Despite the fact that your concussion was weeks (or months or even years) ago, you’re still experiencing symptoms. Maybe they’re ever-present reminders of an injury you’d rather forget, or maybe they come and go as you attempt to live your life as fully as you can. Either way, you’re still suffering. What’s going on, and what can you do about it?
Recurring symptoms after a concussion are known as post-concussion syndrome (PCS) when they persist for three months or more after an injury. Some folks think these stubborn symptoms only happen after severe head injuries, but that’s not the case. Even if you experienced a mild head injury without loss of consciousness, you can still develop PCS. In fact, you’re more likely to develop post-concussion syndrome after a mild head injury than after a severe traumatic brain injury (TBI).
You might experience any number of recurring symptoms, such as headaches and migraines, brain fog, fatigue, dizziness, sleep disruption, mood swings, irritability, poor memory, depression, difficulty paying attention, and more. It’s hard enough to deal with these for a few days post-concussion, let alone indefinitely.
While post-concussion syndrome doesn’t usually resolve on its own, it can get significantly better with the right treatment regimen. Unfortunately, it can be difficult to find a treatment provider who is able to tailor treatment to your brain’s specific needs. Many providers simply don’t have the in-house resources to treat a complex condition like PCS, and one or two therapies are usually not enough on their own to produce a robust recovery.
At Cognitive FX, we specialize in post-concussion syndrome treatment. We offer a combination of cardiovascular exercise and multidisciplinary therapy to promote healing in the brain and reduce symptoms. This treatment program is effective regardless of whether it’s been months or decades since your injury. Out of the thousands of patients we’ve treated at our clinic, the average percent improvement in symptoms after just one week of treatment is 60%. And 90% of our patients experience improvements in that timeframe with a significant reduction in the incidence of symptoms.
Our patient, Anthony Loubet, is just one example. In 2019, he was involved in a serious car accident. The first few months after his mild traumatic brain injury (mTBI) were incredibly frustrating. He suffered from multiple recurring post-concussive symptoms, including short-term memory loss and other cognitive problems, extreme mood changes, light sensitivity, sleep disturbances, and digestive symptoms. Anthony visited many different doctors and therapists to address these issues, but nothing worked until he found Cognitive FX. After his treatment with us, he was able to go back to work full-time. “I came back to work, and everybody noticed that there was something different because I had been so slow to do things, to communicate,” he said. “I came back, and I was happier; I was faster.”
So how do you go from recurring symptoms that just won’t get better to living your life normally again? The journey is different for each person, but there are many resources to aid you in recovery. In this article, we’ll share:
90% of our patients report reduced symptoms after their treatment at Cognitive FX. To see if you’re a good fit for our program, sign up for a consultation.
Common Causes of Recurring Concussion Symptoms

Most people who suffer a mild TBI recover fully within a few days or weeks. They return to everyday life without any long-term effects of head injury. Some patients, however, continue to experience recurring symptoms for months or even years after their initial injury.
Risk Factors for Post-Concussion Syndrome
Doctors don’t fully understand why some patients recover after a concussion and others develop persistent post-concussive symptoms, but they recognize that there are some risk factors. Patients are more likely to develop post-concussion syndrome (PCS) if they:
- Suffered past concussions or head injuries: Each concussion is an opportunity to develop new physical and cognitive symptoms. It’s unclear whether or how a past concussion increases the risk of long-term symptoms from a future concussion, but anecdotally, many of the patients we see in the clinic have suffered more than one concussion. Suffering more than one injury is common in contact sports, where the risk of developing a sport-related concussion is high.
- Suffered a concussion with complications: Some examples include midline shift (when the brain moves off-center inside the skull), a skull fracture, or bleeding inside the skull or brain.
- Have other neurological or mental health conditions. For example, patients with attention-deficit/hyperactivity disorder (ADHD), anxiety, or depression may have a higher risk of developing PCS.
- Experience multiple concussion symptoms. Patients who experience many different concussion symptoms right after their injury — especially if they have severe symptoms — are at a higher risk of developing post-concussion syndrome.
It’s difficult to determine what causes symptoms of post-concussion syndrome in each patient, though a full evaluation can usually reveal which factors are present. The most common causes of recurring PCS symptoms usually include a combination of:
- Neurovascular coupling disruption
- Dysfunction of the autonomic nervous system
- Hormonal dysfunction
- Vision and vestibular problems
- Breathing dysregulation
Neurovascular Coupling (NVC) Disruption
In a healthy brain, brain cells “request” the resources they need to perform a particular task from surrounding blood vessels. These resources come in just the right amount at just the right time in response. This dynamic link between brain regions and the circulatory system is called neurovascular coupling (NVC). Concussions “uncouple” this connection, which means affected brain regions may be unable to complete their tasks. This could be because too many or too few resources are delivered to the brain region in question or because the timing is off (or both). Often the brain has to divert tasks to healthier brain regions, but these regions are less efficient at performing unexpected tasks and may be overloaded easily as they try to juggle what’s already expected of them plus this new burden.
Neurovascular coupling dysfunction results in a variety of symptoms, such as headaches, feeling overwhelmed, and irritability. It may feel like your brain is shorting out when you try to do too much. In addition, you’ll likely experience symptoms specific to which regions of your brain are affected. If the concussion affected areas of the brain involved with vision, for example, you might experience double or blurred vision, difficulty reading, eye fatigue, trouble with crowded spaces, dizziness, and so forth. If the concussion affected areas involved with speech, on the other hand, you might struggle to find the right words, speak more slowly than usual, or get easily confused during conversation.
Neurovascular coupling dysfunction shows up on a special type of brain scan known as functional Neurocognitive Imaging (fNCI), which we’ll describe in more depth in the section on diagnosis.
Dysfunction of Autonomic Nervous System (ANS)
Concussions also affect the autonomic nervous system (ANS). The autonomic nervous system controls vital bodily functions such as heart rate, blood pressure, and breathing rate. This is done via two subsections called the sympathetic nervous system (SNS) and the parasympathetic nervous system (PNS). The sympathetic nervous system regulates the “fight or flight” response, while the parasympathetic nervous system is responsible for the “rest and digest” process. Under normal circumstances, the parasympathetic nervous system and sympathetic nervous system work together in harmony.
For example, let’s say you’re working against a tight deadline. In this situation, the SNS might raise your heart rate and blood pressure. You might feel tension in your muscles from the stress. After you complete the work and the deadline passes, the PNS should help release muscle tension, decrease heart rate and blood pressure, and overall help you relax and regroup.
Or, during a workout, the SNS and PNS might work together closely to make small adjustments to your bodily functions as you move from exercise to exercise.
After a concussion, however, the SNS can remain activated all or most of the time, even when it’s not needed. As a result, PCS patients experience symptoms such as fatigue, headaches, high blood pressure, heart rate changes, body temperature changes, digestive issues, problems sleeping, mood changes, and more.
Further reading: Autonomic nervous system dysfunction after a TBI
Hormonal Dysfunction
In addition, concussions sometimes affect the pituitary gland and the hypothalamus. These two endocrine glands regulate many different mechanisms in the body. Hormone imbalances stemming from injury can cause a myriad of symptoms, including depression, chronic pain, fatigue, digestive issues, and sleep disturbances.
Further reading: Post-concussion hormone dysfunction
Vision and Vestibular Problems
Vision problems are very common after a concussion. Any injury that affects the eyes, the brain, or the way they communicate with each other impacts our ability to see correctly. These issues can result in complications such as dizziness, blurry vision, poor balance, and difficulty reading or concentrating.
Further reading: Vision problems after a concussion
Similarly, vestibular issues can also lead to PCS symptoms. Concussions can disrupt the connection between the vestibular system (located in the inner ear) and the brain and lead to symptoms like dizziness, poor posture, instability when walking, fatigue, and difficulty performing routine daily activities.
Further reading: How concussions can cause vertigo years later
Breathing Dysregulation
Head trauma can also disrupt the connection between the brain, the ANS, and the lungs. If the brain or ANS don’t “understand” what the lungs need, patients may suffer breathing disturbances, including shortness of breath, irregular breathing, dizziness, and fatigue. These difficulties can also perpetuate autonomic dysfunction, creating a cycle of worsening concussion symptoms.
Further reading: Can PCS cause breathing difficulties?
How Is Post-concussion Syndrome Diagnosed?
At the moment, there isn’t one, definitive test to prove that you have post-concussion syndrome. Instead, most healthcare providers diagnose patients with PCS if:
- Recurring symptoms last for more than three months after the concussion; and
- All other possible causes for the symptoms have been checked and ruled out.
What those symptoms are may not stay the same over time. For example, your initial confusion and dizziness may go away, while cognitive tasks become increasingly difficult, and you feel constantly tired. Here are some of the most common recurring concussion symptoms (and links to articles with more detailed information than we have room to cover here):
- Many post-concussion syndrome (PCS) patients experience post-traumatic headaches. Read about what causes headaches, how they manifest, and how to treat them.
- Vision problems and light sensitivity are common symptoms in PCS patients. Our articles cover how these are treated, how long it takes to recover, and treatment options for post-concussion vision changes.
- Patients can also experience balance issues, including difficulty balancing, vertigo, and other vestibular symptoms. Our article explains how concussions cause vestibular problems and how they are treated with vestibular therapy and neurointegration.
- Sleep disturbances affect many post-concussion syndrome patients and aggravate other symptoms. Our article explains how PCS can disrupt sleep, how it affects recovery, and what patients can do about it.
- Post-concussion fatigue has a high prevalence after a concussion. Our article describes how your head trauma makes you so tired and how to get your energy back.
- Many post-concussion syndrome patients experience difficulty exercising post-concussion. We explain how to exercise safely after a concussion and what to do if exercise triggers symptoms such as dizziness or headaches.
- Cognitive impairment, such as brain fog, memory loss, and other related symptoms are also common complaints from post-concussion syndrome patients. Our articles describe how concussions can cause these symptoms and what you can do to help your brain heal.
- Emotional or personality changes are also common after a concussion. Our article explains the relationship between brain injuries and these symptoms and how you can address them.
- Post-concussion syndrome can also cause cardiovascular problems, including blood pressure changes, heart rate changes, palpitations, and more. Read about how a concussion can affect your heart and how it’s treated.
- Whiplash and neck pain often occur at the same time as a concussion. Read about what causes neck pain after a head injury and how it’s treated.
- Gastrointestinal symptoms, such as loss of appetite, stomach upset, food intolerances, and acid reflux can also occur after a concussion. Read about how head trauma can cause these problems and possible treatments.
Besides asking about symptoms, medical professionals (such as neurologists and clinicians) may request a follow-up CT scan (computed tomography scan) or an MRI scan (magnetic resonance imaging scan) to detect severe structural brain abnormalities, brain bleeding, or skull fractures. These scans, however, cannot be used to diagnose post-concussion syndrome because they only detect structural changes in the brain. (PCS only causes functional changes.) Patients can have a normal scan and still experience recurring symptoms after their concussion.
Further reading: Why an MRI can’t detect concussions
That said, functional MRI scans can be used to investigate the effects of post-concussion syndrome. fMRI looks at blood flow dynamics rather than structure integrity. The specific type of fMRI we use at Cognitive FX is called a functional Neurocognitive Imaging (fNCI) scan.
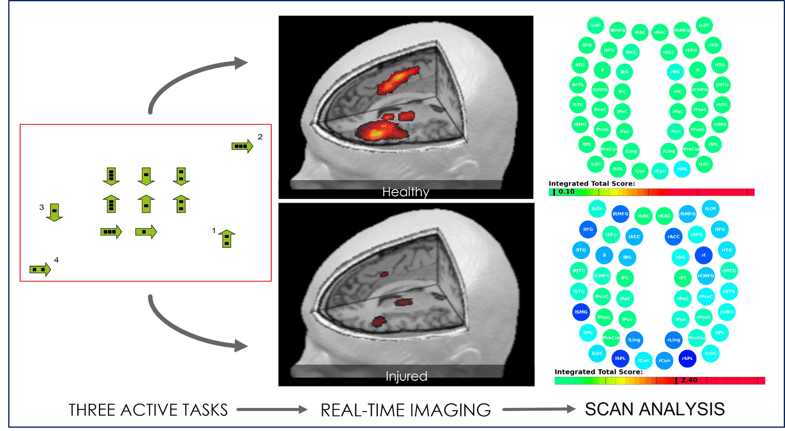
fNCI allows us to image 100 different regions of the brain, investigating blood flow dynamics and communication patterns while our patients complete a set of predetermined cognitive tasks. We use the scan to understand which regions of the brain are working normally and which ones are struggling. Crucially, with this information, we can tailor treatment to the specific needs of each patient (more on this later). The fNCI scan is a key component of our post-concussion treatment that other clinics do not offer.
The exact testing done to evaluate PCS patients is different from clinic to clinic. At Cognitive FX, we take a number of factors into consideration:
- fNCI results
- Medical history
- What symptoms the patient is experiencing
- Results of a physical exam that assesses balance, hand-eye coordination, and other physical abilities
- Results of a cognitive assessment that checks memory, focus, thinking, and other cognitive skills
- Results of a psychological evaluation intended to spot symptoms of mental health problems, such as anxiety and depression
Is Post-concussion Syndrome Recovery Possible?
 A therapist at Cognitive FX demonstrates an activity from occupational therapy.
A therapist at Cognitive FX demonstrates an activity from occupational therapy.
The brain has an innate ability to recover from injuries like concussions. This process is called neuroplasticity, and it refers to the brain's ability to change, reorganize, or even grow new neural networks in response to stimuli.
Immediately after a concussion, neurons in the affected areas stop functioning properly, and the brain can no longer use neural pathways involving these brain cells. To deal with this, the brain looks for alternative pathways to achieve the same task. The problem is that these alternative pathways are not as efficient as the original pathway, causing symptoms of concussion like fatigue, headaches, and brain fog.
In the weeks and months after the injury, brain plasticity involves the formation of new neural pathways and new connections between brain cells. The brain also recruits various types of cells to take the place of those damaged or killed in the injury.
If you leave your brain to recover naturally — without any form of treatment — this process will still happen, but it is entirely possible that the new neural pathways will not be the most effective ones, and that they will even aggravate your recurring symptoms.
In contrast, with appropriate interventions and rehabilitation, it’s possible to guide neuroplasticity in the right direction during the healing process. The aim is to promote new neural pathways that reduce or eliminate the symptoms caused by a concussion. For example, cognitive rehabilitation can help patients recover memory and other thinking skills, and vision therapy can help patients recover their vision because these treatments restore the neural connections and retrain the muscles involved in these processes. This is the approach we use at Cognitive FX.
On average, our patients’ symptoms improve by 60% after just one week of treatment at our center specializing in the long-term symptoms of head injury. To see if you are eligible for treatment, sign up for a consultation.
How Is Post-concussion Syndrome Treated?

Treating patients with post-concussion syndrome is challenging. At the moment, there is no medicine clinically proven to treat PCS. Instead, many doctors prescribe meds for specific symptoms, such as painkillers for headaches and migraines, sleeping pills for sleep disturbances, and antidepressants for emotional problems. The problem is that — as long as the underlying problem causing PCS is not addressed — these symptoms won’t go away. Patients can experience slight improvements for a while, but symptoms eventually come back; plus, the side effects of the medication can be just as bad as the original symptoms.
Further reading: Medication for post-concussion syndrome
At Cognitive FX, we offer physical exercise and multidisciplinary therapies to address the roots of problems such as neurovascular coupling disruption, autonomic dysfunction, vision changes, and vestibular issues. While most patients do not recover 100% by the end of our treatment — called Enhanced Performance in Cognition (EPIC) — they experience significant improvements in many symptoms and continue to improve at home. Most patients are with us for one to two weeks of intense therapy.
Before treatment starts, patients undergo extensive medical neuropsychological tests and complete their fNCI brain imaging scan (as described earlier). Once our doctors and therapists have gathered all the necessary information, they can design a treatment plan customized for each patient.
Our treatment involves a three-step cycle that is repeated throughout your time at the clinic: Prepare, Activate, and Recover.

The prepare step starts with physical therapy, which involves short intervals of intense cardiovascular exercise, usually on a stationary bike or treadmill. The aim is to improve blood flow within the brain and to promote the release of a compound called brain-derived neurotrophic factor (BDNF). BDNF boosts the impact of subsequent therapies and helps the brain adapt better to changes.
After exercise, patients engage in a series of therapies to activate the brain and treat PCS symptoms. Therapies include:
The overall list of therapies offered to each patient may be similar, but the specific exercises and how they’re combined can vary considerably from patient to patient because of how closely they are tailored to each person’s injury and evaluation results. That’s why our treatment success outcomes are so consistent and reliable.

Take Myrthe van Boon’s story, for example. Myrthe traveled all the way from Holland to receive treatment at Cognitive FX after hitting her head in a skiing accident. For 13 years, Myrthe suffered relentless recurring symptoms, including headaches, light sensitivity, extreme fatigue, poor memory, and dizzy spells. During her stay with us, Myrthe worked very hard on memory exercises, balancing exercises, visual exercises, occupational therapy, speech therapy, and everything in between. After just two days she noticed improvements. "Halfway through the week, I went outside during my lunch break, and the world looked totally different — brighter and clearer. My head was calm for the first time ever in all those years. It was an amazing and emotional moment. It gave me faith that this was going to work and would make a difference."
Now, Myrthe can exercise regularly without any symptoms, doesn’t have regular headaches anymore, and no longer needs medication for dizziness. “I think the improvement is more than 80%. I could never have dreamed that I could have had this life again. For me, it's worth everything. Every day, I’m so grateful that we did this.”
 Myrthe van Boon celebrates a great week of treatment.
Myrthe van Boon celebrates a great week of treatment.
Finally, throughout the day, patients also enjoy periods of rest and recovery before the next set of therapies. These periods include breathing exercises and listening to brainwaves to promote relaxation, neuromuscular massage of the neck and shoulders, and mindfulness exercises.
At the end of treatment, patients go through a second scan to assess how their brain is healing and meet with one of our therapists to discuss their results. Patients also receive a set of exercises to do at home, which include aerobic exercises, cognitive activities, and relaxation techniques. Most patients need to spend about an hour per day, five days a week on these exercises and then slowly reduce the time spent as they recover. Completing these exercises boosts your chances of a fast and complete recovery.
90% of our patients report reduced symptoms after their treatment at Cognitive FX. To see if you’re a good fit for our program, sign up for a consultation.
What Can You Do at Home to Promote Your Recovery?

What you do at home has a massive impact on your recovery. Here are a few tips to help you speed up your recovery from post-concussion syndrome:
Take Frequent Brain Breaks
Frequent brain breaks during the day don’t mean staying alone in a dark room doing nothing. Instead, it involves having periods during your day where you limit physical and neural stimulation as much as possible. This could be moving away from the computer and going for a short walk, listening to quiet music, or simply sitting in silence for a few minutes.
Further reading: Breaks are good for the brain
Track Your Symptoms
Tracking your symptoms can help you and your doctor to monitor your recovery. Without this information, it’s difficult to identify triggers that make your symptoms worse or to understand what’s helping you get better. A daily log is a good way to keep tabs on your symptoms. Consider logging items such as:
- Sleep quality
- Symptoms
- Screen time
- Completion of therapy exercises
- Exercise
- Cognitive activities
- Social outings
Engage in Regular Exercise
Physical activity is key for recovery. Increasing your heart rate promotes healthy blood flow within the brain, which in turn speeds up brain healing. Exercise also improves mood, reduces feelings of anxiety and depression, and improves sleep.
Tips to exercise safely:
- Engage in some exercise every day. Even if it’s only for a few minutes, it’s always worth doing. A stationary bike or treadmill is ideal for getting your blood pumping without making your symptoms worse.
- Gradually increase the duration and intensity of exercise. The best way to do this without triggering too many symptoms is by increasing your heart rate a little more every session. At Cognitive FX, we will teach you how to alternate between intense exercise intervals and controlled breathing so that you can reap the benefits of exercise while mitigating symptoms as much as possible.
- Avoid activities where there’s a risk that you may hit your head again. A second concussion could seriously delay your recovery.
Further reading: Why exercise is important for post-concussion healing
Challenge Your Brain
After exercise, engage in some cognitive games and activities. Try playing a game with a friend, or have an interesting conversation with someone. Or, choose one of these cognitively stimulating activities you can do at home. Take breaks as needed, but aim to engage your brain for about thirty minutes total every day.
Follow a Healthy Sleep Pattern
Much of the recovery your brain needs happens while you’re sleeping. This is because sleep promotes the release of important hormones and allows nerve cells to repair themselves.
To increase your chances of a good night’s sleep:
- Go to sleep and get up at the same time every day, including weekends and holidays
- Avoid screens (smartphones, TV, and computers) before bedtime
- Limit daytime naps to 20-30 minutes, ideally early in the afternoon
- Engage in regular exercise (see above)
- If you’re experiencing tinnitus, a white noise machine can help you create a distraction and soothe you into a deeper sleep
- Try a weighted blanket
- Try melatonin supplements
Follow a Balanced Diet
Following a healthy and balanced diet can help you recover faster from PCS. Here are a few tips:
- Drink plenty of water during the day to avoid dehydration. If possible, avoid soda and energy drinks.
- Be careful with caffeinated drinks. Drinking too much coffee or other caffeinated drinks can overstimulate your brain and lower your tolerance to your daily activities.
- Don’t skip meals. Some patients find six small meals over the course of the day to be more helpful than three larger meals, as they provide more stable autonomic function.
- Eat plenty of fruits and vegetables. Avoid processed foods and refined sugar.
Further reading: Post-concussion nutrition to support healthy brain function
Avoid Further Head Injuries
Getting a second concussion while you’re still recovering from PCS can be dangerous. More than one concussion can result in further brain damage that results in long-term complications and permanent impairments, even potentially leading to chronic traumatic encephalopathy (CTE). Multiple concussions also increase the risk of depression, anger, memory loss, post-traumatic stress disorder (PTSD), and other conditions that may not resolve without the help of a psychiatry or psychology practitioner.
Be Patient
Recovery isn’t linear. All patients, even those who recover faster than usual, have good days and bad days. This up-and-down recovery pattern is normal. Most patients do recover; for the majority of our patients, treatment at Cognitive FX plus doing the at-home exercises is enough. Some need additional support from specialists; for example, those with long-standing vision dysfunction often need extra therapy from specialists such as neuro-optometrists.
Some of the patients we’ve treated experienced their concussion(s) decades ago. All of our data shows that they recover just as well as everyone else. The brain never loses the ability to adapt to changes, especially if given the right stimulus.
How you persevere and the attitude you bring to recovery matters. The more you choose to set a positive tone and believe in your ability to recover, the more likely you are to reach your goals.
Ready to take the next step on your recovery journey? To see if you are eligible for treatment, sign up for a consultation.

















