What to Do When Therapy Isn't Working for Depression
Psychotherapy helps many people with depression — but it isn’t effective for everyone. For example, a large clinical trial found that nearly 60% of participants still met the criteria for major...

For many people with anhedonia, life feels like the color has drained out of the world. Activities they used to enjoy — music, food, hobbies, relationships — suddenly feel flat. They can still feel stress, anger, or anxiety, but the spark of interest and reward is gone.
What makes anhedonia even more difficult is how often it’s misunderstood. Many patients are treated as if they’re depressed, even when they’re not. They may receive standard depression therapies or serotonin-based antidepressant medications that don’t meaningfully affect the dopamine-driven motivation and reward system at the root of anhedonia. As a result, they see little improvement and often feel discouraged or misdiagnosed.
Anhedonia is increasingly recognized as a standalone condition, and modern life may be contributing to its rise — from chronic stress to the constant “dopamine hits” of digital devices that disrupt our natural motivation and reward pathways.
This article explains what anhedonia is (and isn’t), why conventional treatments may fall short, and what targeted options — including behavioral activation therapy, dopamine-focused medications, and newer neuromodulation therapies like transcranial magnetic stimulation (TMS) — can help reactivate the brain’s motivation and reward system.
Table of Contents
Anhedonia is often described as the inability to experience pleasure, but this description is incomplete. Clinically, anhedonia refers to a disruption in the brain’s reward system — specifically the pathways responsible for motivation, anticipation, and the emotional “reward” that normally follows enjoyable activities.
Understanding what anhedonia is not is just as important as understanding what it is, because misinterpretation can lead to the wrong type of treatment.
People often disengage from hobbies, creative pursuits, exercise, social events, or routines that once provided a sense of pleasure or accomplishment.
Even when patients intellectually think an activity might be rewarding, they feel little motivation to start it. This often reflects a disruption in the anticipatory side of the reward system.
Rather than sadness, many describe anhedonia as an absence of positive emotion—no spark, no anticipation, no satisfaction. Other negative emotions, such as anxiety or irritability, may remain fully intact.
For some with anhedonia, social interaction no longer feels of interest or rewarding. They may withdraw not because of social anxiety, but because the emotional “return” from connection is missing.
Some patients with anhedonia report:
Daily tasks can feel disproportionately draining. The effort to engage in activities that used to be fulfilling feels too high. Patients may say they are “tired all the time,” even with adequate rest.
Sleep may become irregular or unrefreshing, and appetite may increase or decrease, depending on the individual.
As anticipation, motivation, and engagement decline, life can begin to feel directionless or empty—even when nothing objectively “bad” is happening.
In more severe cases, the absence of pleasure or purpose can lead to hopelessness and suicidal thinking. This requires immediate attention from a mental health professional.
A crucial feature of anhedonia is its feedback loop: When nothing is anticipated as interesting or fulfilling, and nothing feels rewarding, people naturally disengage. But disengagement further weakens the anticipation and reward systems, lowering motivation even more. This cycle can cause significant impairment in daily life long before a formal diagnosis is made.
These terms are frequently used interchangeably by patients and even clinicians, but each reflects a different underlying issue.
Anhedonia refers to reduced pleasure or reward from activities.
Apathy refers to reduced interest in or initiation of behavior.
A person with apathy may not feel motivated to start activities, but once they do, they might still find them rewarding. A person with anhedonia may want to engage and even remember enjoying something in the past, but now feels emotionally flat or unrewarded by it.
Both can occur together, but they arise from different mechanisms within neurobiology and may require different treatments.
Emotional blunting is a general dampening of emotional experience—positive and negative.
Anhedonia specifically refers to the loss of the experience of pleasure and reward.
A patient with anhedonia can still feel negative emotions such as stress, irritability, anger, or anxiety, yet lack the ability to feel joy, interest, or excitement. Emotional blunting may also occur as a side effect of certain antidepressant medications (especially some SSRIs), which further complicates diagnosis.
Anhedonia is not one single experience. It presents in multiple subtypes, and these distinctions guide both psychotherapy and medication strategies.
Reduced pleasure or reward from social interactions, relationships, or emotional connections with others. Social anhedonia is common in schizophrenia, bipolar disorder, and other mental health conditions, but also appears in individuals without any psychotic or affective disorders.
Reduced reward from sensory or physical experiences such as eating, touch, physical activity, or sexual intimacy. Physical anhedonia can affect daily functioning, physical health, and overall quality of life.
Difficulty anticipating future pleasure. Patients may know an activity “should” be enjoyable based on past experience, but they feel no internal motivation or pull to engage.
Reduced ability to experience pleasure in the moment. Even while doing something previously rewarding—listening to music, exercising, eating—nothing feels enjoyable.
A reduced drive to pursue goals or rewarding activities due to impaired dopamine-mediated reward processing and approach behavior.
Different types of anhedonia do not always respond to the same treatment. For example:
Behavioral Activation targets motivational pathways and is most effective when disengagement and avoidance are prominent.
Dopamine-targeting medication may help when motivational or anticipatory reward systems are affected.
Traditional antidepressant medication (especially serotonin-focused SSRIs) may not significantly improve anhedonic symptoms.
Transcranial Magnetic Stimulation (TMS) may benefit patients with treatment-resistant anhedonia when reward-circuit hypoactivity is identified through neuroimaging.
Understanding which component of the reward system is disrupted allows for a more precise, effective approach to treating anhedonia.
The brain’s reward and approach system — particularly dopamine pathways involving the ventral striatum and prefrontal cortex — developed for environments where anticipation, effort, and reward were tightly linked. Today, that system is exposed to constant, low-effort sources of stimulation:
Digital devices and social media provide continuous micro-rewards: likes, alerts, new content, and novelty.
Online shopping, gaming, and other high-stimulation platforms reinforce rapid reward without effort.
Behavioral addictions (including pornography use, gambling-like digital apps, and compulsive scrolling) mimic the effects seen in substance use disorders by altering dopamine release and receptor sensitivity.
Over time, the reward system adapts by reducing responsiveness, creating a muted or “flat” experience of daily life. This flattening can resemble physical anhedonia, social anhedonia, or both.
Dopamine is not simply the “pleasure chemical”; it drives effort, approach behavior, and anticipation. When rewarding experiences require no effort, the brain’s ability to evaluate and pursue meaningful rewards weakens.
This can impair:
The result is a pattern that looks strikingly similar to motivational anhedonia, even in people without an identifiable mental illness.
Prolonged activation of the stress response—including elevations in cortisol—disrupts neural circuits involved in reward processing. Chronic stress also contributes to inflammation and oxidative changes implicated in mood disorders, post-traumatic stress disorder (PTSD), and substance use disorder, all of which increase vulnerability to anhedonia.
These factors contribute to impaired dopamine function, decreased activity in reward-related regions, and diminished quality of life.
Although anhedonia is increasingly recognized in psychiatry and neuroscience as its own clinical phenomenon, it is still frequently misdiagnosed as major depressive disorder. This is understandable: anhedonia is a well-known symptom of depression, and most mental health professionals are trained to interpret “loss of interest” or “lack of pleasure” through a depression-first lens.
However, because anhedonia is commonly assumed to be depression, treatment typically defaults to:
Selective serotonin reuptake inhibitors (SSRIs), which may improve sadness or anxiety, but do not reliably improve anhedonic symptoms.
Standard cognitive behavioral therapy (CBT) or other forms of psychotherapy focused on negative mood rather than reward-system impairment.
A clinical focus on sadness or low mood rather than the underlying reward-processing deficit rooted in dopamine pathways.
Patients may be told to expect gradual improvement yet feel little change in their ability to anticipate reward, experience pleasure, enjoy daily life, or engage in physical or social activities. In some cases, certain antidepressant medications can even aggravate anhedonia due to emotional side effects, blunted positive emotions, or increased detachment.
Misdiagnosis shapes treatment in ways that frequently miss the core problem. If the central issue is a dopamine-related impairment in motivation and reward processing, then serotonin-focused approaches may have a limited effect. This can lead to:
Meanwhile, more appropriate options — such as behavioral activation, dopamine-targeting medication, or transcranial magnetic stimulation (TMS) — may never be considered.
Recognizing anhedonia as its own condition, not exclusively a common symptom of depression, is a crucial step toward improving treatment outcomes and restoring a patient’s well-being.
The two most common categories of treatment for anhedonia are psychotherapy and medication.
Most people with anhedonia are offered therapies designed for depression, which may focus on mood, thoughts, or past experiences but often do not directly address reward-system dysfunction. The most helpful approaches incorporate structured engagement with rewarding activities and skills to relearn anticipation and enjoyment.
Behavioral Activation is one of the most direct and evidence-based psychotherapy options for anhedonia. It focuses on:
Sessions often include scheduling specific behaviors, troubleshooting barriers, and reinforcing early positive signals from the reward system.
Studies show that BA is an effective way to treat anhedonia because it focuses on restoring engagement, rather than processing emotion or cognition alone. However, many patients only experience partial improvements and never return to their baseline levels of pleasure.
CBT can help address negative beliefs that contribute to avoidance (“Nothing will help,” “There’s no point,” “I’ll never feel anything again”). While CBT on its own may offer only partial improvement for anhedonia, it can support re-engagement when paired with a behavioral approach.
Positive Affect Treatment is a specialized therapy designed to retrain the brain’s ability to anticipate and experience positive emotion. It incorporates:
PAT is a promising option for patients whose primary difficulty is generating or sustaining positive emotional states. By repeatedly focusing on enhancing positive experiences, studies show that this therapy can help patients and reduce symptoms of anhedonia.
Medication can be helpful for some patients with anhedonia, but an effective treatment strategy differs from typical depression care.
Because anhedonia involves reduced motivation and reward responsiveness, medications that influence dopamine activity may be more appropriate than serotonin-focused antidepressant medication. Examples include:
These medications may improve motivation, interest, and reward sensitivity, though responses vary and benefits may take time to appear.
SSRIs are first-line treatment for depression but (as discussed above) are often less effective for anhedonia, as they do not significantly impact dopamine pathways. In some patients, SSRIs can contribute to emotional detachment or reduced positive affect, which may worsen anhedonic symptoms.
They remain appropriate when anhedonia occurs within a broader depressive episode, but expectations should be realistic regarding their impact on pleasure and motivation.
Over the past few years, there has been a growing interest in using transcranial magnetic stimulation (TMS) to specifically treat symptoms of anhedonia. Neuroimaging studies show that the magnetic pulses used during TMS can stimulate underactive areas in the brain that are involved in the anticipation and reward system.
This stimulation can help restore normal brain activity and rewire neural connections, leading to improvements in symptoms of anhedonia and a return of enthusiasm for life.
TMS is a non-invasive treatment that uses magnetic pulses to stimulate the dorsolateral prefrontal cortex (DLPFC)—an area of the brain that handles mood regulation and decision-making.
By essentially “rebooting” underactive circuits, TMS helps restore normal activity patterns and reduce symptoms.
Several studies now confirm that TMS is an effective way to treat patients with anhedonia. Interestingly, some patients show more significant improvements in their anhedonia than in their depressive symptoms after TMS therapy. In addition, experiencing early improvements in anhedonia symptoms is a good indication that patients will have long-term improvements with depression.
At Cognitive FX, we offer an advanced form of TMS called accelerated fMRI-guided TMS. It’s similar to Stanford Accelerated Intelligent Neuromodulation Therapy (the SAINT™ protocol)—which produces some of the highest response and remission rates of any depression treatment.
This form of TMS improves upon conventional protocols in important ways:
Conventional TMS protocols use a manual measurement technique to identify the treatment target site, but studies have shown that missing the treatment target area by even a few millimeters can significantly reduce TMS treatment effectiveness.
At Cognitive FX, we use advanced fMRI brain imaging to identify the exact target site for each patient, and neuronavigation to ensure the magnetic pulses are delivered to that exact spot for every treatment session.
Conventional TMS protocols are delivered with daily sessions over 4 to 6 weeks, making it difficult to complete amidst work and life commitments. In contrast, our treatment is completed in just 5 days.
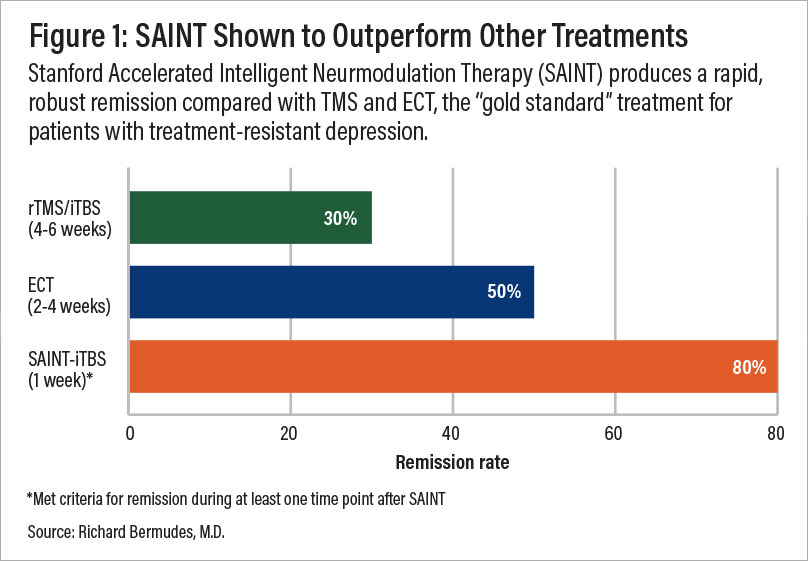
A comparison of remission rates for rTMS/iTBS, electroconvulsive therapy (ECT), and SAINT-iTBS.
There are no studies specifically evaluating SAINT TMS for anhedonia, but in a double-blind randomized clinical trial, about 86% of patients with treatment-resistant depression responded to SAINT, and roughly 79% reached remission. All participants had already failed at least two other depression treatments. One month after treatment, 60% remained in remission.
Our version applies the same core principles—iTBS, fMRI-guided targeting, and a condensed 5-day treatment schedule—but uses our in-house fMRI analysis rather than Magnus Medical’s proprietary software.
Both protocols are safe, precise, and highly effective accelerated TMS approaches, but our fMRI-based targeting keeps costs significantly lower while maintaining precision and outcomes.
Accelerated TMS protocols, including the one we offer at Cognitive FX, are not yet covered by insurance.
We integrate cognitive behavioral therapy (CBT) alongside TMS, which research shows can improve response and remission rates for depression and extend results.
Our program is ideal for adults aged 18–65; we do not treat patients with a seizure history or those in active crisis care.
Click here to learn more about receiving accelerated fMRI TMS therapy at Cognitive FX or take our quiz to see if you’re a good fit for treatment.

Dr. Spangler is a Clinical Psychologist with over 20 years of experience working in both clinical and academic settings. She earned her doctorate degree in Clinical Psychology at the University of Oregon followed by a Postdoctoral Research Fellowship in the Department of Psychiatry at the Stanford University School of Medicine. Dr. Spangler served as a Professor of Psychology at Brigham Young University for 15 years where she directed training in Cognitive Behavioral Therapy for the Clinical Psychology Doctoral Program, and conducted research on the etiology and treatment of depressive, anxiety, and eating disorders. She also served as a Visiting Professor in the Department of Psychiatry Cognitive Therapy Centre at Oxford University in England. Dr Spangler has authored over 60 publications and has lectured worldwide. She has received numerous awards for her collective work from the National Institute of Mental Health, the American Psychological Association, the International Association for Cognitive Psychotherapy, the Association for Behavioral and Cognitive Therapies, the Beck Institute, and the National Association of Professional Women.

Psychotherapy helps many people with depression — but it isn’t effective for everyone. For example, a large clinical trial found that nearly 60% of participants still met the criteria for major...

Many people have had experiences where dark winter days or cold weather have affected their moods. But for about 5% of adults in the U.S., getting through the winter is more than just unpleasant—it’s...

You've waited weeks. You've followed every instruction. And you still feel the same, or maybe even worse. If your antidepressant isn't working, you're not imagining things, and you're far from alone.

If you’re a psychologist or mental health professional, chances are you’ve heard of transcranial magnetic stimulation (TMS)—maybe in the same breath as medications, ECT, or even ketamine. But the...

If your SSRI isn't working, you're not imagining it, and you're not doing anything wrong. You took the medication as prescribed, gave it time, maybe tried a second or third one, and you're still...

Anxious depression, clinically referred to as mixed anxiety depressive disorder (MADD), is a challenging condition to treat. Standard approaches — such as antidepressant medication and psychotherapy...