Here’s something you probably won’t hear in the emergency room: A transient ischemic attack (TIA, or mini-stroke) can have symptoms that last for months or years afterward.
Many healthcare providers think these symptoms are rare or at least short term, but a 2013 survey from the UK Stroke Association showed otherwise. Seventy percent of respondents reported long-term after effects such as cognitive difficulties or poor mobility. And sixty percent had emotional changes after the incident.
As frustrating as it may be, it’s easy to understand why these patients are overlooked. Busy medical professionals allocate their time to the most pressing needs; when stroke victims emerge alive, it’s a victory. But many need intense physical and cognitive therapy to relearn basic functions like walking, talking, and self-care. Not all of them can do those things again. In comparison, most TIA survivors can walk, talk, and feed themselves; because of this, they get lost in the shuffle.
But persistent symptoms like memory problems, foggy thinking, emotional changes, and difficulty expressing yourself shouldn’t go untreated. They have a significant impact on your quality of life. You deserve to know that these symptoms can come from a TIA, and you deserve to get appropriate counsel and medical care.
In our clinic, we treat lingering physical and cognitive symptoms from brain injuries such as concussion, bacterial and viral infection, carbon monoxide poisoning, “chemo brain,” transient ischemic attack, and more.
The TIA patients who came to us had no idea that TIA could cause lingering symptoms when they were first treated at their local hospital. They were so relieved to know there was help available to them.
We believe every TIA patient should know about the after effects of TIA and how to get help when needed. In this post, we review some basic information about how TIAs happen and how to recognize if you’re having one, but we’ll primarily focus on two topics:
Most importantly, seek medical care immediately for a TIA and follow your doctor's stroke prevention steps. Your doctor may order blood tests to check for underlying conditions like high cholesterol or clotting disorders that increase stroke risk. Afterward, pursue medical advice and care to address any longer-lasting effects of the TIA.
If you’ve been suffering from lingering symptoms after a TIA, you’re not alone and you’re not imagining it. TIA can and does cause persistent symptoms that won’t resolve without treatment. 95% of our patients experience statistically verified restoration of brain function after treatment at our clinic. Book a consultation with our team to learn if we can help you.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
What Is a Transient Ischemic Attack?
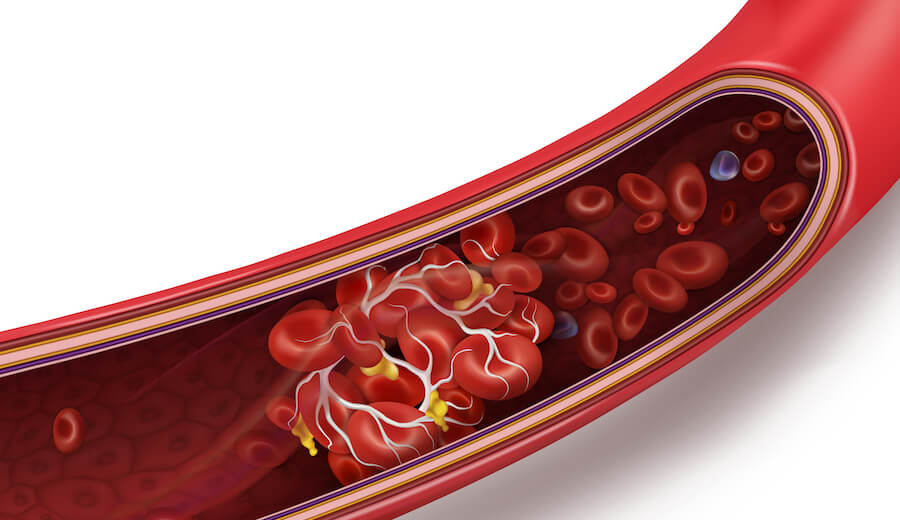
A transient ischemic attack (TIA) is a temporary vascular blockage, usually from fatty deposits (plaque buildup), that reduces or halts blood flow to part of the brain. 'Transient' indicates its duration, typically less than one hour but occasionally longer. An ischemic stroke is caused by clotting rather than blood vessel rupture, ending when the clot dissolves and blood flow resumes.
TIA does not cause widespread, permanent damage, but it may result in small pockets of dead brain cells. It is often called a “warning stroke” because it precedes about 15% of all strokes, and 9-17% of TIA patients have a stroke within 90 days. That means it’s extremely important to seek medical attention and follow-up care because of your higher risk of a stroke.
Symptoms of a TIA
In the moment, you may not know whether you’re having a mini-stroke or a full stroke because many of the signs are the same. You can remember the warning signs and symptoms of stroke with the BE FAST acronym:
- Balance problems: Are you dizzy? Have you fallen?
- Eyesight issues: Have you lost your eyesight? Is your vision blurry?
- Facial weakness: Can you smile? Are your ears or eyes drooping?
- Arm weakness: Can you raise both arms normally? Do you have any muscle numbness or tingling?
- Speech problems: Can you speak clearly? Can others understand you? Can you understand them?
- Time to seek immediate medical attention if any of these signs are present. Every minute matters.
Symptoms of a TIA appear suddenly and may disappear just as quickly. People often mistake them for a migraine or a pinched nerve. Other stroke symptoms include numbness or tingling on one side of the body, memory loss, and confusion.
Take these signs seriously. It’s better to go to the ER or a local hospital’s stroke clinic for a false alarm than to have an undiagnosed TIA or full stroke. Work with your doctor to identify your stroke risk factors (such as high blood pressure/hypertension, high cholesterol, atrial fibrillation, or family history of heart disease or heart attack), take any needed preventative medications (such as statins, anticoagulants, or antiplatelet agents like clopidogrel), and make recommended lifestyle changes to decrease your risk of future stroke (such as diet and exercise).
After your acute care and recovery, you may notice any number of these long-term effects of TIA:
While these symptoms may resolve with time, if they’re still present three months after your TIA, they probably won’t go away on their own. You’ll need appropriate therapy to help them resolve.
What Causes the After Effects of TIA?
During a transient ischemic attack, a blood clot restricts or prevents blood from reaching certain subsections of the brain. These parts of the brain may go without needed resources such as sugar and oxygen for minutes to hours. After the TIA resolves, the brain doesn’t fully return to normal. Functional MRI (fMRI) studies show that even the resting state MRI of TIA patients is abnormal. (This means that their brains don’t look like normal healthy brains do, even while resting from tasks).
Those minutes to hours of restricted blood flow during a TIA can be enough to cause dysfunctional neurovascular coupling, which is the relationship between your neurons and the blood vessels that supply them.
In short, neurovascular coupling is how neurons get the oxygen and other nutrients they need to function. When that relationship is disrupted, an area of the brain may start a task and fail to complete it due to a lack of resources. Or, it might call for more blood supply than it should, depriving other parts of the brain of what it needs. On imaging, we see this dysfunction as hyperactive (doing too much or taking too many resources) or hypoactive (doing too little) regions of the brain.
That signaling dysfunction is behind many of the lingering symptoms after a TIA.
But that’s not all. A TIA often occurs deep in the center of the brain. The carotid arteries bring blood to the brain, with smaller and smaller blood vessels traveling to specific subsections, like tree branches.
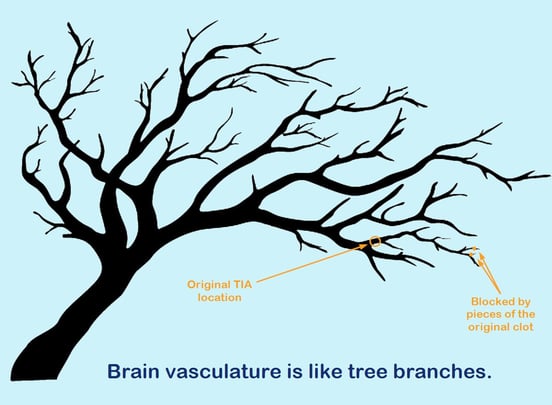
After the blockage breaks up, pieces of the clot may travel down the smaller blood vessels (capillaries) until becoming lodged in place again. As a result, you may have a cluster of brain cells that die when they no longer receive fresh oxygen.
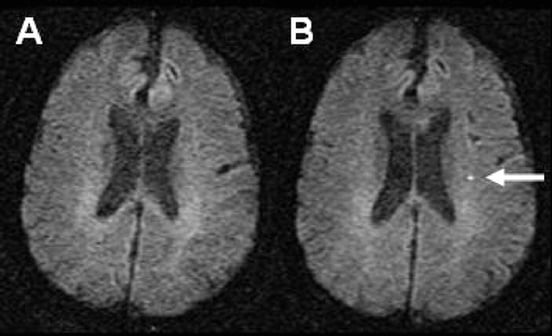 In this figure, we see a patient before (A) and after (B) a TIA caused a small cluster of dead brain cells. Source.
In this figure, we see a patient before (A) and after (B) a TIA caused a small cluster of dead brain cells. Source.
If the TIA causes any brain cells to die, it shows up as little white dots on magnetic resonance imaging (MRI) of the brain, as shown above. A neuroradiologist might see that spot and note it as “nonspecific findings” because that tiny cluster of dead cells won’t kill you. But remember, those cells were doing something before your TIA. And now, some other part of the brain has to compensate for the cells that died.
Recovering from that damage means teaching the brain to route communication around the damaged areas and restoring healthy neurovascular coupling.
How Long Does It Take to Recover From a Transient Ischemic Attack?
TIA patients usually feel better within a couple of days to a couple of weeks after the event. But if you’re having lingering symptoms, it’s hard to say exactly what recovery will look like. It depends on which parts of your brain are injured, how well your brain learns to route around them, and how good your treatment program is.
That said, we’re firm believers that you can always keep recovering if you work at it, even when you’re finished with therapy.
Where to Get Treatment for Lingering Symptoms After a TIA
Patients with lingering symptoms after a TIA need cognitive and physical therapy to make the most progress.
Brain injury is never one size fits all. The specific regions of your brain that were affected by the TIA won’t be the same as the next patient who walks through our clinic doors. Having one standard treatment option produces lackluster results for patients because it fails to take into account their unique needs.
That’s why we use functional neurocognitive imaging (fNCI), a special type of fMRI, with all of our patients. It shows us which specific brain regions are hyperactive and which are hypoactive. We can then tailor patients’ treatment based on their specific scan results, rather than stringing together a few therapies and hoping it works.
The interconnectedness of the brain means that a multidisciplinary approach to treatment is the best. It’s tempting to find a therapist who handles only one issue. For example, patients who notice memory problems will find a cognitive therapist and work specifically on memory.
But “memory” is more than just improving your recall ability. Creating and retaining a memory involves other processes like sensory processing, attention, and executive functioning. If those processes are affected by your brain injury, then attempts to “fix” your memory have to work on those processes, too.
That’s why we offer a combination of therapies based on our patients’ needs, including neuromuscular therapy, cognitive therapy, occupational therapy, sensorimotor therapy, and more.
You can learn more about what a week of treatment looks like here.
Note: Most of the patients we treat have post-concussion syndrome, so most of our online resources are written with them in mind. Many of those resources apply to TIA as well. The reason is that, while concussions are the most common cause of neurovascular coupling dysfunction, they’re not the only cause. We’ve successfully treated TIA patients because the same issue (problems with NVC) is causing the symptoms. It doesn’t matter how you injured your brain; if your symptoms stem from NVC dysfunction, we can help.
Conclusion
Yes, lingering symptoms happen after a TIA. Yes, a TIA can sometimes result in small clusters of dead brain cells. But that doesn’t mean your symptoms are permanent. Even severe traumatic brain injury (TBI) patients can make remarkable progress after their injury with good treatment and perseverance.
The TIA patients we treat often make significant improvement in symptoms because their brain damage is not widespread, nor is it irreversible.
If you want to learn if we can help you, book a consultation with our team. 95% of our patients experience statistically verified restoration of brain function after treatment at our clinic.
Relevant Reading: Mini-Stroke Treatment: Why Symptoms Linger and What Actually Helps













