Post-concussion syndrome is an “invisible” illness.
You can’t see the damage to the brain. You look normal from the outside. You may be very good at masking symptoms when you’re in front of other people.
Worst of all, your doctors might not even take you seriously, because you “seem” fine, and your brain scans and standard blood work are normal. The people around you might question why you’re not back to school or work, or accuse you of making things up for attention.
Dealing with the burden of persistent, unusual symptoms and the pressures of society to “just get better already” is too much for anyone to shoulder alone.
Hopefully, someone in your family or circle of friends is able to be there for you. But it can also be a great relief to find peer support from people who have gone through what you have, can listen without judgment to your story, reaffirm that you’re not crazy, and offer recommendations based on what helped them in their own recovery journeys.
A good support group can offer:
- A safe place for you to ask questions and tell your story.
- A way for you to learn coping strategies from other PCS patients to improve your quality of life.
- Recommendations regarding treatment types and providers.
- “Accountability buddies” for people who want to build healthier habits to take care of their brains.
Unfortunately, not every support group is a healthy environment. Some may be very negative, with participants focused more on what’s been lost than on looking to the future, or on criticizing other members for the way they’re handling their symptoms. Needless to say, this could have a negative (rather than positive) impact on your mental health.
Some also have rules against sharing treatment recommendations and strategies — which is fine if you just want a place to talk, but could be a missed opportunity to work on improving your health.
In this post, we’ll share what to look for in a post-concussion syndrome support group, along with information on our support group and treatment program. If you’re a caregiver and want information on supporting your loved one through a brain injury, read our post on how friends and family can help brain-injured patients.
If you’re experiencing concussion symptoms that won’t resolve after three months, you’re not alone. And you’re not crazy. On average, our patients improve by 75% after treatment at our center specializing in post-concussion therapy. To see if you are eligible for treatment, sign up for a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
How to Find a Good Support Group for Post-Concussion Syndrome (PCS)

There are good support groups for brain injury survivors online and in person. You may find it helpful to join both so you can get recommendations for local specialists (such as who’s the best vision therapist in town) while still learning from a larger, online group.
Whether you’re meeting online or in person, a good group should be positive and practical:
- Positive: It’s healthy to talk about how hard it is to live with PCS, but the group should also have people who encourage each other and celebrate success stories. It’s hard enough to stay calm and hopeful when you may be dealing with both physical and emotional symptoms; you don’t need a group that doesn’t lift you up.
- Practical: It’s OK if you just want a group where you can exchange stories and get emotional support. But if you want a place where everyone is free to link to resources they found helpful, share what worked and didn’t work for them, and recommend doctors, make sure you know what the group’s rules are before you join. A quick glance at their ground rules will help you know what kind of group you’re joining — some insist that since they aren’t medical professionals, they don’t want to make any treatment recommendations.
It’s OK to leave a group if you don’t think it’s a healthy environment for you. Use your feelings as a litmus test: Does interacting with the people in the group make you feel anxious? Do you leave every meeting with a tight neck or stomach ache? If so, it’s probably not a good group for you.
But if interacting with the people in the group makes you feel emotionally better, like you have a plan or at least don’t feel alone, then it’s a good group.
Where to Look for a Post-Concussion Support Group
If you live in the United States and want to find an in-person group, start your search with the Brain Injury Alliance. Each state has different resources; most of them should have information on what brain injury support groups exist and how to join them.
They may also have resources for family members. The group you find may be for more than just people with concussions, such as for anyone who has lingering symptoms after a mild or severe traumatic brain injury (TBI).
If that doesn’t work, try asking local concussion clinics and sports doctors if they have any recommendations. They may have more resources than a pediatrician or general physician.
If you’re looking online, there are many Facebook groups for acquired brain injury and for post-concussion syndrome specifically. Some are moderated by nonprofits, and some are run by people who previously or currently suffer from brain injury symptoms.
You can also join one of the online support groups run by Cognitive FX…
Cognitive FX Support Groups and Treatment

We moderate two completely free support groups:
- The Cognitive FX Graduate Support Group. This group is for patients who have gone through treatment at our clinic (which you can learn more about below).
- The Post-Concussion Support Group. This Facebook group is open to anyone who has lingering symptoms after a concussion or other head injury who wants information and support from others like them.
Our graduate support group is an active community (over 700 members!) in which patients swap recovery stories, ask for situational advice, and discuss how to continue improving in health.
Some topics that graduate group members recently posted about include:
- What to do if you hit your head and your symptoms return.
- Wearable device recommendations to help with fitness and mindfulness.
- What to do if motion sickness returns during activities such as kayaking.
- Strategies to handle POTS (a type of dysautonomia that some brain injuries result in).
We also host weekly webinars on topics that group members want to learn more about. Some past topics include patient stories, what to do at home after treatment, the autonomic nervous system, neuromuscular therapy, and general Q&As.
You can post on any relevant topics and share whatever resources you found helpful in both groups. Although it’s rarely needed, we do moderate the groups to remove strong language and personal attacks if they occur.
Remember to Give Grace (to Yourself and Others)
Whether you’re finding your place in a support group or walking your own recovery path, remember to give yourself grace ... and extend it to others, too.
You and others in a support group are still healing. So if someone in your support group says something callous or offensive, try not to take it personally. They’re also dealing with a brain injury and may not have a good “filter” on their thoughts.
Also keep in mind that people who have never had a brain injury don’t understand what you’re going through. They likely have good intentions, but they may say things you find hurtful because they don’t understand what you’re going through or that their advice isn’t helpful.
So stay supportive of yourself and others, keep working to recover, and be grateful for every step in the right direction, along with those who help you on the way.
Speaking of recovery, we’ve included more information about how to get treatment for post-concussion syndrome, if you’re interested in learning more:
Want to Learn More about Cognitive FX?
Many patients don’t have access to appropriate treatment for post-concussion syndrome. This is due to many factors:
- Many doctors don’t know about post-concussion syndrome, let alone how it’s treated.
- Doctors who do know about PCS don’t usually have the resources to employ the therapists needed for in-house treatment, but sending patients to three to four different therapists isn’t usually feasible (or as effective).
- Most doctors don’t have reliable brain imaging to aid diagnosis and treatment.
At Cognitive FX, we have everything needed for PCS diagnosis and treatment in house. Our patients come to us from across the United States and around the world.
Every patient who goes through our program receives brain imaging called functional Neurocognitive Imaging (fNCI), which is a type of functional MRI. It identifies which regions of your brain were affected by your mild traumatic brain injury (or any other brain injury) and whether those regions are hypoactive (not engaging as much as they should) or hyperactive (either using too many resources or trying to do too much).
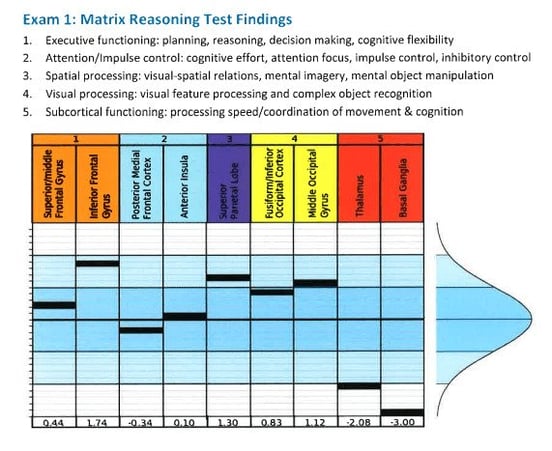 An example from the fNCI report. This patient’s thalamus and basal ganglia were both hypoactive.
An example from the fNCI report. This patient’s thalamus and basal ganglia were both hypoactive.
We use this information to tailor your therapy according to the brain dysfunction you, specifically, are experiencing. Patients complete a period of intense treatment, including therapies such as cognitive therapy, neurointegration therapy, sensorimotor therapy, neuromuscular therapy, vision therapy, psychotherapy, and more.
At the end of treatment, you’ll receive another fNCI scan to confirm the progress your brain has made.
A number of our patients have talked about their experiences at the clinic and what their recovery journey was like. You can read stories from seven of them here.
If you’re looking for resources to learn more about post-concussion syndrome, its symptoms, and treatment options, here are a few posts to get you started:
Want to see if you’re eligible for treatment? Tell us more about yourself and schedule a consultation call with our team.














