12 Recovery Tips for Patients with Post-Concussion Syndrome
Recovering from post-concussion syndrome (PCS) is challenging, but with the right guidance, substantial progress and symptom relief are possible, even years after the initial injury.
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY
At our post-concussion treatment clinic, patients sometimes present with short- or long-term hormone dysfunction after brain injury. While we don’t treat hormonal imbalance at our clinic, we often make referrals for it and communicate with our patients’ physicians about their condition.
Hormone dysfunction doesn’t always become apparent overnight. The symptoms sneak up on you. You start having less and less energy, you get dramatic mood swings, you notice your hair gradually thinning, or your workouts become impossible even though they used to be fine. And since some of the symptoms are easy to blame on other parts of your life (such as stress and diet), it can be a while before you or your doctor suspect hormones.
But if you have symptoms of hormone dysfunction, it’s so important to find a good doctor to treat your condition. Some hormone insufficiencies (such as cortisol) are life threatening; others won’t kill you, but they greatly reduce your quality of life. Unfortunately, getting the right diagnosis and treatment isn’t an easy journey for most patients. Hormone imbalance is not something every family doctor can or will treat. You may have to visit several doctors before finding someone who meets your needs.
We’d like to make that journey as painless as possible, so we made this series of checklists and graphics (along with a full infographic) to help you talk to your doctor about hormone problems. We include:
Click here to view + download the full infographic.
Do you have persistent symptoms after a mild head injury? You’re not alone, and you’re not crazy. On average, our patients improve by 75% after treatment at our center specializing in post-concussion therapy. To see if you are eligible for treatment, sign up for a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
Finding a good doctor for hormone imbalance is hard. Many doctors do not have experience testing for or treating hormone imbalance, and many who do can be inflexible in their opinions and treatment regimens.
It is common for patients to try a few doctors before finding the right one. Don’t give up hope! If a doctor is dismissive of your symptoms or unwilling to look beyond the most basic tests, try a different doctor (even within the same practice). You deserve to be treated by a physician who will take you seriously and dig deeper when the solution to your health issues isn’t apparent at first glance.

Crowdsourcing is the way to go when it’s time to find a good doctor. Read reviews and, if you can, find people who struggled with similar symptoms. If their doctor helped them, it’s worth an initial visit to see if they can help you, too.

Let’s explore these items — they’re important.
Symptoms: Take notes when you’re experiencing symptoms instead of making the list in hindsight. If you wait until later, you might forget important details. For example, you might jot down that you drank four liters of water — but still felt thirsty. Or you might note that you had a severe headache in the afternoon after one morning cup of coffee and two bottles of water.
Don’t be embarrassed by your symptoms; it’s not like you chose them! Your doctor needs to know about any changes that could be related to hormone balance, including sexual dysfunction, changes in hair growth, body odor, and more.
Be firm about what’s normal and not normal for you. For example, with gonadotropin deficiency, patients might notice muscle mass loss. And the knee-jerk reaction of an MD is to say, “Oh, you just need to exercise more.” Well, yes, most of us do. But is it normal for you to struggle to carry the laundry? That added context is a good way to address skepticism
Note for females who have irregular periods or menstrual cycle changes, severe PMS, polycystic ovary syndrome (PCOS), endometriosis, infertility, low libido, or other issues that could stem from hormone imbalance: Consider learning a fertility awareness-based method (FABM). Some ObGyns are trained to diagnose and treat hormone issues without birth control by using the information from your monthly charting. Some methods can provide insight into thyroid health by tracking your morning temperature. You can learn more here and here.
Medications and supplements: Bring a complete list of the medications and supplements you’re taking. If you haven’t already, start taking a multivitamin and consider vitamin D supplements. Some doctors will ask you to take them before running tests, so it helps to get that done ahead of time.
Be honest if you’re not taking prescribed meds as directed. Your doctor needs that information to devise an appropriate treatment plan.
Bringing an advocate: Doctors are imperfect human beings, just like the rest of us. They can be prideful, dismissive, skeptical, or rushed. Bring someone who can advocate for you when you’re uncertain or struggling to speak up for yourself. This is especially important if you have symptoms like anxiety or difficulty finding words in the moment.
Handling weight gain: Some healthcare providers will immediately blame all your symptoms on weight gain. Rapid, unexplained weight gain or loss often stems from underlying health issues and is something you should talk about. But if you’ve gained a few pounds for understandable reasons (like, say, spending months inside during a pandemic), ask that your doctor evaluate symptoms without considering your weight. You can always address dietary concerns separately with a nutritionist.
Note: It’s common for women to experience weight gain around menopause along with other symptoms like hot flashes.
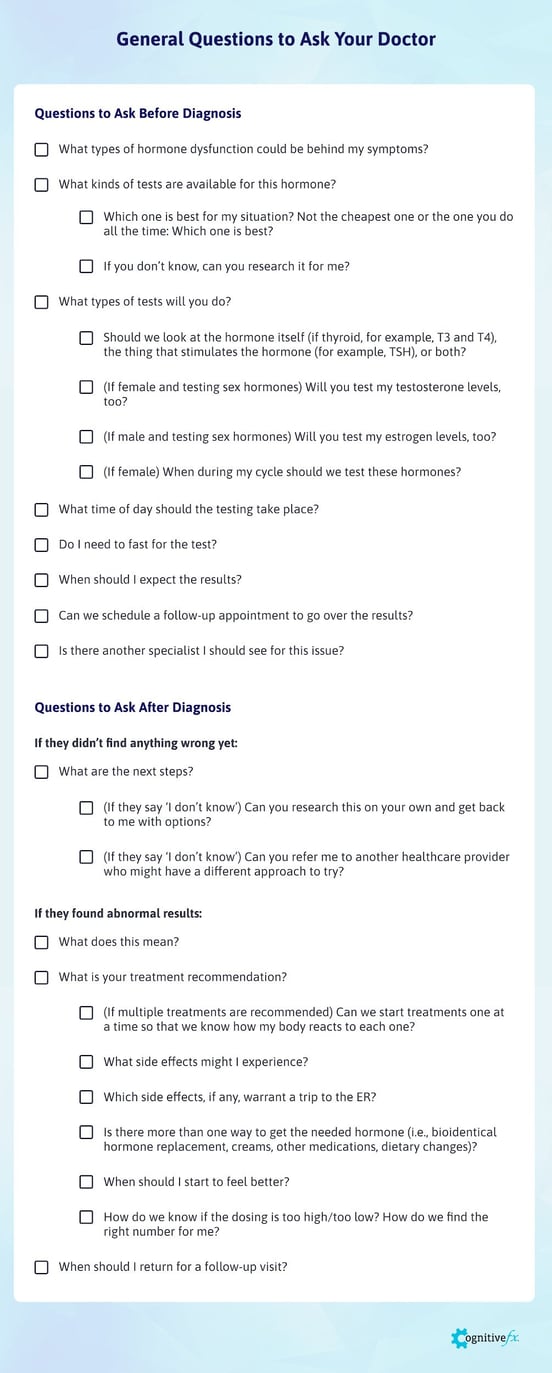
Use these questions as a starting point for your visits. If you think of other questions to ask before or during your visit, ask those too!
When you discuss testing, don’t be afraid to ask about alternatives. Blood tests are not always the only option; some hormones have good urine or saliva tests available as well.
If your physician wants to prescribe multiple medications, ask if you can start with the most important one first and work your way down the list. This process makes it easier for you to identify side effects and dosing problems early, if you experience them.
For example, let’s say your doctor decides to use bioidentical hormone replacement therapy for a progesterone deficiency and also thyroid medication. You might start with the thyroid medication first, then take the progesterone a month later after ensuring that your body handled the thyroid medicine well.
Finally, if you’re working with more than one doctor, remember that it’s completely acceptable to ask one of your doctors to talk to another one of your doctors. If they coordinate your care with each other, that’s ideal.
Up to 46% of patients experience neuroendocrine dysfunction after mild traumatic brain injury. If you or someone you love is suffering from inadequate hormone levels after a brain injury, you’re not alone.
Any one of these scenarios could result in hormone dysregulation:
The most common form of disruption following brain injury is hypopituitarism, resulting in lower-than-needed hormone levels throughout the body. The pituitary gland fails to produce signaling hormones that regulate hormone production elsewhere. For example, thyroid hormones (T3 and T4) may be low if your pituitary doesn’t produce enough thyroid-stimulating hormone (TSH). While most cases of hypopituitarism subside nine months after injury, some hormone troubles persist indefinitely after the injury.
The most common deficiencies after a brain injury are growth hormone deficiency, adrenal insufficiency, hypothyroidism, hypogonadism, and sex hormone deficiencies (commonly lower estrogen, progesterone, and testosterone), and antidiuretic hormone (ADH) insufficiency. Some patients also suffer from underproduction or overproduction of prolactin (hypo- or hyperprolactinemia).
While there are many other types of hormone dysfunction, these are the ones we see most in the patients we treat. Here is a chart of symptoms arranged by type of hormone dysfunction:

As we mentioned before, we can’t treat hormone dysfunction in our patients. But we can address symptoms that stem from brain dysfunction after injury (and occasionally, this helps hormone regulation as well). To learn more about what happens to the brain after a mild traumatic brain injury, why some people have symptoms that linger for years, and what can be done about it, read our guide to post-concussion syndrome.
Diagnosing and treating hormone dysfunction isn’t easy, even when your doctor is knowledgeable and attentive. Doctors are human beings. They are busy. They make mistakes. Push them to give you the best care possible. Be persistent and advocate for your needs (or bring a friend to do it for you). You can improve with the right care.
Do you have persistent symptoms after a mild head injury? You’re not alone, and you’re not crazy. On average, our patients improve by 75% after treatment at our center specializing in post-concussion therapy. To see if you are eligible for treatment, sign up for a consultation.

Alina Fong, Ph.D. is a clinical neuropsychologist and the Clinical Director and Co-Founder of Cognitive FX. She earned her Ph.D. in Clinical Neuropsychology with an emphasis in Neuroimaging from Brigham Young University, where she received the American Psychological Association Division 40 Graduate Student Research Award for her neuroimaging research. Dr. Fong has over 17 years of clinical experience treating traumatic brain injury, beginning with her work at the VA Salt Lake City Healthcare System and Utah Valley Regional Medical Center, where she directed the neurotrauma rehabilitation and sports concussion clinics. She developed the EPIC Treatment protocol and has personally overseen treatment for nearly 8,000 brain injury patients, including professional athletes from the NFL, NHL, and Olympics. She serves as Vice President of the Brain Injury Alliance of Utah, sits on the board of the United States Brain Injury Alliance, and advises PINK Concussions. Dr. Fong has authored peer-reviewed research on functional MRI and concussion treatment and has presented at over 60 medical conferences, including the Federal Interagency Conference on TBI and the American Medical Society for Sports Medicine.

Recovering from post-concussion syndrome (PCS) is challenging, but with the right guidance, substantial progress and symptom relief are possible, even years after the initial injury.

The type of head injury doctor you need to see depends on the type of injury you’ve experienced and how long ago the injury occurred. Doctors who excel at concussion treatment, for example, are often...

Neural fatigue can develop after any type of brain injury, including mild traumatic brain injury (concussion), severe traumatic brain injury (TBI), hypoxia,viral infection, stroke, ortransient...

Many doctors aren’t aware that concussions can cause long-lasting symptoms, a condition commonly called post-concussion syndrome (PCS). As a result, they treat common symptoms rather than the...

Many people are surprised to learn that concussions can have long-term effects if left untreated. Chronic concussion syndrome is a less common term for persistent post-concussion symptoms (also known...

Most patients recover from a concussion within days or weeks. But for roughly 30%, symptoms such as post-traumatic headaches, dizziness, fatigue, sleep disturbance, and brain fog persist for months...
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY