Brain fog is one of the most common symptoms of concussions and post-concussion syndrome (PCS). Some people experience brain fog immediately after a concussion; for others, it might come days, weeks, or even months later (if it’s a result of your brain slowly adapting to dysfunction caused by a concussion, which we’ll explain in detail later in this post.) And, for some people, brain fog comes and goes, depending on the circumstances.
Perhaps you’ve questioned if it’s normal. Maybe people have told you they experience brain fog too, and it’s nothing to worry about.
While it’s possible they’ve experienced something similar due to other medical issues or temporary, situational causes (like being sleep-deprived), brain fog from a concussion is different. It has specific neurological causes. You’re not imagining things, and it’s not happening because you’re not paying enough attention or being lazy.
You probably have questions about why it’s happening, and most importantly — will it go away? In this post, we’ll explain what causes brain fog after a concussion, how it can affect you, and what you can do about it.
Note: If you’re experiencing brain fog and other symptoms that won’t go away after a concussion, we can help. Peer-reviewed research shows that 77% of patients treated at Cognitive FX experienced significant improvement in their post-concussion symptoms. Cognitive FX is the only post-concussion treatment clinic with third-party validated outcomes. To see if you are eligible for treatment, schedule a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
What Is Post-Concussion Brain Fog?
Post-concussion brain fog is a phrase used to describe cognitive symptoms that people experience after a concussion, including difficulty concentrating, slowness in thinking, and trouble remembering and learning new information.
Brain fog is one of the most common symptoms we see in patients who come to us for post-concussion syndrome treatment. Here are a few ways they’ve described the experience:
- It’s like I’m seeing the world through a haze.
- I just can’t process everything.
- I feel like my thinking is slower than it used to be.
- I can’t keep up.
- It’s like there’s molasses in my brain.
- I feel like I’m running in sand.
Brain fog most commonly happens when you’re putting more demands on your brain. It can happen in social situations, such as when you’re trying to have a conversation and there’s a lot of noise and activity around you.
Tasks like reading, using the computer, or even just being in a visually busy environment are common triggers for brain fog because those tasks involve about 50-80% of our brains. Being in pain (having a bad headache, for example) also might result in foggy thinking.
Why? What causes post-concussion brain fog? The simple answer is that key areas of the brain aren’t functioning efficiently anymore. It feels like your brain is slower because it is slower. It’s using workarounds and draining resources to do things that used to be easy.
Where Does Post-Concussion Brain Fog Come From?
A concussion, or mild traumatic brain injury (mTBI), is an injury to the brain that results from an impact to the head or from any jolting movement that causes the head to whip back or around suddenly. The force from that motion or impact causes the brain to smash into the skull, possibly leading to inflammation, bruising, and disruption of communication within the brain.
Areas of the brain are connected by billions of nerve cells that communicate with each other through electrochemical signals. Blood vessels supply oxygen to brain cells so that they have enough energy to send those signals to do the work they are being asked to do.
When healthy, these individual parts work together like a well-orchestrated symphony, producing the beautiful music of life, emotion, and higher-order thinking. When any part of the brain is affected by a brain injury, it’s as if one of the instruments in the symphony is horribly out of tune (or even missing), and everybody hears it. It disrupts the entire performance.
The two biggest sources of brain fog after a concussion are hypoactivation and hyperactivation. A second concussion (and third, fourth, and so on) can make these worse and increase your chances of having problems.
Inefficiency in the Brain (Hypoactivation)

We can use the example of a severe thunderstorm to explain what happens in the brain during and after a concussion.
Imagine that you need to drive to another city right after a bad storm. Some roads are flooding. Trees are down, blocking more roads and causing power outages. As a result, you have to drive slower. You have to backtrack to find roads that are still open. A trip that normally takes you 30 minutes has turned into a 3-hour ordeal. It’s inefficient, stressful, and exhausting.
That is similar to what happens in the brain after a concussion. Post-concussion inflammation and axonal shearing (rotational tearing of nerve fibers in the brain) can prevent certain regions from getting the resources (like oxygen) they need to complete a task. Sometimes the communication signals are disrupted (like traffic lights being out), so maybe the call for oxygen never even goes out. As a result, the brain routes around affected regions, doubling up in healthier areas that already have their own tasks to handle.
