your body temperature stay within the safe range.
For example:
In a healthy person, these mechanisms work together like checks and balances to keep body temperature where it ought to be.
This entire process is controlled by a part of the brain called the hypothalamus and by your autonomic nervous system (ANS). There are feedback loops going both ways. In other words, the hypothalamus and ANS constantly “talk to” one another with signals about temperature.
You can visualize how your body’s thermoregulation system works with this graphic:
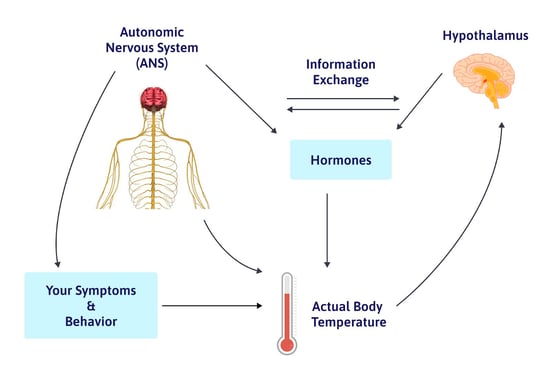
Finally, secondary processes in your body can also influence temperature, including your diet, individual metabolism, and hormones such as thyroid hormones, cortisol, progesterone, estradiol, and testosterone. These processes aren’t the main drivers of thermoregulation but still have an affect on your temperature.

Briefly stated, concussions can interfere with your body’s thermoregulation process because they can affect nearly all of the systems described in the previous section, including your hypothalamus, autonomic nervous system (ANS), and hormone levels.
Many people, even severe head injury survivors, don’t realize that concussions can result in system-wide symptoms and health problems. The root causes of many lasting concussion symptoms are a disruption in neurovascular coupling, which is the relationship between neurons and the blood vessels that supply them with oxygen and other nutrients, and alterations in the function of the autonomic nervous system (dysautonomia).
Here’s a brief synopsis of the specific mechanisms by which concussions affect thermoregulation:
Note that these temperature changes don’t have to be throughout your entire body. For example, some patients notice unusual flushing and warmth in their faces with physical activity, cognitive exertion, or stress.
These and other symptoms can come and go mysteriously or follow strange-seeming trends, even after a mild traumatic brain injury. If your healthcare provider dismisses your symptoms or insists there’s no link between concussion and body temperature problems, they’re misinformed.
Patients who are struggling with lingering concussion symptoms do best with support and a treatment plan that’s designed to address their individual needs. You can learn more about what to look for in a concussion care provider here.
In the following sections, we dive more into specific head injury-related symptoms of fever, feeling hot, and feeling cold.
Yes, Head Injuries Can Cause Fever: Here’s What to Do about It
Yes, head injuries can cause fever. The name for this phenomenon is neurogenic fever, because the fever isn’t caused by infection but instead has a neurological basis.
Research suggests that between 4-37% of TBI survivors experience neurogenic fever.
The majority of the time, fever caused by head trauma is an acute or short-term symptom. Potential concussion-related causes of fever include inflammation or a faulty immune response due to the concussion (that is, your immune system might mistakenly respond as though you have an infection, even though you don’t).
Neurogenic fever is associated with worse outcomes following a concussion. In some cases it’s life threatening and can also result in permanent brain damage. If you’ve recently had a concussion and are experiencing a fever of 103 or higher, please visit the emergency room or seek professional help immediately.
Aside from an acute fever response that follows a concussion, most post-concussion temperature regulation issues are uncomfortable but aren’t emergencies.
But if you’re experiencing a fever of 100.5 degrees Fahrenheit or higher, you should still treat it as a medically significant event, even if your concussion wasn’t recent.
It’s not possible for us to diagnose the cause of a fever or provide medical advice remotely, and it’s best to be on the safe side during the coronavirus pandemic. That means consulting a physician and taking any necessary precautions until you know the cause of the fever.

Even if you don’t have a fever, you can still experience issues like waking up drenched in sweat or feeling “hot flashes” that come and go. Or, you might experience localized flushing and redness in certain parts of your body but not others. These symptoms can emerge anywhere from days to months after a brain injury.
Your symptoms may be accompanied by body temperature elevations, or your body temperature might be 98.6 degrees Fahrenheit or even on the low side.
Either way, you’re not imagining things, and these are absolutely symptoms that could come from a brain injury.
Most often, they occur because your hypothalamus isn’t processing signals from your autonomic nervous system correctly, or because its homeostatic set point is too high (like a faulty thermostat).
While dysfunction in the hypothalamus and ANS are the most common culprits, hormonal changes resulting from a concussion are another potential culprit, especially in women. Sometimes after a concussion, women experience a full range of menopause-like symptoms, including hot flashes, that can be misinterpreted as “early menopause.” In one study, for example, 46% of women with TBI experienced amenorrhea (lack of menstruation) for up to 60 months.
Until you get treatment for post-concussion syndrome, you can take steps to make yourself more comfortable. We recommend using a fan to direct a cool breeze at yourself, opening a window to let in fresh air, turning down the thermostat, changing your outfit or removing layers, or drinking cool water.

Low body temperature, chills, and related symptoms may not be as disruptive or concerning compared to other post-concussion symptoms (such as changes to your blood pressure or heart rate), but they’re still uncomfortable and can lower your quality of life.
Shivering is evidence that your body’s trying to warm up, either because it’s cold or because it perceives that it’s cold. You might notice localized blue, purple, or unusually white skin in areas that feel cold, like your hands or toes. One cause could be inappropriate vasoconstriction, especially if your hands and feet are cold. For example, if you have Reynaud’s syndrome, it can develop or get worse after concussion. Usually this is a result of miscommunications between the hypothalamus and autonomic nervous system.
Concussions can also lower body temperature by altering your hormone levels or disrupting your metabolic function. As an example, if a brain injury interferes with your thyroid function, your core temperature may decrease.
It’s also possible to feel cold or experience chills or shivering with a normal body temperature after a head injury. This symptom results from a concussion-induced disruption in your brain’s ability to correctly perceive temperature.
Note: It is concerning if your body temperature drops below 96.5 degrees Fahrenheit. Seek immediate medical attention if it drops to 95 degrees Fahrenheit or below, as this constitutes hypothermia.
When you experience these symptoms, you can and should take steps to be as comfortable as possible. Here are some of the most effective recommendations if you’re experiencing chills or shivering:
Sometimes patients are unsure whether their shivering might actually be seizure or vice-versa. Research suggests somewhere between 10-20% of people may experience seizures following TBI, and untreated seizures require immediate medical attention.
Unlike shivering, seizures are usually accompanied by other signs like stiffening, lack of responsiveness, unusual movements and gestures, a lack of physical control, dizziness, or an inability to communicate. If you’re not sure whether you’re experiencing shivering or seizures, seek medical attention to be on the safe side.

If you’re experiencing post-concussion symptoms, including body temperature problems or other issues, that’s a clear indication that your brain function is still affected by your injury. In this case, getting the right treatment is the biggest step you can take to start feeling better. You may need a combination of treatment for the head injury, treatment for an endocrinologist for hormone regulation issues, and assistance from a psychologist for emotional symptoms.
Along with treatment, you can also take some steps on your own to manage symptoms of a concussion. Regardless of which type of thermoregulation issues you experience — those related to low body temperature, high body temperature, or both — here are some do’s and don’ts to keep in mind on your road to recovery.
Do: Exercise, because exercise increases blood flow throughout your body and brain.
Enhancing circulation through your body is excellent for cold-related symptoms, but increasing brain blood flow can also help heat-related and subjective symptoms (and most other post-concussion symptoms) by circulating oxygen-rich blood into brain tissue that’s underserved by vasculature due to head trauma.
Do: Discover which behavioral changes work for you.
As human beings, our ability to change our immediate surroundings is essential for thermoregulation. Experiment with as many different strategies as possible to get comfortable (climate control, a fan, hot or cold beverages, layering up or down, etc.) and stick with what works.
Do: Document and track your symptoms.
Writing down or logging your symptoms can help you and your healthcare provider notice patterns and trends. You can also ask your family members if they have noticed behavioral changes since your injury. They may have insights into your symptoms that you don’t.
Don’t: Overcompensate with extremes.
The prospect of a very cold shower might sound tempting if you’re burning up, but extreme temperatures often cause a rebound effect. A chilling shower signals to your body that you need to warm up, exacerbating symptoms of feeling hot afterwards. The same is true of taking a scalding hot bath if you’re feeling cold. Use gentle approaches only to avoid worsening your symptoms.
Don’t: Ignore or minimize symptoms.
All concussion-related symptoms are significant and should be heeded and discussed with a professional. Our body temperature is strongly linked to survival systems, emotional systems, and behavioral systems, so temperature-related symptoms are important, even if some say it’s “just annoying” or “not that serious.”
While achieving relief from symptoms isn’t the same as healing after a concussion, it’s still important for your wellbeing. When you feel better, you’re better able to do the things you love and you’ll feel less stressed, both of which can help you recover and boost your mental health.

People who have had TBIs can experience a range of bizarre, seemingly unrelated symptoms that persist for months or years.
If you’re experiencing these issues, you deserve to feel better. Managing symptoms day to day is fine, but long term, you’ll benefit immensely by addressing the underlying cause to recover from your brain injury.
At CognitiveFX, treatment begins with a diagnostic functional neurocognitive imaging (fNCI) scan to measure cerebral blood flow in over 60 brain regions. This shows us which areas likely suffered impairment of normal brain function.
From there, we provide individualized treatment targeted to the unique needs of each patient. Our cutting-edge, multidisciplinary approach includes neuromuscular therapy, cognitive therapy, occupational therapy, sensorimotor therapy, vestibular rehabilitation, and more. You can read more about how our treatment methods work here.
Will treatment for post-concussion syndrome reverse all your symptoms? Perhaps. It’s more likely you’ll experience rapid resolution of some symptoms and a longer recovery process for others. Each patient is unique, and some issues take longer to improve than others, which is illustrated by the patient stories we publish on our blog.
We help post-concussion patients recover from persistent symptoms every week. 95% of our patients show statistically verified restoration of brain function. To discuss your specific injury and symptoms, schedule a consultation with our team.

Alina Fong, Ph.D. is a clinical neuropsychologist and the Clinical Director and Co-Founder of Cognitive FX. She earned her Ph.D. in Clinical Neuropsychology with an emphasis in Neuroimaging from Brigham Young University, where she received the American Psychological Association Division 40 Graduate Student Research Award for her neuroimaging research. Dr. Fong has over 17 years of clinical experience treating traumatic brain injury, beginning with her work at the VA Salt Lake City Healthcare System and Utah Valley Regional Medical Center, where she directed the neurotrauma rehabilitation and sports concussion clinics. She developed the EPIC Treatment protocol and has personally overseen treatment for nearly 8,000 brain injury patients, including professional athletes from the NFL, NHL, and Olympics. She serves as Vice President of the Brain Injury Alliance of Utah, sits on the board of the United States Brain Injury Alliance, and advises PINK Concussions. Dr. Fong has authored peer-reviewed research on functional MRI and concussion treatment and has presented at over 60 medical conferences, including the Federal Interagency Conference on TBI and the American Medical Society for Sports Medicine.

Depression, one of the five stages of grief, may be the most familiar, and frustrating, feeling experienced after a traumatic brain injury (TBI) or concussion. And it’s not a fun one. Depression is a...

Emotions are expressed in many ways—through gestures, facial expressions, and the tone of our voice. When you're happy or upset, others typically recognize those emotions by looking at you and...

People who have suffered a mild traumatic brain injury (mTBI) often experience difficulties with theirpsychological and emotional health. For example, among the patients we treat at our clinic, it’s...

If you’ve recently suffered a concussion, you might be confused about when and how to return to exercise. Maybe you were told to avoid all physical activity until you feel better. But what if that...

Personality changes (or what feels like them) are common following a traumatic brain injury. Even a concussion can affect the brain long after it’s healed from the initial injury. The way we process...

Post-concussion syndrome is an “invisible” illness.
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY