Recover from Extreme Fatigue from Post-Concussion
It’s not uncommon for people in today’s society to be tired. The demands on our time seem to be never ending. However, there’s a difference between being tired from being on the go all of the time...
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY
Some doctors say it’s absolutely unsafe to drink liquor when you’re recovering from a concussion. Others say it’s safe, but it might set back your recovery. Still others say, “Why not substitute a fancy coffee for your favorite cocktail on your next night out?” (Please don’t do this. We’ll explain why later in this post.)
Why the abundance of opinions? It’s simple: There’s little research on how alcohol and caffeine affect concussion and post-concussion syndrome patients. So the decision-making often falls to the patient. We treat post-concussion syndrome patients every week at our clinic and commonly have conversations with them about this very choice. They want to know things such as:
While we don’t know precisely how alcohol and caffeine interact with an injured brain, we do know some facts that can help you make your decision. From those, we can make deductions about what you can drink and when. We’ll do our best to distill that information into something you can stomach (pun definitely intended).
Here’s a look at what we’ll cover:
If you still have symptoms more than three months after your concussion, you’re not alone. Up to 30% of concussion patients develop persistent symptoms that won’t go away on their own. 95% of our patients experience statistically-verified restoration of brain function after treatment at our clinic. To learn if we can help you, sign up for a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
A concussion, also known as a mild traumatic brain injury (mTBI), occurs when your brain hits your skull due to an external force (a direct hit to the head, whiplash, or jostling can all cause concussion). The impacted tissue may be bruised and inflamed.
While bruising and inflammation in your arm might cause a little discomfort, it’s not a huge issue. But in the brain, it causes a temporary breakdown of brain cells (neurons) in the injured area. The inflammation can put pressure on other areas of the brain. And worst of all, it disrupts communication between neurons and the blood vessels that supply them with oxygen as needed, a connection known as neurovascular coupling (NVC).
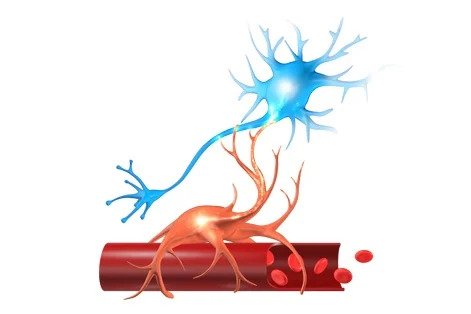
Dysfunctional NVC can take a number of forms. Sometimes, the injured brain region doesn’t get enough of the resources it needs to complete a task. Other times, a region completes its task but uses more than its fair share of resources to do so. Often, healthier regions start compensating for unhealthy regions, eventually becoming overwhelmed by the extra work.
These issues present as post-concussion symptoms such as headaches, difficulty concentrating, brain fog, memory problems, sleep difficulties, balance issues ... The list goes on. And it’s why the brain doesn’t always react to foreign substances such as alcohol and caffeine the way it did before an injury.
For most people, this situation is only temporary. The brain sorts itself out after a few weeks, and patients go on with their lives. But for up to 30% of concussion patients, dysfunctional NVC and symptoms stretch on indefinitely. This condition is known as post-concussion syndrome. To learn more, read our Complete Guide to Post Concussion Syndrome.
In this section, we’ll cover the effects of alcohol on the brain, what symptoms it might worsen, and what to consider before drinking.
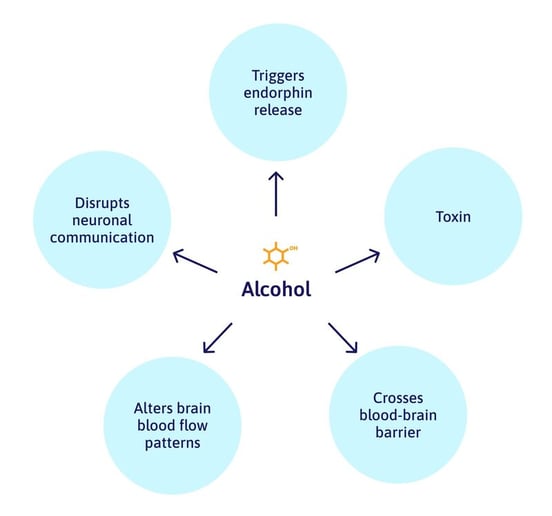
Alcohol is a toxin that can cross the blood-brain barrier and directly affect neurons. While most alcohol is broken down in the liver, a healthy brain also has the ability to break down alcohol molecules locally. If you put a neuron in a petri dish, a high enough concentration of alcohol will kill it. However, the amount you have circulating in your blood after a few drinks is not enough to kill brain cells directly.
That doesn’t mean it’s harmless: Alcohol disrupts communication between neurons in your brain and has been shown on fMRI to alter hemodynamics (blood flow patterns across the brain, aka, neurovascular coupling).
When you become intoxicated (legally defined in many places as a BAC of 0.08%), you may experience a host of effects from that altered neuronal communication: impulsivity and poor decision making, slurred speech, memory loss or problems, reduced motor coordination and slower reaction times, loss of consciousness, and more. Intoxication is behind roughly half of all traumatic brain injuries.
So if it does all these bad things to the brain, why do we like it? Alcohol releases endorphins, which make us feel good.
Not every patient has the same reaction to drinking alcohol. For some patients, how much they drink is indicative of how bad they’ll feel. For others, any alcohol is intolerable.
Here are a few of the ways our patients report reacting to alcohol:
That’s not to say this is a complete list of symptoms — each person is unique and can have varied responses to alcohol. For example, one patient we treated loses sight in her left eye whenever she drinks liquor!
Also keep interactions with medicines in mind. For example, alcohol does not mix well with many anti-depressant medications. Since 35% of post-concussion patients suffer from depression after their head injury, it’s a relevant consideration. Many post-concussion patients also take medicine for headaches and migraines. Some take medications to help them focus. Do you know if your medications interact with alcohol? Find out before drinking.

Every brain injury is different. When we use fNCI (a special form of fMRI) to examine patients’ brains, we see some areas of the brain that are hypoactive and some that are hyperactive. The exact combination, along with factors such as balance and blood flow to the liver, determines a person’s symptoms and how they’ll react to alcohol. If you experience an increase in symptoms while drinking, we recommend against drinking at all.
Animal studies suggest that alcohol impairs recovery from mild TBI; as for human patients, it’s inconclusive. That said, alcohol can interfere with sleep quality. Good sleep is essential for full recovery (whether you’re suffering from acute concussion or post-concussion syndrome). So if you do decide to drink, do it the right way: Don’t drink right before bed, consume it with food, and don’t drink alcohol shortly after traveling to different time zones (the change to your schedule is hard enough to adjust to without adding alcohol to the mix!).
Finally, if you’re having balance problems or issues with motor coordination, wait to consume alcohol until they resolve. Alcohol can make those symptoms worse, putting you at risk of further injury.
Let’s review:
Ultimately, whether or not to drink alcohol during concussion recovery or while suffering from post-concussion syndrome is up to you and your doctor. But you may set back your recovery in the process.
Note: Heavy use of alcohol is common after a TBI. We do not intend to discuss substance abuse in this post. If you need help, try the samhsa.gov helpline.
Let’s say you’ve had treatment at CognitiveFX and want to try drinking alcohol again. When is it safe?
Here’s a good rule of thumb: If you had a bad reaction to alcohol before treatment, wait a while before trying it again. When you do try it, start with just a few sips and see how it goes. A few days later, try a bit more. Keep going until you’re able to have one or two drinks socially without difficulty. Don’t start with shots!
We’ve also been asked if alcohol consumption can reverse treatment. It cannot. Drinking may cause your symptoms to resurface for a time, but it will not undo all your hard work at the clinic. That said, we don’t know how alcohol affects the trajectory of your symptom reduction in the first few weeks after treatment.
If alcohol makes you feel bad, but you still want to drink it, what should you do? Think of it as splurging on a fancy dinner when you’re on a fixed budget. You can do it ... but you might be living on ramen for the rest of the week. Similarly, you can have alcohol even when it increases your symptoms, but it may cost you a few days of feeling under the weather before you’re back to normal.
Caffeine affects a wide range of systems throughout the body and makes several changes to the brain. We’ll discuss what those are, along with how caffeine can increase symptoms for post-concussion patients.
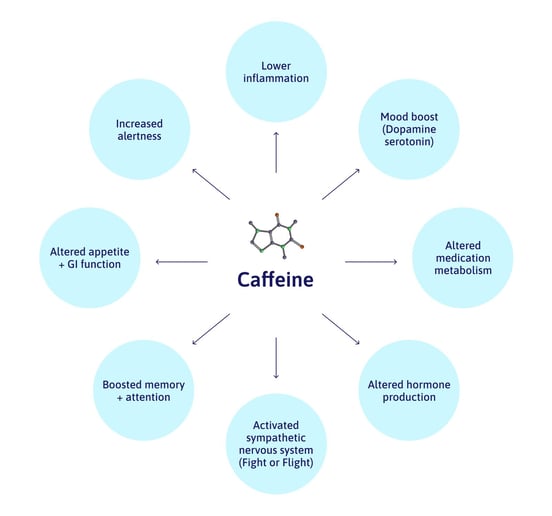
Your brain has a system to determine when you should feel awake vs. sleepy. An important part of that system is a molecule called adenosine. Through complex interactions with your brain, adenosine tells your body to slow down.
Caffeine molecules look like adenosine to your body. But caffeine blocks actual adenosine molecules from doing their job — for a time — so the dampening effect is staved off. Consequently, drinking caffeine will make most people feel alert.
But caffeine isn’t just for feeling awake. It also helps your brain make use of “happy” chemicals such as dopamine, glutamate, and serotonin. Caffeine boosts the action of those chemicals so you feel happier and more energetic.
Caffeine can also interact with your pituitary gland, a small brain region in charge of hormone production with wide-reaching effects across your body. It’s closely tied into your autonomic nervous system; caffeine increases your production of adrenaline, which engages the sympathetic branch of your nervous system (think “fight or flight” response). This connection is why some people notice an increased heart rate when they drink coffee.
Caffeine affects other systems, too. It can temporarily improve your memory and attention span. It might alter your appetite and digestion. And it can affect how your body metabolizes some prescription and over-the-counter medications (it’s very important to discuss caffeine consumption with your health care provider if you’re on meds).
The amount of time caffeine takes to move out of your system is longer than most people realize. The cup you drank in the morning is not almost gone when the effects wear off at 2 pm; it’s actually still in your brain at dinnertime! And if you drink coffee regularly, it produces changes in your brain that take more than just a day or two to revert. Changing your intake (up or down) or the time of day you drink coffee has a noticeable effect on your brain chemistry. If you’ve been drinking coffee for two years and stop cold turkey, your body might be dealing with the effects for weeks, not days.

Coffee can make us feel like a superhero. You get abnormal abilities, such as more energy, improved memory, and a good mood. You might even find physical activity easier. But it’s not sustainable. Those perks come at a cost — one you pay for later (anyone who’s experienced a post-caffeine crash can attest to this). Lower doses of caffeine correspond with smaller consequences. But drink too much caffeine, and you’ll be rewarded with a hard crash when it wears off.
So what happens when you combine caffeine with an injured brain that already doesn’t have enough resources to go around? It depends on the patient. Here are a few reactions we’ve witnessed:
Overall, caffeine + a head injury = not a good combination. Unfortunately, fatigue is one of the most common symptoms of post-concussion syndrome. Those who are well enough to work or attend school often rely on caffeine to manage daily activities.
If you can afford to cut caffeine from your diet while recovering from brain injury, we recommend it — especially if it’s increasing your symptoms. If you have dysautonomia, we strongly recommend avoiding caffeine because it will make the overactivation of your sympathetic nervous system worse.
What if you can’t cut caffeine out? Look for ways to moderate your intake. Think about the form you’re getting it in, too. Super sugary coffee drink? Energy drinks? Green tea? How much caffeine you consume and how you consume it will affect the strength of the symptoms you have in response.

That said, we do recognize that caffeine can have positive effects on the brain, such as reduced inflammation. But any caffeine consumption, especially post-injury, needs to be in moderation. “Moderation” is relative to how much caffeine you consumed before your injury. If your brain is used to two cups of coffee in the morning, then changing your intake suddenly might be more disruptive to your brain than staying the course. Just don’t increase your caffeine dose in response to the fatigue that comes with injury.
If you haven’t had treatment for post-concussion syndrome, be prepared to discuss alcohol and caffeine consumption with your treatment provider. At Cognitive FX, we need to know about consumption history as part of the diagnosis process. For example, caffeine can interfere with diagnostic imaging. We might request that you limit or avoid certain beverages until diagnosis and treatment are complete.
Some people don’t notice severe symptoms after drinking caffeine or alcohol; others find it takes them days to recover after just one drink. Both caffeine and alcohol could set back your recovery, but there isn’t enough research for us to say that definitively.
To help you with your decision, we’ve made a flowchart for deciding when it’s OK to drink alcohol or caffeine (please don’t consume both together) after a brain injury. When in doubt, follow your treating physician’s advice and drink according to CDC guidelines.
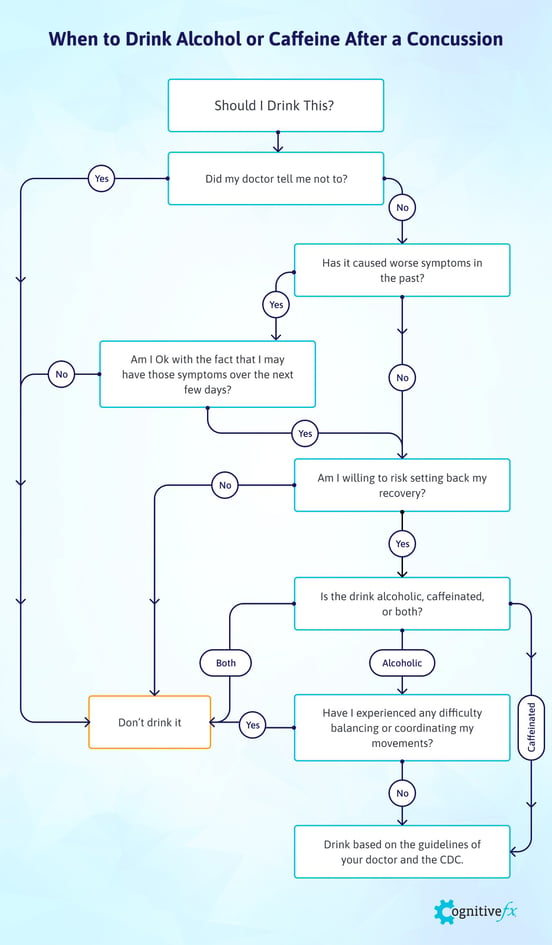
Ultimately, the decision of whether or not to drink comes down to your priorities and your situation — whether you’re taking medications that interact with alcohol or caffeine, how bad your symptoms are, what your tolerance for risk is, and whether you’ve undergone treatment. If you feel your decision-making ability is still compromised, ask a trusted friend or family member to (literally) call the shots.
Note: If you still have symptoms more than three months after your concussion, you’re not alone. Up to 30% of concussion patients develop persistent symptoms that won’t go away on their own. 95% of our patients experience statistically-verified restoration of brain function after treatment at our clinic. To learn if we can help you, sign up for a consultation.

Dr. Mark D. Allen holds a Ph.D. in Cognitive Science from Johns Hopkins University and received post-doctoral training in Cognitive Neuroscience and Functional Neuroimaging at the University of Washington. As a co-founder of Cognitive Fx, he played a pivotal role in establishing the unique and exceptional treatment approach. Dr. Allen is renowned for his pioneering work in adapting fMRI for clinical use. His contributions encompass neuroimaging biomarkers development for post-concussion diagnosis and innovative research into the pathophysiology of chronic post-concussion symptoms. He's conducted over 10,000 individualized fMRI patient assessments and crafted a high-intensity interval training program for neuronal and cerebrovascular recovery. Dr. Allen has also co-engineered a machine learning-based neuroanatomical discovery tool and advanced fMRI analysis techniques, ensuring more reliable analysis for concussion patients.

It’s not uncommon for people in today’s society to be tired. The demands on our time seem to be never ending. However, there’s a difference between being tired from being on the go all of the time...

If you’ve suffered a concussion, you can usually expect to get better over the course of two weeks. (Concussions from sports injuriesaverage7–10 days, while recovery from concussions from other...
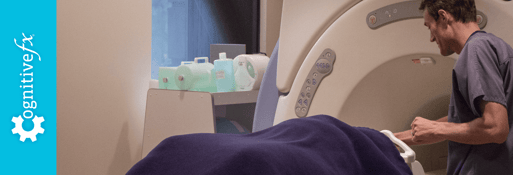
A regular MRI (magnetic resonance imaging) looks at brain structure and integrity. While it helpful for diagnosing structural brain damage, it can’t often be used to detect post-concussion syndrome...
.png?height=175&name=childhood%20head%20injuries%20(11).png)
After a concussion or other type of traumatic brain injury (TBI), some patients experience persistent symptoms for months, or even years. This condition is known aspost-concussion syndrome (PCS),...

Concussions can have long-term physical, cognitive, and emotional effects. Symptoms such as brain fog, headaches, and depression can last for months or years after the initial injury. When the...

Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY