A Patient’s Guide to TBI Physical Therapy
Recovering from a traumatic brain injury (TBI) often means dealing with physical symptoms, such as headaches, balance issues, weak muscles, and vision problems. These symptoms can affect every aspect...
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY
In post-concussion syndrome (PCS), a patient with a mild traumatic brain injury (mTBI) experiences persistent symptoms from the injury. If left untreated, the symptoms might last months, years, or even decades after the event.
For most patients, having PCS (or wondering if you have PCS) can mean confusion, questions, and anxiety. And even if you do know you have post-concussion syndrome, finding treatment that works is no guarantee. Experts on PCS and how it’s treated are far and few between. One of our patients went from doctor to doctor for five years before finding relief from her symptoms through our treatment program.
In this post, we hope to clarify what a good treatment program includes. We cover:
Some patients are incorrectly told they don’t have post-concussion syndrome. Others are told that it’s a permanent condition that can’t be improved with anything but time. The truth is that most patients can make significant progress under the supervision of experienced physicians and therapists.
As we discuss below, the key to recovery is an active approach to recovery rather than waiting it out or trying to mitigate a few symptoms with medication (which doesn’t address the underlying issue).
If you've experienced one or more concussions and your symptoms persist, you're not alone—and you're not imagining it. Help is available. Peer-reviewed research shows that 77% of patients treated at Cognitive FX experienced significant improvement in their post-concussion symptoms. Cognitive FX is the only post-concussion treatment clinic with third-party validated outcomes. To see if you are eligible for treatment, schedule a consultation.

All of the following are common symptoms of post-concussion syndrome:
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
As you can see, the symptoms of PCS range from cognitive symptoms, such as difficulty making decisions, to physical symptoms, such as balance problems and post-traumatic headaches. Many patients also suffer from emotional symptoms such as anxiety, depression, post-traumatic stress disorder (PTSD), and emotional lability.
Symptom severity depends on several risk factors. You’re more likely to have lasting symptoms if you’ve had multiple head injuries, but that doesn’t mean your symptoms will be more severe than for someone who only has had one.
Contrary to popular belief, loss of consciousness doesn’t increase your likelihood of having persistent symptoms. And a sport-related concussion isn’t necessarily less severe than a vehicle-related injury. What seemed like a minor head injury at the time can still cause persistent post-concussion symptoms that interfere with your daily life.
Note: If you're exploring treatment because symptoms haven't gone away, start with a clear picture of what you're dealing with. Our free concussion and PCS quiz evaluates your symptom severity, timeline, and medical history to help you understand whether you're likely to recover on your own or need targeted treatment.
It is not unusual for the symptoms of concussions to come and go, worsen over a period of time, or last for years after the initial injury. For example, you might have some symptoms that worsen with exercise or stress. Many patients find that carefully controlling their routines (things like avoiding situations known to aggravate symptoms, getting enough sleep, and eating well) results in a reduction of symptoms. But if they deviate from that routine, the symptoms come back.
The good news is that you can still see positive results even if your injury occurred years ago: If it was treatable then, it’s treatable now. Our adolescent patients with a recent injury average the same improvements as someone with an injury that’s decades old. We’ve seen patients whose injuries were 30+ years in the past make remarkable progress during and after treatment.
Has it been years since your concussion(s)? We can still help. Some of our patients visit our clinic decades after their head injury and still make a significant recovery. Contact us to schedule a consultation to discuss your situation.
The four most common causes of persistent post-concussion symptoms are neurovascular coupling dysfunction, autonomic nervous system dysfunction, vestibular dysfunction, and vision problems after the head injury. Knowing when and how these causes lead to symptoms is an important part of forming a good PCS treatment plan.
Neurovascular coupling (NVC) — the dynamic relationship between neurons and the blood vessels that supply them with oxygen and other nutrients — is behind many post-concussion symptoms. Here’s a quick breakdown of what happens to your brain during and after a concussion and why some people don’t recover as expected:
When you experience a concussion (or any TBI), your immune system causes inflammation near the site(s) of injury. The affected parts of your brain experience a temporary breakdown of tiny structures in and around those cells.
As a consequence, those cells don’t get the oxygen they need to power the signaling your brain normally does. When you try to do something that those cells govern — like remembering where you put your keys — they won’t be able to accomplish the task. Other neural pathways will then attempt to complete the process, even though it’s a less efficient path for that information to take.
For the majority of people who suffer from a concussion, symptoms usually resolve 3-6 weeks post-head trauma. We assume that’s because the brain goes back to using the best pathways for any given process (although it may just be really good at compensating for the injury). But for post-concussion syndrome patients, the brain keeps using less efficient pathways to complete tasks even after the inflammation has resolved. That suboptimal signaling is what results in long-lasting concussion symptoms.
If suboptimal signaling seems confusing to you, think of it like road traffic. A healthy brain would distribute “traffic” — i.e., the signaling and blood flow dynamics needed for a task like reading — equally along existing pathways. Suboptimal signaling is like getting stuck in a traffic jam or taking a frontage road instead of the highway. It’s inefficient and requires more “gas” to get to the same destination.
Cells impacted by post-concussion syndrome either can’t call for enough blood flow to complete the task or they call for far too much, making it harder for the brain to do its job well. Other cells in nearby regions have to do the job for them, but it’s easy for them to become overloaded.
The more your brain has to use suboptimal pathways, the more likely you are to experience symptoms. That’s why so many patients notice their symptoms worsening with overexertion. Fortunately, that’s not the end of the story: Your brain can relearn better signaling pathways during a combination of physical and cognitive therapy. We’ll explain how that works in our section on therapy for PCS.
The autonomic nervous system regulates involuntary processes throughout your body — think heart rate, blood pressure, speed of digestion, pupillary response, breathing, liver processes, and even sexual function. It’s the system that produces your “fight or flight” response (through the parasympathetic nervous system, or PNS) and your “rest and digest” state (through the sympathetic nervous system, or SNS).
A concussion can disrupt the complex dynamics between the parasympathetic and sympathetic nervous system branches. For most patients, that involves mostly sympathetic nervous system overactivity, with occasional swings toward the parasympathetic side.
It can cause many surprising symptoms throughout the body:
 Further Reading: Post-Concussion Dysautonomia
Further Reading: Post-Concussion Dysautonomia
The vestibular system, located in your inner ears, communicates with your brain to determine your position in space. It helps you feel balanced and helps your vision stay clear, especially when you’re moving or tilting your head. Think of it like neural GPS: Your brain is the phone, and your eyes, ears, and body are the three satellites needed to triangulate your position.
If a concussion disrupts healthy signaling between the brain, eyes, ears, and body, you might experience vestibular dysfunction. That can lead to balance problems, impairment of spatial awareness, dizziness, motion sensitivity, nausea, eye strain, vertigo, and even sleep problems.
Fortunately, post-concussion vestibular therapy has a high rate of success in restoring healthy function of the vestibular system.
A concussion can wreak havoc on previously healthy vision. Visiting a regular optometrist’s office doesn’t help, however, because you can have 20/20 vision and still have vision problems. That’s because a concussion impacts the way your brain and eyes work together, leading to functional vision problems. Here are some of the most common functional vision problems concussion patients experience:
|
Focusing Issues: If your eyes don’t focus quickly and easily, you might have these problems:
|
Eye teaming: If your eyes don’t converge correctly, you might have these problems:
|
|
Depth Perception: If your eyes can’t judge distances or the location of objects in relation to each other correctly, you might have these problems:
|
Eye tracking: If your eyes aren’t tracking properly, or moving accurately and easily from place to place, you might have these problems:
|
|
Overactive peripheral vision: If your brain is paying attention to too much of the activity in your peripheral vision, you might have these problems:
|
Underactive peripheral vision: If your brain is paying attention to too little of the activity in your peripheral vision, you might have these problems:
|
All of these issues are treatable with vision therapy. While some therapies can be done quickly and effectively, vision therapy often takes a few months for the full effect.
Further Reading: Vision Problems After a Concussion
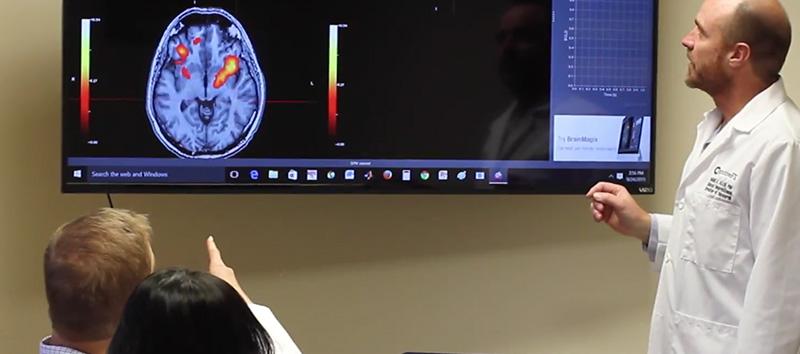
Structural MRI (magnetic resonance imaging) scans cannot detect post-concussion syndrome. In a similar vein, CT scans can’t detect PCS either. They can show tissue-related brain damage, brain bleeds, skull fractures, and the like. But post-concussion syndrome comes from a communication issue, which neither of those scans measure.
Fortunately, there is a way to detect abnormalities in your brain function after a head injury. At Cognitive FX, we use fNCI, which is short for functional neurocognitive imaging.
fNCI is a kind of functional MRI that looks at oxygenated and deoxygenated hemoglobin in the brain as it performs different cognitive tasks. By comparing blood flow in regions of your brain to a database of healthy brains, we can pinpoint which areas of your brain are affected and develop a customized treatment protocol.
Your results will be mapped to descriptions of functional skills. Here’s an example from a healthy patient:
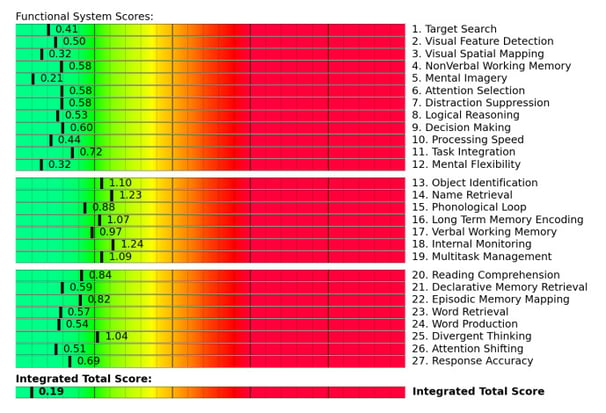
By knowing which specific regions of your brain are not functioning well, we can tailor treatment to what you need. For example, if your thalamus is underactive, it will likely benefit from Dynavision, an activity that requires quick reaction times.

The fNCI scan is one of the reasons our treatment program is so effective. We don’t have to guess which regions of your brain are underperforming based on your symptoms, which means we can confidently construct a treatment regimen specifically for your brain’s needs.
There are two treatment options for post-concussion syndrome, generally speaking: active rehabilitation (therapy) and medication. Therapy is currently the best treatment protocol for restoring healthy cognitive function. Because recovering from post-concussion syndrome typically requires multiple types of therapy, most doctors cannot offer a comprehensive rehabilitation program (it is cost-prohibitive to have so many therapists on staff unless you focus entirely on treating post-concussion syndrome).
Your alternative, medication, should be a last resort: While it doesn’t address the underlying problems, it can make certain symptoms more bearable while you pursue concussion recovery. But for many patients, even that improvement comes at a cost since many cause side effects and may make other symptoms worse.

The brain’s ability to recover via neuroplasticity is remarkable. Patients suffering from post-concussion syndrome can and do experience notably improved symptoms after active rehabilitation, assuming it is done correctly.
At Cognitive FX, we employ a combination of physical and cognitive therapy over the course of treatment designed to help the brain return to more optimal neural pathways. Doing so takes a multidisciplinary approach; we have a clinical neuropsychologist, a neuroradiologist, a neurosurgeon, a clinical psychologist, neuroscientists, neuromuscular therapists, cognitive therapists, occupational therapists, and even a neurointegration specialist on our team.
We’ve discussed general types of therapy for concussion rehabilitation in another post. Today, we’ll focus on the primary methods we use at our clinic. Before you read about each type of therapy, it’s important to understand how they all work together.
We use a three-part cycle: Prepare, activate, recover
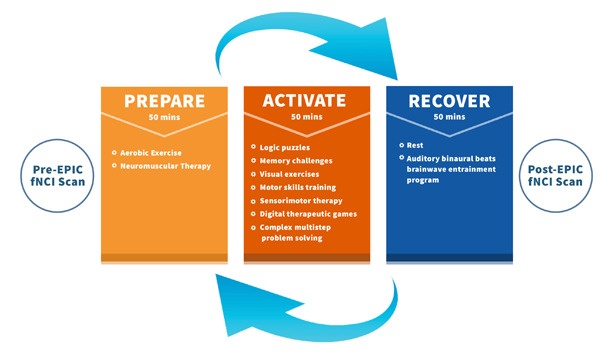
With supervised exercise, you will prepare your brain and autonomic nervous system. (For safety, patients with dizziness and exercise intolerance use stationary bikes rather than a treadmill, for example.)
Cardiovascular exercise improves cerebral blood flow and unleashes a cascade of neurochemicals (such as brain-derived neurotrophic factor, or BDNF) that help your brain adapt during therapy. It also encourages the brain and forces your brain and ANS to work together better.
The activate phase is when you complete different types of therapy that target the regions of your brain that were injured.
Finally, the recover phase gives your brain a chance to destimulate and engage your parasympathetic nervous system. For example, you might follow up a therapy session with a few minutes of resting in a dark room while listening to binaural beats (find the app here).
These breaks help your brain recover enough to continue therapy throughout the day.
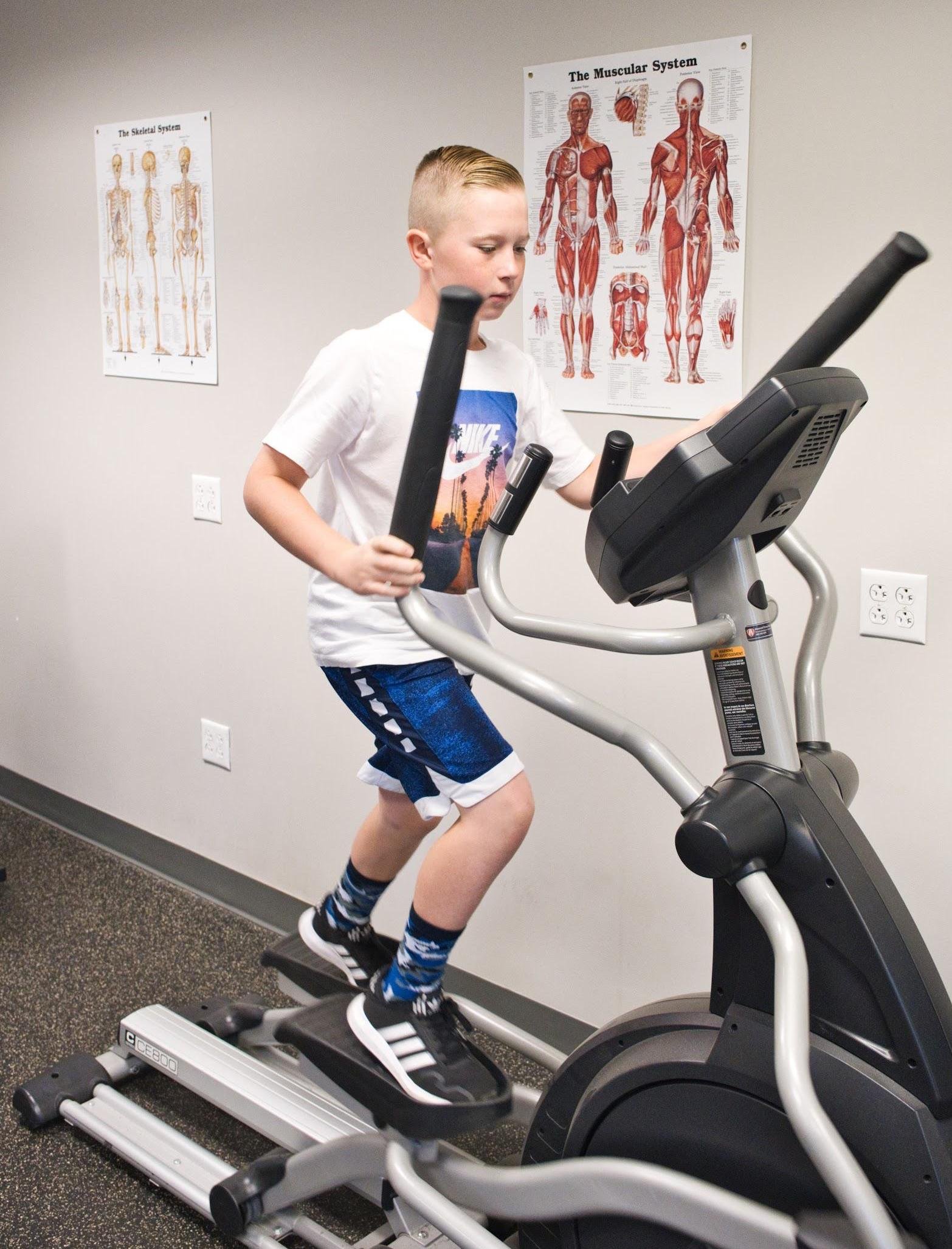
Our neuromuscular therapists oversee the aerobic exercise portion of your treatment, as well as provide physical therapy and massage therapy (particularly on the neck to help relieve tension and improve headache and vision symptoms).
They combine physical activity with cognitive challenges and hand-eye coordination exercises. You might find yourself balancing on a Bosu ball, playing catch, and naming countries for each letter of the alphabet — all at the same time!
Further reading: Physical Therapy for Post-Concussion Syndrome
Our cognitive and occupational therapists are focused on restoring and improving skills like memory, attention, decision making, and reasoning. While occupational therapy is designed to help you cope with symptoms and regain as many “real world” skills as possible, we’re also trying to rehabilitate your neurovascular coupling at the same time so that your symptom burden is lower and your brain is healthier.
Some examples from cognitive therapy include solving logic puzzles, identifying word patterns while listening to distracting sounds, memorizing pictures, and more.
Further reading: Cognitive Therapy for Post-Concussion Cognitive Deficits
Vestibular therapy involves gaze stabilization exercises along with movement and balance exercises. Which ones depend on the needs of each patient.
For example, you might catch a ball while standing on a balance board, or walk in a Figure 8 pattern around obstacles all while keeping your eyes focused on a point (called the Infinity Walk).
Further reading: Vestibular Therapy for Post-Concussion Syndrome
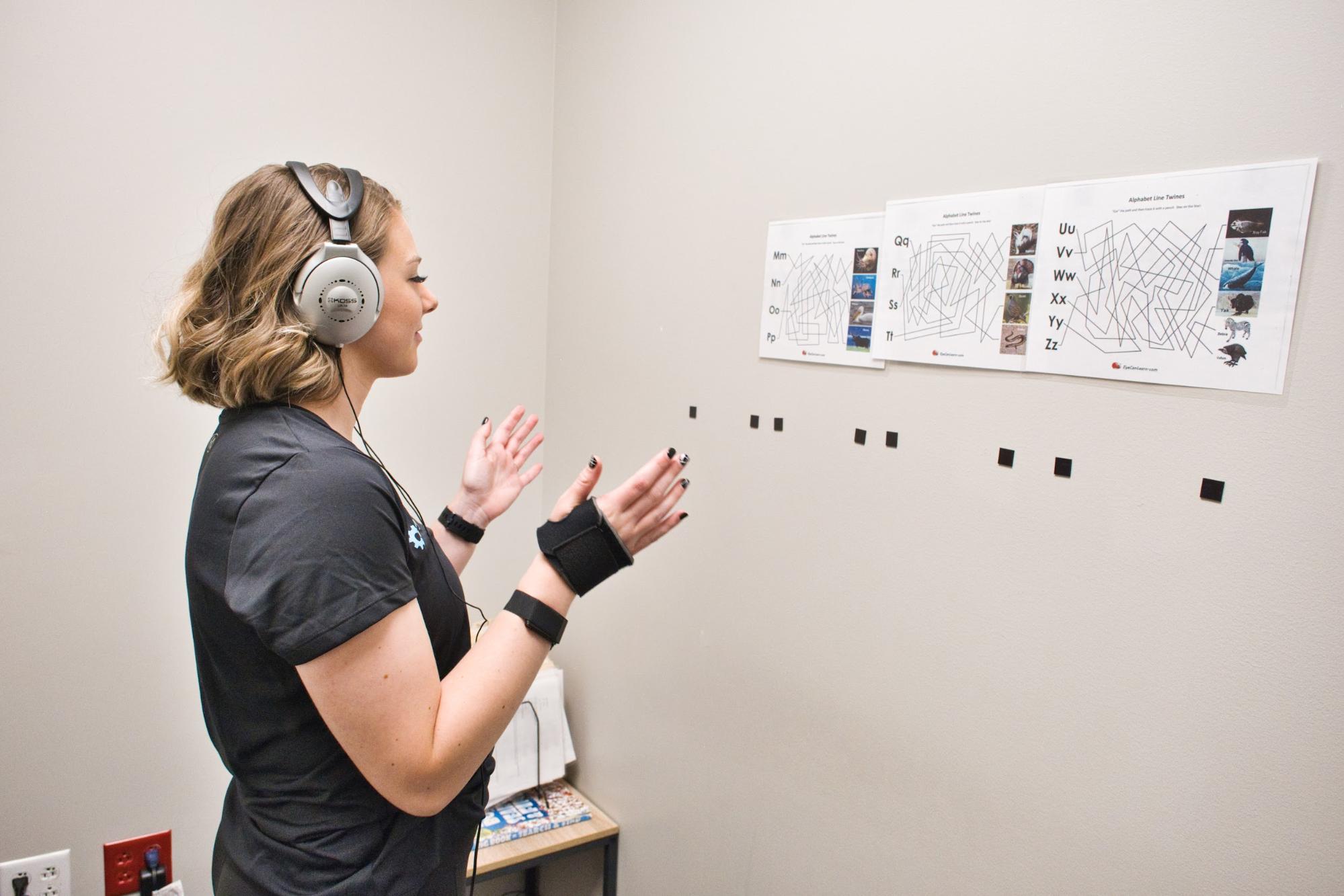
In sensorimotor therapy, patients move according to simple patterns in time to a metronome. When they’re able to do that, the therapists add in cognitive and vision work as well.
For example, you might be clapping and stomping in time to a beat while completing a visual search puzzle at the same time. These activities challenge the brain in unique ways, encouraging neuroplasticity to occur.
During each week of treatment, all patients meet at least twice with a clinical psychologist. During these sessions, your healthcare provider will evaluate your mental health and make recommendations for follow-up neuropsychological care, if needed.
If you suffer from clinical anxiety, for example, you might receive a referral for cognitive behavioral therapy (CBT), which is a highly effective treatment for that condition. That said, many patients note significant improvements in their emotional symptoms after treatment simply because their brains are functioning better.
In addition, patients attend a session on mindfulness and how they can use those techniques to help their brains rest and recuperate from the difficulties of recovery and daily life.
Further reading: Cognitive Behavioral Therapy for Post-Injury Mental Health Difficulties
While we offer some vision therapy during our treatment program, you will likely need ongoing vision therapy (also known as neuro-optometric rehabilitation) after visiting our clinic. If that’s the case for you, we’ll help you identify a knowledgeable therapy provider in your area.
But while you’re here, we incorporate Dynavision, visual tracking exercises, the Brock String, and some other computerized technologies into treatment.
Want to give rehabilitation a try? Schedule a consultation with our experts on post-concussion syndrome.

As you’ve likely experienced, many doctors prescribe medication to help manage the symptoms of post-concussive syndrome without addressing their cause. While some medications are necessary to keep you functioning, others only serve to mask the root issue.
Most patients arrive at our clinic on a number of medications designed to control their symptoms. We’ve seen it all — antidepressants, nausea meds, headache and migraine medication, blood pressure medication, pain prescriptions… But the reality is that most of our patients don’t attribute much (if any) improvement in their condition to those medications. In fact, we can’t name a single medication that is consistently reported as helpful!
Unfortunately, most medications were never tested on patients with a brain injury. But as you’ve seen earlier in this post, post-concussion syndrome can cause metabolic changes (gut motility, blood pressure, liver function, and more). Plus, injured patients often see a marked increase in blood flow to the brain. All of those realities change how much medication you metabolize and which parts of your body and brain it interacts with. As a result, post-concussion syndrome patients are much more likely to experience negative side effects with medication use.
And that doesn’t even take into consideration the extra toll taking multiple medications has on the liver (which as we mentioned before is already under extra stress from your condition).
So does that mean you shouldn’t ever take medications? Not at all. Certain medications truly are necessary and helpful. For example, if you develop hypothyroidism, then taking thyroid medication will help your well-being tremendously. There are also some supplements (like melatonin for sleep or vitamin C for general health) that can help you.
That said, we do recommend caution regarding which and how many medications you’re taking. We also recommend looking up possible drug interactions between your medications and food, since most doctors often forget to mention them.
For a full discussion of this topic, see our post on medications for post-concussion syndrome.

If you’ve decided to pursue rehabilitation for post-concussion syndrome, then the next step is to decide where you will go for treatment. Obviously, you have to consider things like location, cost, and time.
But there are other factors surrounding the quality of the health care you receive that you can use to make a good decision. For example, the best clinics have the characteristics listed in our post-concussion treatment center checklist:

It’s important to make sure ahead of time that the clinic has the resources, staff, and program needed for the neurorehabilitation of persistent symptoms.
Further reading: How to Find the Best Post-Concussion Clinic Near You
Not every clinic or practicing doctor has these resources. Most general physicians, pediatric doctors, and neurology practitioners can only offer medication (and sometimes referrals). Sports medicine practitioners may be able to offer physical and vestibular therapy, but not in combination with other types of cognitive therapy. A psychiatry practitioner can offer counseling and medication for emotional symptoms, but can’t fix the physical changes causing the post-concussion syndrome.
Further reading: What a Neurologist Can (and Can’t) Do for Post-Concussion Syndrome and The Types of Doctors Involved in PCS Care

Many post-concussion syndrome patients suffer for years before they discover the reason for their illness. Even then, it can be difficult to get adequate treatment for the condition — neuroscience and clinical research on PCS is still new, and many clinicians aren’t aware of best practices like neuroplasticity-based post-concussion syndrome treatment.
No matter how long it’s been since your injury, there’s still hope for recovery. With the right treatment regimen, a post-concussion syndrome diagnosis is not a life sentence. We’ve had patients from all over the United States and Europe visit our clinic because they knew we would take good care of them.
If you want to take the next steps toward recovery, schedule a consultation with our team. We’ll equip you with the resources you need to move forward.

Alina Fong, Ph.D. is a clinical neuropsychologist and the Clinical Director and Co-Founder of Cognitive FX. She earned her Ph.D. in Clinical Neuropsychology with an emphasis in Neuroimaging from Brigham Young University, where she received the American Psychological Association Division 40 Graduate Student Research Award for her neuroimaging research. Dr. Fong has over 17 years of clinical experience treating traumatic brain injury, beginning with her work at the VA Salt Lake City Healthcare System and Utah Valley Regional Medical Center, where she directed the neurotrauma rehabilitation and sports concussion clinics. She developed the EPIC Treatment protocol and has personally overseen treatment for nearly 8,000 brain injury patients, including professional athletes from the NFL, NHL, and Olympics. She serves as Vice President of the Brain Injury Alliance of Utah, sits on the board of the United States Brain Injury Alliance, and advises PINK Concussions. Dr. Fong has authored peer-reviewed research on functional MRI and concussion treatment and has presented at over 60 medical conferences, including the Federal Interagency Conference on TBI and the American Medical Society for Sports Medicine.

Recovering from a traumatic brain injury (TBI) often means dealing with physical symptoms, such as headaches, balance issues, weak muscles, and vision problems. These symptoms can affect every aspect...

Loss of taste and smell featured heavily in the news during the COVID-19 pandemic as one of the first signs of infection. But this is not the only condition that may lead to loss of smell. You could...

If you’ve had a severe or mild traumatic brain injury (severe TBI or mild TBI) that’s left you with post-concussion syndrome (PCS), just thinking can be taxing. Cognitive health is “the ability to...

There is no exact time frame for recovering from a mild traumatic brain injury (mTBI), otherwise known as a concussion. The majority of people who sustain an acute concussion recover within a few...
Oxygen is good for the brain. A lack of oxygen is bad for the brain. So is getting more than normal levels of oxygen better for the brain?

Health care providers often set low expectations after a severe traumatic brain injury (TBI). When patients exceed those expectations, it’s cause for joy. At the same time, it’s disheartening to be...
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY