Can an MRI Detect Post-Concussion Syndrome?

A regular MRI (magnetic resonance imaging) looks at brain structure and integrity. While it helpful for diagnosing structural brain damage, it can’t often be used to detect post-concussion syndrome (PCS). However, a specialized form of MRI called functional neurocognitive imaging (fNCI) can detect PCS.
We understand that managing care and recovery from PCS can often be confusing. Many patients are told to get an MRI after their concussion symptoms linger, but the truth is that an MRI will not give them the definitive diagnosis they seek. Here, we explain why a traditional MRI can’t detect post-concussion syndrome and then explain what you can do to get a diagnosis instead.
For your convenience, we’ve included hyperlinks to all the major questions we answer in this post:
- Can an MRI Detect Post-Concussion Syndrome?
- What Can Detect Post-Concussion Syndrome?
- Do I Have Post-Concussion Syndrome?
- Is Post-Concussion Syndrome Treatable?
Note: If you've experienced one or more concussions and your symptoms persist, you're not alone—and you're not imagining it. Help is available. Peer-reviewed research shows that 77% of patients treated at Cognitive FX experienced significant improvement in their post-concussion symptoms. Cognitive FX is the only post-concussion treatment clinic with third-party validated outcomes. To see if you are eligible for treatment, schedule a consultation.
Can an MRI Detect Post-Concussion Syndrome?
A regular MRI usually cannot be used to detect post-concussion syndrome. A regular MRI detects structural damage to the brain, but PCS is not caused by structural damage. Because of this, many individuals with PCS are told they’re fine and that the symptoms are all in their heads — due to normal MRI results. As we know now, that’s simply untrue.
To understand why that’s the case, let’s talk about what an MRI can see.
A regular MRI uses magnets to look at protons (positively charged particles) in water. In the case of a brain MRI, that means looking at soft tissue in your head. It doesn’t show bone well, but it will show the structure of your brain, since that’s where the water is. The protons in water respond to a magnetic field differently based on what kind of tissue they’re in, so we can look at those differences to determine what kind of tissue is present and how that tissue is shaped. For this reason, a regular MRI is powerful at detecting serious issues such as strokes, aneurysms, tumors, bleeding in the brain, and so forth.
But mild traumatic brain injuries do not show up on standard brain imaging tests because the tissue is not damaged in an obvious way. Post-concussion syndrome impacts the ability of neurons (brain cells) to signal for the right amount of blood to accomplish certain processes (among other things) but does not cause structural degradation to the cells themselves.
Imagine a struggling company. If you look only at the outside of that company, everything looks great — employees put in their eight-hour days, computers are running, and the lights are on. But if you go inside, you might observe that employees aren’t getting their work done, communication is terrible, or budgets aren’t being met. You couldn’t see the dysfunction from the outside, but if you monitored communications, it would become clear that something was very wrong.
Trying to use a regular MRI to detect post-concussion syndrome is like looking at the exterior of the company building. The “MRI view” would tell you if the company is still afloat or if they have shut down. It wouldn’t show you the communication breakdowns happening inside. Fortunately, there is a test that takes a more detailed look at how communication is going in your brain: an fNCI scan.
fNCI: The Scan That Can Detect Post-Concussion Syndrome
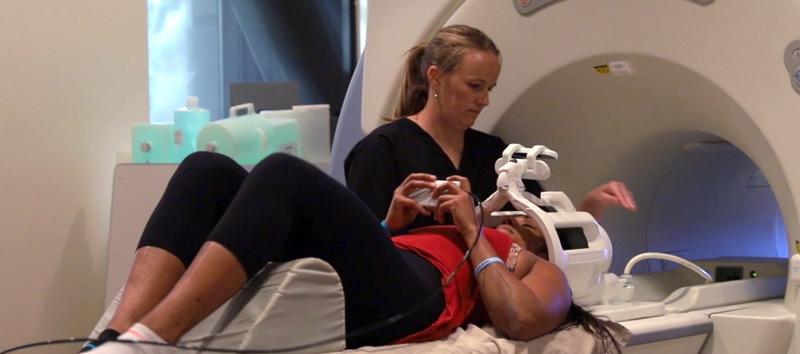
A fNCI scan (functional Neurocognitive Imaging) is a specialized scan that can detect post-concussion syndrome. Since fNCI can provide information about how oxygen is carried to the different regions of your brain, it can detect the “dysfunctional communication” that is caused by PCS.
With fNCI, near-real-time changes in blood flow are measured while a patient completes several different cognitive tests. This is especially important for detecting post-concussive syndrome because PCS symptoms often worsen under cognitive load.
fNCI uses an fMRI (functional MRI) to look at blood flow to the brain in real time and monitor changes. fMRIs are famous for helping scientists “see” brain activity. It can do this by monitoring which parts of the brain become more active, i.e. have increased blood flow, when someone does cognitive tasks (such as remembering a loved one, recalling a distant memory, or solving math problems without writing them down).
fNCI looks at something called neurovascular coupling (NVC). NVC is the connection between neurons and the blood vessels that bring them oxygen.
With PCS, the connection between the brain cells and the blood vessels that supply them is disturbed, making it difficult for certain cells to work properly. Some clusters of neurons may be getting too little blood flow, while others may be getting too much. This is because of damage the neurons themselves sustained during or after the concussion.
That inappropriate oxygen supply means that when you’re trying to accomplish a task, it may be more difficult to stay focused, you might become fatigued quickly, or perhaps you just can’t seem to recall the name of the person with whom you’re speaking. The neurons that facilitate these activities are slow and not as responsive as they should be due to the concussion. They aren't sending the correct signal to receive enough oxygen or 'power' for normal cognitive function.
Irregularities in the amount of blood being used by different parts of the brain can be an indication of brain damage caused by a mild head injury. These irregularities are identified by comparing fNCI scans with a database of fNCI scans from normal patients.
At Cognitive FX, we’ve built up a database of fNCI scans from patients who have never had a brain injury and who do not have symptoms of PCS (in other words, they have apparently normal brain function). This database is extremely valuable in identifying where and how PCS patients’ brains deviate from the norm.
The ability to pinpoint problems in neurovascular coupling is very important for our patients' recoveries. Our database allows us to calculate if each region of the brain is working correctly or if it is getting too much or too little blood flow and how far each region is from “normal.” This gets to the heart of any cognitive problems caused by PCS and allows each Cognitive FX treatment regimen to be tailored to the needs of each patient.
Note: To see if fNCI is an option for you, sign up for a consultation.
Do I Have Post-Concussion Syndrome?

If you have post-concussion syndrome, it can be difficult to get an accurate diagnosis — hence the power of a fNCI scan. But neuroimaging is not necessarily the first step for someone who suspects they have post-concussive syndrome.
It’s important to first discuss your history and symptoms with a physician. Post-concussion syndrome symptoms overlap with other conditions, including brain tumor symptoms, Lyme disease, PTSD, and more. Your symptoms are an important initial indicator that you may have PCS, but there are other factors that must be considered as well.
The main criteria for diagnosing PCS are:
- History of one or more head injuries (does not require loss of consciousness)
- PCS symptoms
- Persistent symptoms for at least 6 weeks after a concussion.
All of the following are symptoms of post-concussion syndrome:
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
If you determine during your consultation that PCS is a likely diagnosis for your condition, then an fNCI is the next best step. Not only is an fNCI one of the best diagnostic tools for PCS, but the results also guide treatment and recovery for the patient.
Schedule a consultation to see if fNCI could help you on your road to recovery from a mild TBI.
Should I Get an MRI If I Think I Have PCS?
Your physician may have ordered an MRI for you, or maybe you’ve completed one and are awaiting the results. Either way, an MRI is not a waste! Conventional imaging such as MRI is a common part of health care after head trauma or with the presentation of post-concussion symptoms to rule out structural damage or other conditions.
Regular MRIs can be lifesaving in their ability to detect bleeding in the brain, strokes, tumors, and other conditions. They provide detailed views of soft tissues that cannot be captured using an X-ray or CT scan. A structural MRI is not a waste; it just might not be the only test you need.
Is Post-Concussion Syndrome Treatable?
Yes, post-concussion syndrome is treatable!
There are two main ways that doctors treat post-concussion syndrome: medication (to help manage symptoms) and active rehabilitation (to help repair concussion damage).
Active rehabilitation, which is what we provide at Cognitive FX, should always be tried first. Active rehabilitation helps repair damage from brain trauma, while medication can only mask or minimize symptoms.
Active rehabilitation for post-concussion syndrome is fairly new, but it’s a significant improvement over previous treatment guidelines (think “rest, hydration, and medication”).
We now know that active rehabilitation is a much better path to recovery. Think of it this way: would you tell someone with a broken arm to go home and “wait it out”? Of course not! You would cast the arm, allow it to heal, and then complete physical therapy to aid in the proper recovery of bone, muscle, and ligament.
In the same way, physical and cognitive therapy is an important step in rehabilitating mTBI patients. But because it is fairly new, many doctors aren’t able to offer a comprehensive active rehabilitation program.

At Cognitive FX, we employ a combination of physical and cognitive therapy designed to push the brain into rewiring itself. Doing so takes a multidisciplinary approach; we have a clinical neuropsychologist, a neuroradiologist, a neurosurgeon, a clinical psychologist, several neuromuscular therapists, several neurocognitive therapists, several occupational therapists, and two DynaVision specialists on our team.
If you’re interested in learning how we use neuroplasticity to aid post-concussion syndrome recovery, you can read our post on neuroplasticity and concussions.
Conclusion
An important aspect of recovery involves the proper detection of post-concussion syndrome. Completing an fNCI scan would definitively show whether or not you have post-concussion syndrome.
If you think you may be suffering from post-concussion syndrome, schedule a consultation with our team. We can help you determine if an fNCI and active rehabilitation are the right next steps for you.

About the author
Dr. Mark Allen, Ph.D.Dr. Mark D. Allen holds a Ph.D. in Cognitive Science from Johns Hopkins University and received post-doctoral training in Cognitive Neuroscience and Functional Neuroimaging at the University of Washington. As a co-founder of Cognitive Fx, he played a pivotal role in establishing the unique and exceptional treatment approach. Dr. Allen is renowned for his pioneering work in adapting fMRI for clinical use. His contributions encompass neuroimaging biomarkers development for post-concussion diagnosis and innovative research into the pathophysiology of chronic post-concussion symptoms. He's conducted over 10,000 individualized fMRI patient assessments and crafted a high-intensity interval training program for neuronal and cerebrovascular recovery. Dr. Allen has also co-engineered a machine learning-based neuroanatomical discovery tool and advanced fMRI analysis techniques, ensuring more reliable analysis for concussion patients.