Anxiety. Depression. Irritability. Dramatic mood swings. Difficulty sleeping and concentrating.
You can suffer from any of these conditions without ever having had a head injury.
However, these are some of the many common symptoms of a concussion. They are also symptoms of post-traumatic stress disorder (PTSD). People suffering from these symptoms sometimes wonder if they could be related. The conditional answer: It’s definitely possible.
Anything that jars your head or causes it to whip around suddenly can cause a concussion. This can happen in a car accident, if someone slams into you while playing a sport, or from the blast wave of an explosion in a war zone. (Note: Motor vehicle accidents and combat injuries are also very common sources of PTSD.)
You can get a concussion even if you don’t lose consciousness or experience memory loss. And you can get a concussion even if you’re wearing a helmet, since the helmet is only designed to protect the skull and not the brain from severe traumatic injury. It can’t stop the brain from sloshing around inside the skull — and that’s what causes concussions.
Most people recover from a mild traumatic brain injury (mTBI) naturally, within a few weeks. For others, however, symptoms linger and sometimes even worsen, for months or years. This condition is called post-concussion syndrome (PCS).
Many of our patients are surprised to find out that:
- You can have both post-concussion syndrome and PTSD
- You can get PTSD from the same incident that caused your concussion.
So it’s possible that either PTSD or PCS is causing your symptoms, or it could be a combination of both. Knowing which is contributing to your condition is critical to receiving the right treatment. It takes an assessment from an experienced health care provider to determine which is affecting you, but you can still learn about:
- Causes and risk factors associated with post-traumatic stress disorder
- Common symptoms of post-traumatic stress disorder and post-concussion syndrome
- Treatment options for post-concussion syndrome and PTSD
If you’re experiencing emotional and physical symptoms that won’t resolve after a concussion, you’re not alone. 95% of our patients experience statistically verified restoration of brain function after treatment. To see if you are eligible for treatment, sign up for a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
Post-Traumatic Stress Disorder: Causes and Risk Factors
Post-traumatic stress disorder is defined by the American Psychiatric Association as “a psychiatric disorder than can occur in people who have experienced or witnessed a traumatic event such as a natural disaster, a serious accident, a terrorist act, war/combat, rape or other violent personal assualt.”
The crucial component of this diagnosis is that you have to have experienced or been exposed in some way to an event that is either life threatening or psychologically traumatic. This can be from a one-time event, such as a motor vehicle accident (MVA) or an assault. It could also result from a chronic situation, such as experiencing or witnessing recurring abuse.
Note: Keep in mind that the severity of trauma is relative. Some patients become frustrated or believe that they are somehow weak because the trauma that triggered their PTSD wasn’t as bad as some others have experienced. There is no right or wrong amount of trauma to cause PTSD. You are not weak or lacking in any way because you suffer from PTSD.
Many people develop PTSD without having a related concussion. However, an injury that causes a concussion can also cause PTSD.
For example, many of the patients we see at Cognitive FX who have both PCS and PTSD received their concussion in an MVA or a bicycle accident. These accidents were traumatic in that they were sudden, unexpected, and threatening, and the patients realized later that they could have died from the accident.
Understanding How Our Bodies Respond to Perceived Threats
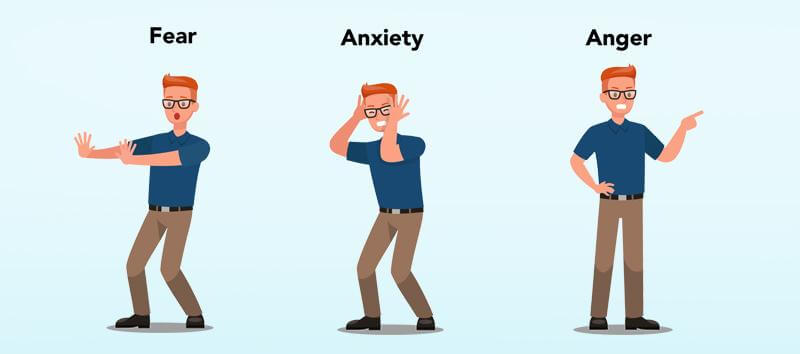
Our bodies have what you might call a threat response system. This system has three prongs: fear, anxiety, and anger. The fear system and anxiety system can both come into play with PTSD.
The fear system responds to perceived immediate threats with the “flight” half of “fight or flight.” If your fear system is engaged, you’re likely laser focused on the threat in front of you and may experience an adrenaline rush, increased heart rate, clammy hands, the urge to run, and so forth.
The anxiety system is designed to handle possible future challenges. If it’s engaged, you may ruminate on what could go wrong in the future, feel general muscle tightness in your jaw or neck, and feel moderate stomach upset.
In patients with both post-concussion and PTSD, both the fear and anxiety systems get overactivated. It becomes far easier to move into the fear state, resulting in many of the PTSD symptoms we’ll discuss later in this post.
PTSD Risk Factors: Who Is More Likely to Suffer?
Not everyone who experiences a traumatic event develops PTSD, but there are a few factors that increase the risk of developing it.
The biggest factor is the severity of the event. The more severe or life-threatening the event, the higher the chances of developing PTSD. The PTSD Alliance reports that events with increased risk of developing post-traumatic stress disorder are physical assault, active-duty combat, rape or sexual abuse, and “extreme life events” such as car accidents and house fires.
Another factor that affects the risk of developing PTSD is having previously experienced any other type of trauma. Some studies indicate that merely experiencing trauma in the past results in an increased risk of PTSD. Another study found an increased risk of recurrent PTSD if the patient had developed PTSD in response to a past trauma.
Women are more likely to develop PTSD. Having pre-existing mental health conditions or a lack of social support are additional risk factors.
PTSD and Post-Concussion Syndrome Symptoms

PTSD and PCS can cause a variety of similar symptoms; however, there are certain symptoms that point more definitively to either PTSD or PCS as the source. But before we dive in, there’s one more system we need to introduce: the autonomic nervous system.
Among other things, the autonomic nervous system (ANS) controls the sympathetic system (aka the “fight or flight” response) and the parasympathetic system (aka the “rest and relax” response). The sympathetic branch of the ANS activates in response to danger.
When the mind or body perceives a threat, the sympathetic system (aka the “fight or flight” system) kicks into high gear. It calls for a big shot of adrenaline. The heart starts pounding and blood pressure rises, giving the body a temporary boost in strength and energy to fight or flee danger. After the danger has passed, the parasympathetic system restores heart rate, blood pressure, and breathing to normal.
But after trauma, the autonomic nervous system can become dysregulated. It can contribute to many systemic issues (like blood pressure and heart rate changes, difficulty exercising, dizziness, headaches, and even gastrointestinal upset). In some patients, the ANS misperceives harmless things as a threat and activates more easily or for longer than normal, contributing to symptoms like panic attacks or difficulty sleeping.
With that in mind, let’s explore those symptoms of PTSD and PCS.
Anxiety
By definition, anxiety is being nervous or fearful of something that might happen. Physical symptoms of anxiety include restlessness; the inability to relax; muscle tension, especially in the neck, shoulders, and jaw; tightness in the abdomen; and difficulty sleeping.
Dealing with life after a concussion can cause generalized anxiety. Patients with post-concussion syndrome often suffer from debilitating symptoms day after day. They may have to drastically alter their work and social lives because of those concussion symptoms. Unknowns about how long this condition will last also contribute to anxiety and worry.
Any experience traumatic enough to cause PTSD is traumatic enough to trigger anxiety. Some patients suffer from both. But even people with PTSD who don’t exhibit signs of classic anxiety often feel like they are always on alert for danger, despite there being none. With PTSD, the overactive anxiety system is also easily activated and slow to turn off.
Someone with PTSD from a traumatic head injury could also have a dysfunctional autonomic nervous system, which just exacerbates anxiousness.
Panic Attacks
People with PTSD also frequently suffer from panic attacks, which can happen seemingly out of nowhere or after a period of intense anxiety.
Panic attacks occur when your fear system is dysregulated. Essentially, you experience a strong, physical fear response, even when there’s nothing to fear. Panic is a common symptom of PTSD, which often occurs in response to even subtle trauma reminders or triggers. Post-concussion patients can also experience panic attacks for different reasons but not in direct response to trauma reminders.
Flashbacks and Exaggerated Startle Response
PTSD patients often will experience flashbacks (typically triggered by something that reminds them of the traumatic event) in which the body and mind respond as if they were back in the threatening situation. To the patient, it feels like re-experiencing the trauma.
The trigger for flashbacks can be obvious (like fireworks for a service member injured in combat) or more subtle (like the smell of food that was cooking in the other room when the traumatic event occurred).
Flashbacks are characteristics of PTSD but not often of PCS.
However, they may occur in conjunction with something called an exaggerated startle response, in which the body responds very quickly and strongly to perceived threats, usually as a result of some kind of trigger. A smell, sight, or loud, unexpected noise (like a car backfiring or a dog barking nearby) causes a full-on activation of adrenaline and increased heart rate.
In patients with PCS, this is usually a result of an ANS dysfunction. In patients with PTSD, it can be from their overactive fear system or may be combined with a flashback.
Our patients with PTSD from an MVA, for example, report that just seeing a stop sign can trigger a flashback if their accident happened at an intersection with a stop sign. If they have to drive somewhere, they are afraid and tense — constantly scanning, expecting an accident to happen at any moment. As passengers, they become the worst back-seat drivers: hitting a foot on the floorboard trying to brake the car, gripping the door handle or the seatbelt, and warning the driver of any perceived threats. When they finally get out of the car, it can take them an unusually long time to calm down.
Overwhelm

After head trauma, being in certain environments can trigger unpleasant symptoms. For example, walking down a crowded city street or being in a busy store with a lot of noise and fluorescent lights can trigger headaches, dizziness, or nausea.
Sometimes people suddenly feel almost unable to function. Even the smallest decision seems almost impossible to make. When they find themselves in such a situation, they feel like they need to leave immediately. Patients often begin, intentionally or unintentionally, to avoid the situations that produce their concussion symptoms. This can look a lot like an anxiety disorder, but is really a symptom that stems directly from post-concussion syndrome associated with overstimulation rather than a sense of threat or danger.
PTSD patients may experience overwhelm, but usually in response to trauma triggers or feeling unsafe, which is different from the type of overwhelm PCS patients experience due to overstimulation.
Avoidance
Avoidance is a common symptom in patients with PTSD, but not usually in PCS.
Sometimes, it’s a mental or emotional avoidance. They try to push the memory of the event out of their minds completely. They refuse to think or talk about it. They describe a feeling of emotional numbness, emptiness, or apathy. A typical comment is, “I feel like a robot.”
Other times, it’s a physical avoidance. They actively try to steer clear of any physical reminder of the event. For example, if they were involved in a car accident, they dread getting into a car and don’t do it unless they absolutely have to. Sometimes they don’t want to be a passenger because they feel out of control unless they are the driver. If the accident happened on a freeway, they refuse to drive on a freeway. If there’s no way to avoid a similar situation, the exaggerated response kicks in and they are afraid the entire time.
This type of avoidance is different from that of someone with PCS. The person with PTSD is trying to avoid specific places and situations because they are perceived to be dangerous or are similar to the situation in which the trauma occurred, whereas the person with PCS is trying to avoid environments that bring on intolerable symptoms of concussion.
Note: Blunt head trauma isn’t the only source of concussion-like symptoms. Some other situations — such as stroke, viral infection (even COVID-19), carbon monoxide poisoning, and more — can cause similar dysfunction in the brain. The good news is that it can be treated in a similar manner to post-concussion syndrome. To see if you are eligible for treatment, sign up for a consultation.
Depression
A few of the symptoms of depression are persistent sadness; feelings of hopelessness and helplessness; loss of interest in things that used to interest you; decreased energy; and trouble sleeping or sleeping too much. Depression can be experienced by anyone. (Read more about depression after a concussion here.)
Difficulty Sleeping

Sleep problems can be experienced by anyone, with or without PTSD or PCS. Symptoms include having a hard time going to sleep or going back to sleep after waking up; not getting enough sleep; and sleeping too much. Damage to certain areas of the brain after a mild TBI are often responsible for sleep problems after a concussion. Up to 96% of PTSD patients may experience vivid and frequent nightmares.
Fatigue
You might wake up feeling exhausted even though you think you slept well all night. You might feel tired all the time. Or, you might have a couple of energetic hours in the morning, but then you suddenly run out of energy for the rest of the day. A concussion can affect many physiological systems and result in extreme fatigue. ANS dysfunction can also cause patients with PTSD to be extremely fatigued. The body uses a lot of energy being on high alert all day long.
Mood Swings and Personality Changes
Sudden mood swings and personality changes are common with both PCS and PTSD. Irritability and sudden angry outbursts can happen after a brain injury. In PTSD, anger is a common reaction to trauma, and it can be yet another consequence of the overactivation of the fight or flight response.
Brain Fog
Brain fog and cognitive difficulties after a concussion are common. Patients who experience brain fog often say they have a difficult time processing information, as if their brain just can’t keep up anymore. They might have to read a sentence several times to understand it. This is most often due to the inefficient communication system in the brain after an injury. The brain runs out of energy, and there isn’t enough left over to complete cognitive demands.
Brain fog is less commonly associated with PTSD, but it’s frequently experienced by post-concussion patients.
Substance Abuse
Substance abuse is common to both PCS and PTSD. Sometimes people relied on alcohol or illicit drugs before a brain injury, and that continues afterwards. But it’s not uncommon for people to turn to unhealthy ways of coping or trying to find relief from the changes brought about by a brain injury or other trauma.
If you struggle with substance abuse, the Substance Abuse and Mental Health Services Administration (SAMSA) has a hotline and other resources to help.
Treatment: How to Find Help for PCS and PTSD
Our focus and expertise at Cognitive FX is treating post-concussion syndrome. Some of our patients also suffer from PTSD and may or may not have been diagnosed before visiting us. Many times, our post-concussion PTSD patients were injured in a motor vehicle accident. These patients are almost always surprised to find out that PTSD from an MVA is not only possible but that it’s actually one of the most common forms of PTSD.
So how do we move forward with treatment in these cases?
When you’re suffering from post-concussion syndrome and PTSD, it is almost always best to begin by treating the PCS. Getting relief from the physical and mental symptoms of PCS makes it easier to move forward with treatment for PTSD.
First Things First: PCS Treatment
When a person sustains a mild traumatic brain injury, they often experience inflammation and sometimes swelling. As the brain tries to cope with that inflammation and other issues caused by the head injury, it may establish workaround communication pathways to bypass injured parts of the brain.
Unfortunately, these detours aren’t as efficient as the original pathways; the brain tires quickly while using them, leading to post-concussion symptoms. When the brain continues to use these inefficient pathways even after the initial injury resolves, the symptoms persist indefinitely.
We have developed a highly effective treatment for post-concussion symptoms using the brain’s inherent ability to repair itself (neuroplasticity) to encourage the brain to return to using its efficient, pre-injury pathways.
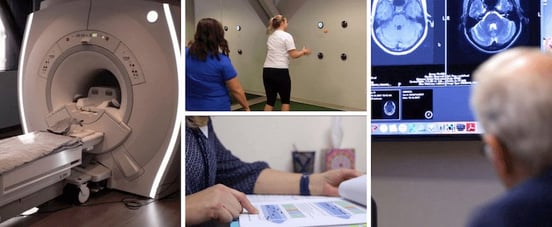
Epic Treatment begins with a functional Neurocognitive Imaging Scan (fNCI) that allows us to look at how a patient’s brain is responding to a series of cognitive demands. We measure the blood flow to specific regions, looking for areas of dysfunction. We then use the fNCI results and an inventory of the patient’s symptoms to create an individualized treatment plan that targets those dysfunctional brain regions.
Therapy includes a unique combination of neuromuscular, vision, and balance exercises, along with aerobic and cognitive activities. Relaxation and instruction in proper breathing techniques are also a part of Epic Treatment, as is a meeting with a psychologist.
Though many patients show remarkable improvement during treatment, patients are given instructions on how to continue treatment at home. This is a vital part of the recovery process.
These therapies are not designed to treat emotional disorders per se, and we make no claims to do so. However, we have found that by reducing or eliminating physical symptoms caused by a concussion, it becomes easier to deal with psychological ones. The exercises we teach you can also help the autonomic nervous system start to improve.
In addition, having more energy, getting quality sleep, and being able to think clearly make it easier to focus on successfully treating PTSD (not to mention enjoying a higher quality of life).
Getting Help for PTSD

There is no one-size-fits-all treatment for PTSD. Effective treatment needs to be tailored to the specific type of PTSD that a patient is experiencing; for example, MVA PTSD treatment protocols are not the same as treatment protocols for PTSD that stems from chronic abuse.
While patients are at Cognitive FX, we assess for PTSD and other psychological disorders, and then we provide recommendations for psychological treatment to assist them on the road to recovery.
Sometimes, the first step is talking about PTSD. As stated before, many of our patients didn’t know the injury that caused their concussion could also cause PTSD and that it’s possible to be suffering from both. For example, our MVA PTSD patients are often relieved to hear that treatment is available and the prognosis is good. Many had feared they’d never be able to drive or be comfortable in a car again.
While at Cognitive FX, we also provide strategies for PTSD symptom management, such as grounding techniques. Relaxation techniques are part of our EPIC treatment and include learning proper breathing techniques and listening to brainwaves designed to promote relaxation.
We also assist patients in finding a trauma specialist near where they live who can provide the most effective therapy for their specific form of PTSD.
Most importantly, we want you to know that there is help. You can recover from PCS and PTSD with the right treatment.
If you’re experiencing emotional and physical symptoms that won’t resolve after a concussion, you’re not alone. 95% of our patients experience statistically verified restoration of brain function after treatment. To see if you are eligible for treatment, sign up for a consultation.