In many cases, these effects are only temporary. Like flood waters receding, the pathways open again, and efficient communication and blood flow gradually resume.
But in some cases, the brain decides the road is washed out permanently, and it abandons the old route. It persists in using the alternate routes. The trouble is, those new routes continue to be much slower and require a lot of energy.
The basal ganglia, for example, can easily cause brain fog if affected by a concussion. The basal ganglia helps us coordinate both how the brain processes information (such as sound and sight) as well as physical movement. It also helps us perform habitual actions that we’ve already learned and don’t usually have to think about (such as opening a door) and new actions (such as learning a new dance step).
But if your basal ganglia is hypoactivated — meaning it’s not doing its fair share of the work — then the rest of your brain will work too hard. Eventually, that results in a foggy brain.
System Overload (Hyperactivation)
With hyperactivation, an area of the brain is “on” too much. It’s working too hard or it’s trying to do too much, exhausting your limited supply of energy.
For example, consider the frontal cortex. We use areas of it (called “executive areas”) to plan and reason through things. If that area is hyperactivating because it’s trying to do the work of hypoactivating areas plus its own, it never takes a break. It’s like leaving a light on in your house all day, every day. It’s going to constantly drain energy, leaving you tired and with less energy to think clearly.
To sum it up: Areas of the brain might be working inefficiently, overworking, or both. In any case, the brain has to work a lot harder than it used to. It’s not only slower, but it’s also using more energy. Sometimes, there’s not enough energy to finish a task, and it just gives up. It’s out of fuel. This is the core source of post-concussion brain fog.
Other Possibilities
If you’ve been experiencing persistent brain fog that isn’t going away — even if it’s intermittent — it’s important to find the root cause to treat it. Let’s briefly look at a few of the other common causes of brain fog.
- Hormonal dysfunction, especially hypothyroidism, is one of the more common culprits. Head trauma can damage the pituitary gland or the hypothalamus, which would cause hormonal dysfunction. Hormonal changes during pregnancy and menopause can also lead to brain fog. In any case, it’s important to get your hormone levels tested and seek treatment accordingly.
- Poor sleep quality is another possible cause of brain fog. Changes in the brain from a concussion can interfere with sleep quality, or they could be related to other problems. Either way, your brain needs sleep to function, so it’s worth troubleshooting until your sleep improves.
- Food and environmental allergies cause brain fog in some people.
- Vitamin B-12 deficiency or anemia can also cause brain fog.
One clue that your symptoms are from a concussion and not another source is that you can’t predict what’s going to trigger them. For example, if your brain fog happens after you only get 4 hours of sleep at night, you can tie that episode to lack of sleep.
But if you’re regularly getting a full night’s sleep and brain fog hits seemingly out of the blue several times a day or week, it could be from post-concussion syndrome.
Note: If you’re experiencing brain fog and other symptoms of concussion that won’t go away after a concussion, we can help. On average, our patients improve by 75% after treatment. To learn about diagnosis and treatment options, schedule a consultation.
Concurrent Symptoms with Brain Fog: Why Do They Happen?

Brain fog rarely occurs as an isolated symptom of a concussion. It’s often one of many, and patients often notice that they experience brain fog with another concussion symptom (or more). In this section, we look at common pairings and briefly discuss what causes them:
Brain Fog, Headaches, and Other Physical Pain
Frequent headaches are one of the most common and persistent symptoms of a concussion. We discuss post-concussion headaches in detail in this post.
One of the most common reasons for concussion headaches is that the autonomic nervous system (ANS) is malfunctioning. The ANS controls things like body temperature, blood pressure, and heart rate. It might be sending too much blood into the brain and not removing it quickly enough. This causes a headache that feels like a band tightening around your head, or a feeling of strong pressure.
Neck tightness and tension can also prompt the ANS to send too much blood into the brain, leading to headaches and brain fog (and, of course, neck pain).
Basically, any time that we experience physical pain, our brain is going to be more focused on that pain. The energy that the brain does have is going to be diverted from cognitive function to dealing with that pain.
Brain Fog and Depression
It’s very common for patients to come to our clinic with a depression diagnosis. We’ve found that about 82% of the patients who come to us for post-concussion syndrome treatment list depression, anxiety, and personality changes as their main symptoms.
Why is that?
For one thing, post-concussion syndrome and depression symptoms often overlap. It can be difficult for general practitioners to differentiate between them. The conditions might coexist independently of each other, but changes in the brain due to a concussion can actually cause depression.
Research shows that problems in the thalamus and hippocampus can lead to depression. The thalamus helps process sensory information, which can affect our feelings and behavioral reactions.
The hippocampus attaches emotional components to memories and can be affected by stress hormones. The prefrontal cortex also helps regulate emotions, so if this area is experiencing concussion-related problems, it can contribute to depression.
In addition, life is just harder after a concussion. People are often in pain. They might have to restrict their activities. Even normal activities like going out to lunch or to a movie might suddenly be intolerable. They often disconnect from their social networks and become isolated. Drastic lifestyle changes like this can certainly lead to situational depression.
For some patients, depression was a pre-existing condition. Those patients usually tell us that their depression got worse after the concussion. They also seem to experience more severe depression than patients who were not previously depressed.
At Cognitive FX, we have a clinical psychologist on staff to help patients during treatment, and we can schedule additional meetings for those who need them.
Brain Fog and Memory Loss
Dysfunction in several key areas of the brain can cause memory problems and brain fog.
- The prefrontal cortex (the area in the front of your brain, behind the forehead) processes working memory. It can only hold a few pieces of information at a time for about one minute. The hippocampus needs to file that information away in long-term memory to keep it. If the brain doesn’t have enough energy (because it’s being depleted by other malfunctioning systems), it can’t send those short-term memories to storage. That means you’re only going to remember something for 60 seconds or so, and then your brain will delete it.
- The thalamus collects, screens, and relays sensory information to other parts of the brain. If the thalamus isn’t working properly, your brain isn’t screening out the unimportant information. It’s working hard trying to remember everything it sees, hears, and senses, and it just can’t do that. Additionally, recent research indicates that the thalamus also plays a role in learning and short-term memory transfer.
- The basal ganglia helps us plan, process, and coordinate physical movement. Normally, we can simultaneously do things and remember things. However, if the basal ganglia isn’t working properly, it draws a lot of energy from other parts of the brain just to maintain our many physical movements. It also means that it’s much more difficult to physically do something and remember things at the same time.
Brain Fog and Fatigue

Fatigue is almost always associated with brain fog. It can be hard to figure out where it’s coming from because there are so many possible causes. (Read more about post-concussion syndrome and fatigue in this post.) Both physical and mental fatigue can contribute to brain fog.
Fatigue From Poor Sleep Quality
Sleep problems are a very common source of fatigue and brain fog. Some of our patients suffer from hypersomnia, meaning they sleep more than 12 hours per day but still feel tired during the day. Others suffer from insomnia.
The short explanation for this is that several areas of the brain need to work together to induce restorative sleep. If one area is not working right, often the thalamus, then the process is constantly disrupted. You might spend a lot of time in bed, but you’re going to wake up tired, and your cognitive function is not going to be great. Many of our patients find themselves needing to take long naps every day just to try to clear their heads or get through the day.
Sleep apnea can also arise as a result of a brain injury. People with sleep apnea stop breathing periodically during the night. Brain injury can also cause changes in our breathing. Instead of diaphragmatic breathing (“belly breathing”), many post-concussive patients do more breathing from the chest.
Sleep apnea and shallow breathing both result in the brain not getting enough oxygen during sleep. Therefore, sleep is less restorative. If you’re having sleep disturbances and fatigue, you might want to read our blog about post-concussion sleep for a more detailed explanation and tactics you can try for better rest.
Fight or Flight Response
The sympathetic nervous system is part of the autonomic nervous system. It activates the body’s “fight or flight” mechanism. It raises your blood pressure and gives you a shot of adrenaline in a seemingly dangerous situation, such as when a deer darts out in front of you while you’re driving.
Sometimes after a brain injury, the sympathetic nervous system stays hyperactivated, resulting in the feeling of constantly being on high alert. This uses a lot of energy and is going to cause fatigue.
Brain Fog and Vision Problems
Common vision problems our patients report are blurry vision, difficulty focusing or reading, light sensitivity, and problems with peripheral vision, among others. Patients might not experience these problems all the time. They might only notice them after trying to use a computer or after reading for awhile, for example.
Vision tasks require a huge amount of brain function, and if any of the areas of the brain that are involved in that process aren’t functioning correctly, the brain’s energy is going to be rapidly depleted. These problems can also induce other post-concussion symptoms such as dizziness, feelings of overwhelm, and headaches.
Brain Fog and Dizziness
Dizziness is often a result of a vestibular disorder. The vestibular system is located in the inner ear. It senses motion and our position in space. When you look up or down or move around, the vestibular system senses that and communicates with other areas of the brain.
If your vestibular system is malfunctioning, it won’t give your brain accurate information about your bodily position and movements. Problems also result when the information from the vestibular system conflicts with information from another system, such as the visual system. This can lead to dizziness or vertigo, balance problems, headaches, and fatigue. If you’re experiencing severe symptoms such as these, seek medical attention.
Brain Fog and Hormonal Disorders
The areas of the brain that regulate our hormones are the pituitary gland and the hypothalamus. These can be damaged by a head injury, resulting in inadequate function.
The pituitary interacts with the endocrine system to increase or decrease hormone production. These hormones help regulate our bodily functions (including growth and energy use) and control our responses to stress.
Hypothyroidism is a common hormonal disorder that can result from damage to the pituitary. Brain fog and memory problems are among its symptoms.
Brain Fog and Exercise Difficulties

We often see patients who complain of brain fog coming on during or after exercise. It might hit right away, hours later, or even a day later. (If you have questions about when it’s ok to exercise after a concussion or why exercising makes your symptoms worse, this post breaks it down into greater detail.)
The autonomic nervous system controls our heart rate, blood pressure, breathing, and temperature. When we exercise, our heart rate, breathing, and blood pressure need to work together. If they’re off in any way, we’ll feel it via symptoms such as headaches, lightheadedness, and brain fog during or after physical activity.
Many of the patients we’ve seen with ANS dysregulation don’t breathe deeply enough while exercising. This type of breathing could add nausea to the mix of symptoms related to exercise (explained in more detail below).
Brain Fog and Nausea
Nausea can be caused by improper breathing while exercising or at rest. The technical term for this is respiratory acidosis. Basically, incorrect breathing patterns (sometimes due to brain injury) lead to excessive amounts of carbon dioxide in the blood. The body can’t eliminate it as it should, resulting in nausea.
Vestibular disorders could also be the culprit. Think of what happens when you get seasick on a boat. If you’re used to being on solid ground, your brain and your eyes are confused by these conflicting messages about the position of your body and the movement you’re experiencing. It makes you nauseated.
Some of our patients with vestibular problems tell us they have to be the driver if they’re traveling in a car. Somehow, it helps their brain connect and accept the messages without resulting in nausea.
Patients with thalamus dysfunction might be overwhelmed in visually busy environments if their thalamus isn’t filtering information as it should, leading to nausea.
Similarly, someone with overactive peripheral vision, a common post-concussion vision problem, can get motion sickness and nausea in a visually busy environment. Their brains are taking in too much information through the visual process.
What Can I Do to Get Rid of Brain Fog?
Some patients come to us and say their brain fog really isn’t that bad. But when we dig deeper, we see they’re compensating for it in some way. Or maybe their injury was so long ago that they’ve gotten used to it, and it just seems normal to them.
On the other hand, some are having so much trouble that they’re unable to work, or their productivity is drastically reduced. They are desperately seeking a solution.
So, how do you get rid of brain fog? Will it ever go away?
First, we’ll look at a few things patients often do or try. Then, we’ll discuss a few strategies that can really help.
Things People Do to Cope with Brain Fog

If you didn’t get enough sleep last night but you still have to go to work in the morning, you might turn to some kind of stimulant to perk yourself up: a very large coffee, maybe with a sugary treat, to give yourself an energy boost.
We often see patients resorting to the same behaviors to try to cope with their brain fog. They turn to stimulants, supplements, and sometimes medication to try to clear the fog. Unfortunately, what often happens is that it helps for a short time, but then they crash afterward. Just like that sugar high leaves you falling asleep at your desk after it wears off, this strategy usually backfires.
Other patients adapt their lifestyles to try to avoid anything that triggers their brain fog. If they notice that being in noisy, crowded spaces induces it, they start to avoid noisy, crowded spaces. If reading for long periods brings it on, they read less and less. They might take a nap or two every day. They change their routines or rely on a spouse or other caregiver to take over taxing duties.
These coping mechanisms might reduce the incidences of brain fog, but they also reduce quality of life or even keep you from living the life you want.
Things That Can Reduce or Eliminate Brain Fog
While these strategies might not completely eliminate brain fog on their own, they can all be beneficial. That said, if your brain fog comes from post-concussion syndrome, you will make the most progress by getting treatment.
Exercise
An exercise prescription might alarm you if every time you exercise, you’re immediately hit with a horrible case of brain fog. (For some concussion patients, there’s a slight delay.) However, the pros outweigh the cons in this case.
Exercise is actually crucial for concussion and post-concussion syndrome recovery. The brain needs that supply of oxygen-rich blood reaching it to spark the production of essential chemicals that lead to healing.
Two things are key if exercise triggers your brain fog:
- When you exercise, make sure that you are breathing properly. You might need to seek some outside help with this if it’s a problem for you. Self-help tutorials on the internet might be helpful.
- It’s important to exercise regularly at a sub-symptom level. This means you should exercise, but back off when your symptoms start increasing. Gradually increase the intensity of your exercise as you are able.
We’ve written a detailed post on the topic of safely exercising after a concussion, which provides additional information.
Nutrition
You don’t need to be told that good nutrition is necessary for good health. However, if going to the grocery store is a symptom-producing hell for you, you might avoid grocery shopping. Maybe you’re too exhausted to shop and cook.
In this case, you need to look for alternatives until your condition improves. Try grocery shopping at off-peak hours so you can get in and out of the store quickly and with less stimulation. Is there someone who can do the shopping and cooking for you? Would a food delivery service help? Maybe cooking in bulk and freezing individual meals could help you through the rougher days.
For ideas on what to include in your regular diet, see our brain food guide.
Relaxation Techniques
Reducing stress levels and taking time to try to force your mind to relax is another strategy. Be mindful of your thoughts. Be aware of your breathing. Take some time to relax and meditate every day.
Patients at our clinic take a short break from therapy to listen to brainwaves in a quiet room daily. We encourage them to continue this routine at home.
Is Your Brain Fog From Post-Concussion Syndrome?
 A patient tries Dynavision, a board with concentric rings of buttons that light up depending on the therapy routine.
A patient tries Dynavision, a board with concentric rings of buttons that light up depending on the therapy routine.
If you’re still experiencing brain fog months after a concussion, this is a sign that some area of your brain is malfunctioning. The longer it continues, the more a vicious cycle of negative consequences is ingrained.
Frequently, patients who come to us for post-concussion treatment have been to many health care providers and clinicians, but they haven’t gotten the results they’d hoped for. Or they weren’t taken seriously at all.
Patients often tell us about doctors who ordered an MRI or CT scan to check for more serious brain damage and found nothing. Since they didn’t have a severe traumatic brain injury (TBI), patients were told they were fine.
But the reality is that those tests typically won’t show concussion damage. Just because they didn’t show anything doesn’t mean your symptoms aren’t real.
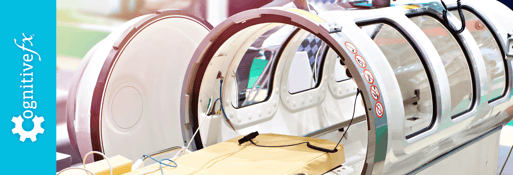
At Cognitive FX, we provide thorough assessments and treat our patients holistically through our EPIC Treatment program. We look at the results of each patient’s functional Neurocognitive Imaging scan (fNCI) — a test that can show concussion dysfunction — to design a treatment plan for that individual’s specific areas of injury. We use multidisciplinary cognitive and physical therapies to treat the core causes of symptoms, and we give patients the tools to continue their concussion recovery at home.
Our patients — which range from children to older adults — show an average of 75% improvement in brain function as measured by their before and after fNCI scans. They also self-report an average 60% improvement in post-concussion symptoms.
To learn more about diagnosis and treatment options, schedule a consultation.