Are you still experiencing post-concussion syndrome symptoms even after resting like your doctor recommended? If you’re frustrated, tired, and in pain because your concussion symptoms won’t go away, you’re not alone.
Although rest is the most common recommendation for recovering from concussions, science has shown that rest isn’t the best option.
The reality is that physicians often aren’t equipped to provide patients with the robust post-concussion treatment needed for full recovery. At Cognitive FX, we’ve built a large, multidisciplinary team of clinicians trained to treat patients who have suffered one or more mild traumatic brain injuries.
Post-concussion syndrome recovery takes time, and walking into the clinic and starting therapy is just the beginning. Because of that, we provide patients with continued support and “homework” to help them keep getting better at home.
Seeking treatment can sometimes be the most difficult phase. Getting started is never easy, especially if you suffer from mood changes, headaches, anxiety, or any number of other common symptoms. Since knowing what to expect will help you prepare and plan for treatment, this post covers:
If you’re experiencing symptoms that won’t resolve after one or more head injuries, you’re not alone. And you’re not crazy. On average, our patients improve by 75% after treatment at our center specializing in post-concussion therapy. To see if you are eligible for treatment, sign up for a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
Do You Have Post-Concussion Syndrome?

Naturally, the first step to recovery is to establish whether you have post-concussion syndrome (PCS) before pursuing treatment. PCS can be difficult to diagnose because (a) the symptoms overlap with other common medical conditions, and (b) PCS does not show up on traditional MRIs. For example, we often see patients who may have post-traumatic stress disorder (PTSD) and/or post-concussion syndrome. Teasing out the differences isn’t easy; many patients with PCS are misdiagnosed when they seek help because of this reality.
The main criteria for diagnosing PCS are:
- A history of one or more head injuries (does not require loss of consciousness or post-traumatic amnesia)
- Multiple PCS symptoms
- Persistent symptoms for at least 6 weeks after head trauma.
While multiple previous concussions could be a risk factor for developing post-concussion syndrome, PCS can develop from just one head injury.
All of the following are physical and cognitive symptoms of post-concussion syndrome:
|
|
|
|
|
|
|
|
|
- Car sickness or nausea with motion
|
|
|
|
|
- Change in (or loss of) taste or smell
|
|
|
|
|
- Delayed response to questions
|
|
|
|
|
|
|
|
- Difficulty finding things
|
|
|
|
|
|
|
|
|
|
- Slow to decide, think, speak, or act
|
|
|
|
|
|
|
|
|
|
|
|
|
These symptoms are often from a combination of post-concussion complications:
If you are experiencing persistent symptoms after hitting your head, jostling your head, or experiencing whiplash, it’s important to seek medical treatment. If you think you have PCS and want to talk to an experienced health care provider about your symptoms, schedule a consultation.
Further reading: How to recognize post-concussion syndrome in pediatric patients
Post-Concussion Syndrome Recovery Time
 Sam Gray poses outside Cognitive FX, where he received treatment for post-concussion
Sam Gray poses outside Cognitive FX, where he received treatment for post-concussion
Recovering from post-concussion syndrome (also known as post-concussive syndrome) can take time, and the “right” amount of time is unique to each person. Most patients do not recover without treatment. After treatment, some patients feel better immediately; others need weeks, months, or even a year to transition back to normalcy. The extent of your injury, the roadblocks you face in daily life, genetics, and many other factors play into recovery.
Here’s the good news: Recovery is still possible decades after the injury that caused your symptoms. For example, Sam Gray recovered from his mTBI 33 years after injury. And Aimee had been suffering with symptoms for 17 years after her accident.
Brain damage from Aimee’s severe traumatic brain injury (TBI) caused personality changes, constant headaches (“I took migraine medications like they were candy,” she recalled), memory problems, exhaustion (even narcolepsy), dizziness with workouts, light and sound sensitivity, and more. After treatment, her life has turned around completely. “When I left on Friday, I was so excited that I couldn’t contain myself; I just wanted to talk! It’s been two months now, and I can still remember all the pictures they laid out for me to help me remember things, even though they were pretty insignificant to me.”
Taking things at the right pace for you can be extremely difficult, but try to have patience with yourself. It doesn’t matter if you have a longer recovery time than someone else. The important thing is to stay hopeful and keep working to get better.
Post-Concussion Syndrome Treatment

Although some of the recovery process must happen at home, it’s important to seek professional diagnosis and treatment if you suspect you are suffering from post-concussion syndrome. Recovering from post-concussion syndrome is a delicate process that requires the expertise of multiple professionals and needs to be tailored specifically to your injury and needs.
While we can’t speak to the experience you’ll have elsewhere, we can tell you about treatment and recovery at Cognitive FX.
Before you schedule, we’ll talk to you about your experience and schedule treatment if we think you’re a good fit for the program. We collect medical history, symptoms, and other pertinent information prior to your arrival at the clinic for one or two weeks of intense treatment.
Before Therapy, Everyone Gets a Scan
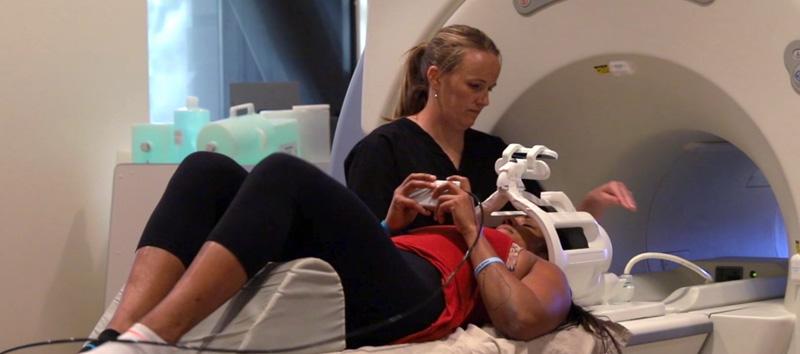
The week begins with a functional Neurocognitive MRI (fNCI). This scan, which examines 56 brain regions and the communication between them, identifies the areas of your brain that were most impacted by mild head injury. fNCI shows how well your brain is communicating based on neurovascular coupling (NVC). Neurovascular coupling is the connection between the neurons and the blood vessels that bring them oxygen and other resources. Irregularities in NVC after mild traumatic brain injury causes alterations in brain function which concussion patients experience as symptoms. With an fNCI scan, the doctors at Cognitive FX can customize treatment to target the specific areas of your brain that were most impacted by your injury.
You’ll also receive a standard MRI of your brain and cervical spine, just to make sure that there is no unresolved physical damage standing between you and recovery during treatment. While rare, some people do need other interventions (such as neurosurgery) to address those injuries before they can complete treatment for PCS.
Most patients are nervous on Mondays (when you get the initial scan) and Fridays (when you get your post-treatment scan). Some cry out of relief; others get angry when seeing their results for the first time, saying, “I have been trying to tell people something was wrong but my doctors kept saying I was fine!”
One patient, Lynette, decided to get an fNCI scan to learn if she had PCS and what she could do about it. “At that point, I became incredibly emotional, because for the first time in my life, I realized that I had some hope. I thought I was going to have to live the rest of my life with a foggy brain and a massive headache all the time.”
After the initial scan, we tailor your treatment plan to address your specific symptoms. Treatment of post-concussion syndrome involves various multidisciplinary therapies, including vision therapy, occupational therapy, cognitive therapy, neuromuscular therapy, sensorimotor therapy, neurointegration therapy, and psychotherapy.
How Treatment Promotes Physical Recovery

Each patient then starts treatment at 8 a.m. and ends at 6 p.m., with a few breaks and lunch scheduled between the various therapies. The process is intense, but effective.
Exercise is a key part of the concussion treatment and recovery process. During treatment at Cognitive FX, patients complete cardio exercise and interval-style training. Many patients are scared to exercise if physical therapy has made their symptoms worse in the past. But workouts are a critical part of recovery — exercise improves blood flow in the brain and releases a cascade of helpful neurochemicals, which means your brain gets better results from therapy.
Exercise also decreases sympathetic nervous system over-activation, a condition responsible for many symptoms of PCS. Exercise can also improve dizziness, nausea, headaches, and issues with balance and coordination. Our therapists know how to guide patients’ exercise without pushing them too hard. It isn’t easy, but the outcome is worth it.
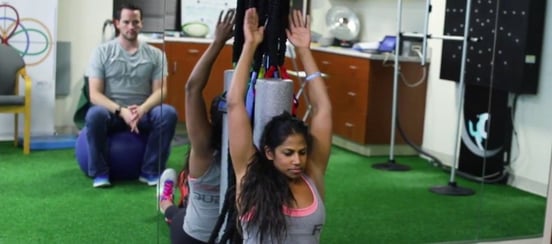
For example, a young woman came to our clinic who was terrified of running. Every time she ran, the jarring movement hurt her head and made her symptoms skyrocket. So we started her on a stationary bike for the first few days. Near the end of treatment, her therapist got her to try the treadmill again. A few minutes in, she started crying — not because she was scared or in pain, but because she was able to run again without problems!
Another patient who came to Cognitive FX had so much trouble walking that she arrived in a wheelchair. She could walk with a walker, but not very far. After a week of therapy and slowly pushing through her limitations, she was able to leave without even needing a walker.
This patient’s story is a great example of the healing anyone can find with the right medical care. As long as you don’t have any structural damage to the brain (e.g., stroke, major issues from a TBI), you can get better. (Patients who suffered brain damage from a severe TBI can recover, but their outcomes are more dependent on which brain regions were injured and how well we can ‘route around’ those areas. Click here to learn more about recovery from a severe TBI.)

In addition to neuromuscular therapy, patients complete neurointegration therapy, sensorimotor therapy, and occupational therapy. With these therapies, a patient completes exercises designed to target and improve specific areas of the brain. Although these are physical exercises, they improve the four main categories of symptoms: physical, emotional, mental, and sleep.
For example, you might find yourself balancing on one leg and touching numbers as they light up on a board, an exercise that helps with vision and balance. Later in the week, you might balance on the flat side of a Bosu ball while playing throw and catch with a trainer, all while solving cognitive puzzles. The patient we mentioned earlier, Sam Gray, loved how it addressed his needs:
“The point is that you're occupying the parts of your brain that, at least in my case, I had mapped around and was supposed to use for balance and catching but that I was using for things like word retrieval as well as balance. But I wasn't using the correct part of my brain for word retrieval and memory. So that exercise was forcing my brain to use the correct parts for word retrieval and for memory,” he explained.

Patients are often shocked by how much these exercises help with everything from chronic pain in the neck and shoulders to sleep disturbances.
How Treatment Promotes Mental and Emotional Recovery
In addition to physical changes, patients often need mental and emotional support as well. The brain controls our thoughts and emotions. Naturally, when the brain is injured, our mental abilities and emotional control are impacted also.
During treatment, patients will complete therapy to improve symptoms around processing speed, attention difficulties, sensitivity to noise, memory problems, and other cognitive issues. Exercises might include tasks like recalling numbers and then reciting them back in ascending order or inverse order, recalling 20 to 30 photos by relating them through a story, and many other cognitive activities.

Suffering from post-concussion syndrome can often be an emotional roller coaster on top of any emotional symptoms caused by the injury. Patients complete a full psychological evaluation and at least two psychotherapy sessions during treatment.
Even the treatment process itself can be an emotional time. Treatment is intense, and many patients have staked a lot on this treatment. It’s easy to put too much pressure on yourself or get frustrated by your limitations. Breakdowns happen — and that’s okay. Our therapists accompany each patient on their journey through treatment. They are there for you as you navigate the emotional difficulties associated with post-concussion syndrome.
If the psychologist believes your mental health struggles require further attention, you will receive recommendations for follow-up in your area of residence. In the meantime, here are a few resources on common neuropsychological changes after concussion:
The Role of Medications in Post-Concussion Syndrome
When PCS patients visit a doctor, they’re often given multiple prescriptions and supplements designed to mitigate individual symptoms. They might be given antidepressants, pain medicine, anti-nausea meds, blood pressure medication, and more. All those medications come with possible side effects, place strain on the liver, and often are not metabolized normally by the injured brain.
As a result, while some patients occasionally benefit from certain medications, the vast majority who come to us are suffering even more because of the medications they’ve been taking. For a detailed discussion on the topic — including precautions PCS patients need to take, when medications are helpful vs not helpful, and more — see our post on medications and post-concussion syndrome.
Further reading: What a neurologist can do for post-concussion syndrome
Post-Treatment Recovery

We’ll follow up with you several times over the first six months to make sure you’re on track and to answer any questions you might have. And if you ever get another concussion, we’ll work with you to handle recovery remotely so that you (hopefully) don’t need to come back to the clinic for additional treatment.
Post-treatment recovery often moves through phases. To make things easier, in this post, we’ll call them the “shock phase” and “acceptance phase.”
‘Shock Phase’
We’ll refer to the first 1-4 weeks after treatment as the “Shock Phase.” After you complete intense treatment, you have to return to normal life.
Being thrust from the treatment setting back into normal life can be a bit of a shock. We send every patient home with exercises that will help their brains keep the new improvements they gained during treatment. It’s important to continue with the recommended follow-up exercises and to get at least 30 minutes of physical exercise every day.
Some patients have doubts and frustrations about their progress during the first few weeks. If this happens to you, it’s not because you’re regressing, but because your body is adjusting to a new normal. Do your best to stay positive — giving in to negative emotions and thought patterns will activate the sympathetic nervous system, leading to an increase in your symptoms.
One patient, a young man, did very well during treatment but was always nervous. He had a particularly difficult flight home, and his symptoms began to increase. Soon, he called the Cognitive FX team, worried his brain had returned to its pre-treatment state. With follow-up support, he was able to understand that fluctuations in symptoms are normal at first. As he continued to complete his at-home exercises, he continued to improve.
Patients universally benefit from having a family member or friend with them during and after treatment. Our loved ones can provide a much-needed perspective on the changes occurring as you heal. It can be difficult to recognize your own progress day-to-day, but others can encourage you and share their observations on how far you’ve come.
Finally, while many patients experience an increase in energy during treatment, it’s completely normal to be fatigued afterward. It’s a big effort and requires time for your body to recover. Realize that fatigue is a normal response, and have patience with yourself.
‘Acceptance Phase’
During treatment, we induce rapid changes in your brain in a short period of time. Adjusting to these changes can bring new challenges and opportunities. Your life before treatment probably won’t look like your life after treatment. Managing that transition is what we call the “acceptance period.” This phase can last anywhere from one month to almost a year.
Many patients lean on routines and coping mechanisms to manage post-injury neurological impairments. After treatment, many of those symptoms will no longer hold you back from doing what you want to do. You will have to decide who you want to be and how you want to spend your time, while still giving yourself breathing room to recover at the rate your body requires.
As you adjust to your new life, you may never feel like the same person you were before or during your illness again. It’s important to accept and embrace the new you. It can be difficult to let go of the past and move forward, but maintaining a positive attitude, setting goals, and surrounding yourself with a good support network can help.
During this phase, your family members, friends, and acquaintances will also have to adjust to your changes. A spouse or friend may have gotten used to your coping mechanisms and will need to adjust to the new way you handle daily activities and the challenges that come with them.
Just remember — change is difficult, but it’s an opportunity for the better. Use this time to reflect on who you are and how you can use your improved health to live in a way that’s meaningful to you.
Misconceptions About Recovery

The healing process doesn’t happen overnight. Setting the wrong expectations can lead to disappointment and ultimately hinder your healing.
One of the biggest misconceptions about PCS recovery is that you won’t ever go backwards. It’s not uncommon for your progress to have some ups and downs. It may be difficult to see in the moment, but the overall trend tends to be one of improvement. You may feel emotional when symptoms start to return or worsen, but that’s a normal part of the recovery process. If your symptoms are progressively getting worse over a long period of time, you should reach out to your physician (or, if you’ve received treatment at Cognitive FX, follow up with our staff).
You won’t get better all in one week. Treatment at Cognitive FX is meant to be the beginning of your recovery, not the end. Continuing treatment by completing your follow-up exercises and recommendations is important.
There may be a new normal. We are shaped by our life experiences. Don’t be disappointed with your progress if you’re not 100% “where you were before.” A positive outlook will aid recovery. You will experience improved quality of life — but much of that hinges on how you approach recovery.
It isn’t all physical healing. You may find it helpful to seek and continue psychotherapy after completing PCS treatment. Negative emotions can keep the body locked in fight-or-flight mode, a state that only exacerbates mild TBI symptoms and prevents healing.
It is never too late. If you are suffering from post-concussion syndrome years after a seemingly minor head injury, it’s not too late to seek treatment and start the recovery process. We offer a consultation to talk about your situation and get you started on the path to recovery.
Post-Concussion Syndrome Support Group

Having a good supportive group of people around you can also help to enhance your recovery. It is often difficult to “see the forest through the trees” while recovering.
If you can, surround yourself with supportive people who encourage you when recovery is difficult. It’s often most difficult for us to see changes in ourselves, while others perceive them easily. Recovery is an emotionally difficult process and having support along the way can help make the process smoother.
You may find it helpful to join a post-concussion syndrome support group. To provide community and support, Cognitive FX has a Facebook group for patients who have completed treatment.
How to Enhance Post-Concussion Syndrome Recovery

You are the most important part of your recovery. Although it takes a supportive group of people, physicians, and other experts, ultimately, each person’s recovery is in their own hands. This doesn’t mean you’re not getting better because you’re not trying hard enough, but it does mean your decisions and behaviors can lead to a better outcome.
Keep a positive attitude.
One of the most important recovery enhancers is a positive attitude. With post-concussion syndrome, the sympathetic nervous system is overactivated. Maintaining a positive and peaceful attitude may be a struggle because of your symptoms, but it will help to calm your nervous system and make recovery easier. A positive attitude can help to enhance every area of your recovery.
That said, you don’t need a false sense of positivity, just an open mindset and can-do attitude. By keeping your mind open and committing to trying your best, you will help enhance your recovery.
A healthy sense of skepticism is okay and is quite normal for most patients. Having tried many other “treatments” or therapies, patients often have a difficult time allowing themselves to believe they can get better.
Keep a journal.
Keeping a journal can help you to maintain perspective on your progress and stay positive. Over the course of a few weeks, for example, you may still get headaches after going out and socializing, so you may think you aren’t progressing. But by noting how long you can stay out, you might see that over a two-week period, you’ve gone from having to leave after 20 minutes to spending over an hour socializing with friends. Without those specifics, you could completely miss some of the progress you’ve made.
Give yourself permission to heal.
It can be difficult to move forward after struggling with so many symptoms of concussion for a long period of time, but it’s important to embrace your progress and allow yourself to get better. Slowly getting back into your normal life can help. By gradually returning to normal, the brain and the body are able to adapt and thrive, decreasing fears and doubts that might otherwise hinder progress.
Stay consistent.
Post-concussion recovery doesn’t happen overnight; consistency is important. After completing treatment, it’s important to continue daily exercise, seeing a psychotherapist if recommended, and completing any other exercises or “homework” as recommended specifically for you by the Cognitive FX team.
Fuel your brain.
Certain foods and vitamins are ideal for a healing brain. Learn more in our post about nutrition for post-concussion syndrome recovery.
Further reading: Recovery from sport-related concussions
Recovery Stories from PCS Patients

Myrthe van Boon took time after treatment to keep exercising and slowly re-integrate into society. She kept things in perspective and was thrilled with the progress she made.
If you’d like to learn more about other patients’ recovery journeys, you may enjoy the stories some of our other patients have shared. Here are a few links to get you started:
- Quieren is a Cognitive FX patient from the Netherlands who suffered from PCS after a bike accident.
- Sam Gray (mentioned earlier in this post) sought treatment 33 years after a brain bleed.
- Myrthe van Boon is a mother of two who struggled with debilitating post-concussion symptoms for years before finding Cognitive FX.
- Olivia Seitz is a former figure skater who found symptom relief after more than a decade of chronic illness.
- Sam Pembleton was an adolescent hit by a soccer ball in the head; she tried treatment methods for five years before finding Cognitive FX.
- These patients all completed video testimonials about their initial injury and their experience at Cognitive FX.
Every recovery story is unique, because each person is unique. But PCS patients face many shared challenges — and they’re always easier to face when you’re not alone.
If you think you have post-concussion syndrome, schedule a consultation. Not all treatment options are created equal; we pride ourselves in having the strongest PCS treatment program in the world and would love to be a part of your journey to recovery.






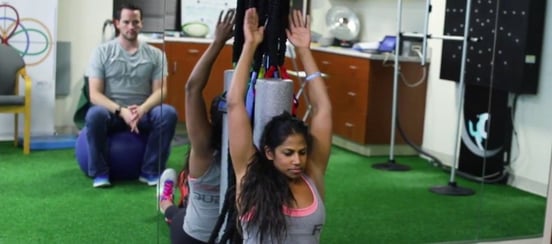











.jpg?height=175&name=Slow%20Concussion%20Recovery%20(6).jpg)





