Can’t Sleep After COVID? How to Treat COVID Insomnia (2026)
You lie awake at 2 a.m., exhausted but unable to sleep. When sleep finally comes, strange dreams jolt you awake. Morning arrives and you feel like you never rested at all.
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY
The number of patients with long COVID may be decreasing, but those still experiencing the condition need reliable treatments and resources for recovery more than ever.
The problem is that doctors still don’t know why some patients develop this condition and haven’t agreed on a gold-standard treatment. At the moment, there is no single strategy that helps everyone. The good news is that there are many treatments and at-home strategies that help long COVID recovery. The key is figuring out which ones are the most helpful for your individual situation.
At Cognitive FX, we tailor our treatment approach for each patient. We have been caring for patients with long COVID using a multidisciplinary approach since the first cases started to emerge. We use a state-of-the-art brain imaging scan (fNCI) to determine exactly how the virus disrupted blood flow dynamics and cross-region communication in the brain. With the scan results and information from a rigorous physical and cognitive evaluation, we develop a customized plan for each patient involving exercise, therapy, and rest. We also offer recommendations and resources for patients to use on their own or in conjunction with those offered by other care providers.
To learn more about how and why we developed this method, see our post on long COVID treatment.
In this article, we summarize 18 major treatments and at-home strategies to help with long COVID recovery, including the pros and cons of each.
Of the COVID long-haulers who meet our screening criteria, over 90% show improvement after treatment at our clinic. Our long COVID patients report over 40% decrease in symptom severity in 13 symptoms after just one week of multidisciplinary therapy. To discuss your specific long COVID symptoms and whether you’re eligible for treatment at our clinic, schedule a consultation.
The Centers for Disease Control and Prevention (CDC) defines long COVID as “signs, symptoms, and conditions that continue or develop after acute COVID-19 infection.” This condition can affect multiple parts of the body — such as the heart, lungs, kidneys, skin, and brain.
Despite this general definition, the current understanding is that long COVID should not be seen as a single disease, but as a group of conditions under the same umbrella. This means what triggers symptoms for one patient may not be the same as for another.
From our experience treating long-haulers, one of the main reasons behind symptoms is neurovascular coupling disruption. This occurs when the connection between brain cells and blood vessels in the brain is disrupted. Groups of cells with poor NVC might receive the wrong amount of resources or the right amount at the wrong time, and so forth. As a result, they no longer operate normally, forcing the brain to redistribute its work in an inefficient, taxing manner. Your symptoms may vary depending on which regions of the brain are affected by dysfunctional NVC. You can read more about NVC here.
Another possible explanation for the wide range of symptoms involves COVID-induced dysfunction of the Autonomic Nervous System (ANS). Under normal circumstances, two parts of the ANS — the sympathetic (SNS) and parasympathetic nervous system (PNS) — work together harmoniously. However, long COVID patients have to deal with an imbalance between the SNS and PNS (in most cases, overactivation of the sympathetic nervous system). This condition can cause symptoms such as abnormal heart rate, heart palpitations, blood pressure changes, fatigue, muscle pain, shortness of breath, and headaches.
Further reading: Yes, COVID causes POTS and dysautonomia
There are many other possibilities. Maybe your symptoms are caused by your immune system turning on you — a phenomenon known as autoimmunity; or maybe leftover viral particles remain in your body after the infection, keeping your immune system permanently on standby. It may be that COVID-19 dealt long-lasting damage to certain organs. Or, some think that the coronavirus awakens viruses that your body has fought before, such as the Epstein-Barr virus (which causes mononucleosis), for example.
All of these possibilities have some evidence to support them, and they’re not mutually exclusive. For some patients, these things could be happening all at the same time. This certainly would explain the sheer number of symptoms associated with long COVID (some symptom lists go over 200). However, this also makes treatment very challenging, making it all the more important to obtain an accurate diagnosis and a long-haul COVID treatment protocol that can be adapted to your specific needs.
With that in mind, here are some of the most prominent treatments offered today.
![oxygen therapy in hyperbaric chamber [V6]](https://www.cognitivefxusa.com/hs-fs/hubfs/oxygen%20therapy%20in%20hyperbaric%20chamber%20%5BV6%5D.jpeg?width=1000&height=559&name=oxygen%20therapy%20in%20hyperbaric%20chamber%20%5BV6%5D.jpeg)
Possibly one of the most widely advertised treatments for long-term COVID-19 is hyperbaric oxygen therapy (HBOT). Briefly, this therapy involves putting patients inside a pressurized environment to breathe 100% pure oxygen. After an infection that causes inflammation, such as COVID-19, different tissues in the body sometimes struggle to receive enough oxygen, which delays the healing process.
During HBOT, patients alternate between pure oxygen and normal air (about 21% oxygen). When the body senses this drop, it interprets it as a lack of oxygen, which triggers the body to seek ways to repair itself. These responses include, for example, growing new blood vessels in the brain and activating the immune system.
A few studies show that HBOT can help long COVID patients, especially by improving memory and attention and reducing pain and fatigue. However, these results are based on limited data, and more research is needed to determine how effective it is and how long its effects last. There are some arguments that HBOT is more effective during acute infection than for long-haul treatment. For this reason, many medical experts — including Cognitive FX — advise caution in using it as a treatment for long-haulers. In addition, it’s not FDA approved for long COVID, and it’s an extremely expensive treatment only available at private facilities.
Another type of treatment hailed to cure long COVID is called repetitive transcranial magnetic stimulation (rTMS). This is a non-invasive method of stimulating specific nerve pathways in the brain to promote certain changes in movement and behavior. RTMS has been found to be effective for a broad range of medical conditions, including movement disorders, such as dystonia and tremors caused by Parkinson’s disease, as well as for psychiatric conditions, such as depression and anxiety.
When it comes to long COVID, studies show that it can help neuropsychiatric symptoms, such as low mood and depression, but it does not improve physical symptoms such as fatigue. Similarly to HBOT, there are limited studies looking at how it can help long-haulers, so caution is advised. Nevertheless, this procedure has been approved by the FDA for treating depression with very positive results. This may help some long COVID patients with neurological and psychological symptoms, but it’s not a complete treatment.
As we’ve seen, long COVID is a complex and challenging condition to treat. As a way to counteract this, doctors are also working on preventative treatments to stop patients from developing long COVID in the first place.
Getting at least one dose of a COVID-19 vaccine not only lowers the risk of developing long-term COVID, but it also reduces the severity of the symptoms in those patients who develop this condition. Researchers don’t fully understand how the vaccine protects against long-term COVID but speculate that it may destroy any remaining viral reservoirs present in the body.
Unvaccinated people may benefit from the vaccine even if they already had the disease previously.
A second option to prevent long COVID was discovered by chance. In late 2021, the FDA approved a combination of nirmatrelvir and ritonavir (Brand name: Paxlovid) as the first antiviral medication to treat acute COVID-19. Very soon, it became clear that patients who had received Paxlovid soon after testing positive for the virus were less likely to develop long COVID. Recently, another study found a second antiviral — molnupiravir (Brand name: Lagevrio) — with a similar protective effect.
Similar to the vaccines, it’s believed these antivirals help eradicate any lingering viruses present in the body after the acute infection. Unfortunately, this protection is only activated if the antiviral is administered within a few days after the patient tests positive, but it has no effects if taken when patients realize they have long-term COVID.
Patients may need to seek treatments to help relieve specific post-COVID-19 symptoms they’re experiencing rather than focusing specifically on the virus. The downside of this approach is the need to visit multiple healthcare professionals, such as:

Taking the previous approach one step further, instead of having patients seek multiple healthcare professionals as needed, it is more supportive for patients to find different disciplines in the same place. Multidisciplinary long COVID rehabilitation clinics — with access to different medical specialties — are in a perfect position to recognize and respond to whatever symptoms patients are experiencing better and quicker than any other care models. Many healthcare providers believe these multidisciplinary clinics should form the backbone of our response to long COVID. Multiple hospitals around the country have now opened post-COVID clinics.
At Cognitive FX, we follow this multidisciplinary approach, but we offer more than just treatment for different symptoms under one roof. Our treatment tackles two common conditions underlying post-COVID syndrome: neurovascular coupling disruption and autonomic nervous system dysfunction.
We know this because we have seen it in our patients. We specialize in post-concussion syndrome (PCS), where patients suffer with long-term symptoms after a mild traumatic brain injury (mTBI) for months or even years. When patients started reporting long-term symptoms after COVID, we realized that PCS patients and long COVID patients had many symptoms in common.
We assessed long COVID patients using a brain imaging scan (see the procedures we follow below) and discovered that these patients were suffering from a similar type of brain dysfunction. We’ve since treated many long COVID patients with very positive results: Some symptoms improve immediately while others take a little longer, but most patients see significant improvements after our intensive treatment and continue to improve at home.
We treat long COVID patients using a combination of physical exercise and multidisciplinary therapies. Our protocol includes:
Before treatment starts, patients undergo a detailed medical examination. During this process, our doctors ask you about your symptoms, medical history, and any other relevant information, such as exams or treatments to address long COVID that you’ve already tried. This assessment also includes a physical exam to check reflex response, balance, and hand-eye coordination; a cognitive evaluation to assess cognitive issues, such as brain fog, poor memory, or difficulty focusing; and a psychological evaluation to detect signs of anxiety, depression, or other mental health problems.

After this initial assessment, patients complete a brain imaging scan to find the areas in the brain most affected by the virus. The scan — called functional NeuroCognitive Imaging (fNCI) — investigates brain function in about 100 regions in the brain and how those regions communicate with each other. During the exam, the patient performs a series of standardized cognitive tasks.
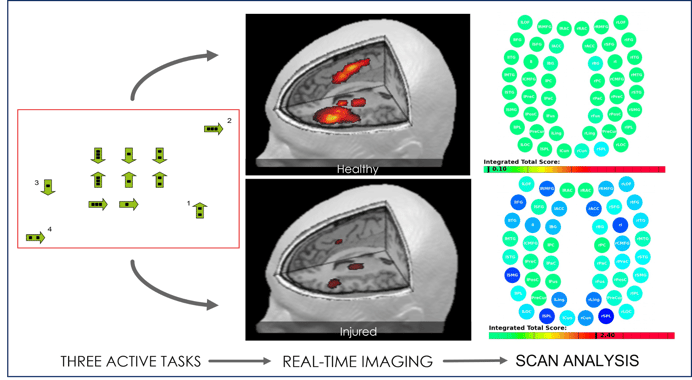
Once these exams are done, our team combines all the information and designs a treatment plan customized for each patient.
From my first day to my last day of my one week treatment at Cognitive FX I felt welcomed and relieved that I was finally getting the help I needed. The team at Cognitive FX runs like a well oiled machine. The communication between team members allows for adjustments to be made to your treatment plan instantaneously. The fMRI scans are only a starting point, the hands-on evaluations further fine tune the treatment to your individual needs. After suffering the effects of long Covid for over a year my balance was greatly improved by the last day of treatment and by the time I settled back into work the following week I noticed my stamina had improved as well. I fully expect continued improvement in the coming weeks and months. This was truly life-changing for me. Thank you!!
— Jennifer Hendrickson (via Google review)
During treatment, our therapists use a combination of physical exercise followed by different therapies. Aerobic exercise, usually on a treadmill or stationary bike, promotes blood flow to the brain and triggers the release of chemicals in the brain, including one called brain-derived neurotrophic factor (BDNF). BDNF improves communication between different areas of the brain, helping the brain become more flexible and able to benefit more from subsequent therapy.
![EPIC Treatment on elliptical [V6]](https://www.cognitivefxusa.com/hs-fs/hubfs/EPIC%20Treatment%20on%20elliptical%20%5BV6%5D.jpg?width=1195&height=783&name=EPIC%20Treatment%20on%20elliptical%20%5BV6%5D.jpg)
Cognitive FX treats long COVID in children as well as adults.
Since cardiovascular exercise can be challenging for some post-COVID patients, our therapists closely monitor heart rate and symptom progression. They will modify the recommended exercise and intensity based on your situation to make sure you obtain the benefits of exercise without burning out too soon.
After exercise, patients engage in a variety of multidisciplinary therapies, including:
While most patients receive all of these therapies during their treatment, the way in which they’re used is personalized for each patient. Each patient is given a unique combination of exercises with emphasis on the skills and brain regions they need assistance with.

Many people experience breathing problems post-COVID (most likely caused by dysfunction of the autonomic nervous system), so an important part of our treatment is to teach these patients a variety of breathing exercises. This is done in combination with extra cardio sessions to encourage the parasympathetic nervous system (PNS) to become better regulated, neutralizing the dominance of the sympathetic nervous system (SNS). These exercises “retrain” the brain and body, allowing both SNS and PNS to work together to respond to what the body needs.
Throughout the treatment, patients also have multiple opportunities to rest so their brains can recover before the subsequent therapies. These periods may include a neuromuscular massage to the neck and shoulders, mindfulness exercises, or sitting in a dark room listening to binaural beats, which encourage relaxation and decrease anxiety.
At the end of treatment, we reassess the patient's physical and cognitive performance and administer a second fNCI. This helps us assess the patient’s progress and guides our recommendations going forward. It’s important to note that treatment at our clinic is only the beginning; recovery must continue at home.
![EPIC Treatment exercise with headphones [V1]](https://www.cognitivefxusa.com/hs-fs/hubfs/EPIC%20Treatment%20exercise%20with%20headphones%20%5BV1%5D.jpg?width=2265&height=1425&name=EPIC%20Treatment%20exercise%20with%20headphones%20%5BV1%5D.jpg)
At the end of his treatment, Cognitive FX patient Boston Sharp shared, “I was really happy because I felt like me again. This is super cliché, but I felt like me. And it was the greatest feeling that I was back.”
You can read more about the Sharp family’s road to post-COVID recovery here.
Each of them had work to do at home, but the fundamental healing they needed to experience had begun to take place.
Supporting our patients after treatment is an important part of our approach. Before leaving us, patients meet with one of our therapists to discuss their results and receive a series of exercises to do at home. This typically includes physical exercises, cognitive activities, visual and vestibular exercises, and relaxation techniques. It usually takes an hour or less five times a week and can be reduced as your symptoms improve. If our therapists feel that the patient may benefit from further therapy, we offer referrals to suitable specialists.
Of the COVID long-haulers who meet our screening criteria, over 90% show improvement after treatment at our clinic. Our long COVID patients report over 40% decrease in symptom severity in 13 symptoms after just one week of multidisciplinary therapy. To discuss your specific long COVID symptoms and whether you’re eligible for treatment at our clinic, schedule a consultation.
In addition to seeking medical assistance to treat your long COVID symptoms, there are many ways to speed up your recovery with simple lifestyle changes, such as engaging in regular exercise or following a healthy diet. Here are a few of our suggestions.

Following a healthy and balanced diet can help your body recover faster.
To help long-haulers, some studies recommend the Mediterranean diet as a way to reduce inflammation, which is believed to be behind many of the symptoms of long COVID. This diet focuses on foods known to reduce inflammation, such as green leafy vegetables, nuts, fatty fish, and fruits such as strawberries and blueberries, while avoiding foods that trigger inflammation, such as fried foods, refined carbohydrates, sugar, red meats, and processed meats.
Be cautious about specific diets you may see advertised online, which can be extremely restrictive and cause nutritional deficiencies. One example is the low histamine diet, which is supposed to control inflammation and reduce COVID symptoms. However, there is no evidence to support these claims, and given the lack of evidence, we think the risks outweigh the potential gain for most patients.
When in doubt, find a licensed and reputable nutritionist or a registered dietician, ideally someone who is already working with long COVID patients, to assist you in your recovery meal planning.
Some patients experience changes in or loss of smell and taste after a COVID infection. Adding strong flavors to your food may help. Some patients find that eating foods with different textures makes meals more interesting. Others prefer to eat cold foods, which may taste better.
Many long-haulers experience digestive issues, including feeling sick, bloating, pain, and diarrhea. Eating plenty of fiber-rich foods, such as fruit, vegetables, nuts, seeds, beans, pulses, and whole grains can help. Probiotics may also be a good option, although there is no hard evidence that these can support long-haulers. If these symptoms persist, speak to your doctor as it’s important to rule out other causes of gastric distress, such as celiac disease.
Vitamin D is vital for the immune system to be fully functional. If you have little or no sunshine exposure due to long COVID, your doctor may advise you to take vitamin D supplements. Some patients with long-term COVID believe high doses of vitamins, such as niacin (vitamin B3), vitamin C, vitamin D, quercetin, and zinc will help with common symptoms. There is no evidence to support these claims, and taking high doses can actually be harmful to you. If you want to take vitamin supplements, read more in our article about natural long-COVID treatments.
Long COVID can drastically reduce your ability to engage in physical activity. This is worse than just deconditioning associated with a period of inactivity, and many patients struggle to begin exercising again and to get back to their pre-COVID levels of fitness. This situation is called post-exertional malaise, and it’s classed as a symptom associated with long COVID.
Nevertheless, going back to regular exercise can help with your long COVID symptoms. It’s important, however, to follow the right approach to avoid triggering symptoms and worsening your condition. You need to structure your exercise plan based on the severity of your symptoms rather than following a standard exercise program that consistently increases in intensity over time. Your progress is not going to be consistent all the time, and sometimes, you may need to reduce the amount of exercise you’re doing and prioritize rest.
In addition, exercise doesn’t have to be something very difficult. Start with whatever you’re capable of, even if it’s just 10 minutes of yoga. You can slowly build up with longer and more demanding regimens. Once you’re further along in your recovery journey, you can try a combination of endurance and strength training. These exercises are ideal to improve muscle strength, which is known to decline during a COVID infection and recovery. Exercise also improves respiratory and cardiovascular fitness, reduces fatigue and shortness of breath, helps with post-acute muscle aches, and boosts quality of life.

Patients with long COVID experience many cognitive symptoms, including deficits in attention, executive functioning, language, processing speed, and memory.
For these patients, engaging in cognitive activities strengthens brain function and reduces cognitive symptoms, but only if the games and activities are challenging. Watching TV is unlikely to provide any benefit, but trying to drive home via a different route can help with memory and decision making, for example. Virtually any mental activity can help, and the more senses you try to incorporate into your games, the better.
A few examples include:
See our post on cognitive exercises for PCS for more ideas; they work just as well for long COVID patients.
Further reading: What to do about post-COVID brain fog
Due to the nature of the condition, patients with long-term COVID are at a high risk of social isolation. Symptoms such as fatigue, headaches, and brain fog are not very conducive to engaging in social activities, and many patients tend to just stay at home.
Being socially active can help patients recover faster, but it needs to be done in the right way:
One of the most common long COVID symptoms involves sleep disturbances. This often leads to fatigue and headaches, as well as low mood or even depression due to lack of sleep.
Getting enough sleep is crucial to your recovery. Various strategies can support better sleep, including:
If all of these suggestions don’t really help you sleep, see a doctor to review symptoms and gain a fuller understanding of what is causing poor sleep.
Further reading: What to do about post-COVID insomnia

If you’re recovering from long COVID, you need to include frequent breaks when you plan your daily activities. Ignoring your symptoms and trying to “tough it out” will just make things worse.
If you’re not sure when you need a break, follow the rule of three. If you’ve noticed that three symptoms have started or are worsening, then you need a break. For example, if you’re feeling a little anxious and dizzy and you have a headache, find a quiet space for a break.
If you’re experiencing a single symptom, but it’s deteriorating quickly, it’s a sign that you need a rest. For example, if your headache started off as mild (level 1), but it’s jumped three levels, and it’s now severe (level 4), you need to get away from what you’re doing.
It’s important to note that you don’t have to take a break every time you experience symptoms. If you’re just feeling slightly nauseous, or you’re feeling a little “foggy,” it’s OK to continue your activity. In fact, this helps the brain heal and can help reduce other symptoms in the future.
If you work for long hours on the computer, the 20-20-20 rule may be helpful. The rule is easy to follow: Every 20 minutes, look at something that is 20 feet away for 20 seconds. You don’t need to be exact with the distance; the aim is to shift your focus from the computer (closed) to what’s outside (far away). You can just look out a window or go for a quick walk outdoors.
Even as you recover and start to manage working without triggering symptoms, it’s still advisable to take regular breaks. Simply set hourly reminders on your phone to know when it’s time for a break. When your phone beeps, stop what you’re doing and take a break.
These breaks don’t necessarily mean doing nothing (though they can). You just need to give your brain a rest from what you were doing and do something else. For example, you can:
Of the COVID long-haulers who meet our screening criteria, over 90% show improvement after treatment at our clinic. Our long COVID patients report over 40% decrease in symptom severity in 13 symptoms after just one week of multidisciplinary therapy. To discuss your specific long COVID symptoms and whether you’re eligible for treatment at our clinic, schedule a consultation.
Many long-haulers complain of fatigue during the day. If that’s the case for you, the best way to cope with this symptom is to pace yourself. In practical terms, this means working out what activities you can manage without overexerting yourself and gradually building up your activity level from there. This is a tried-and-tested formula: A study involving more than 3,700 long-haulers found that pacing was very helpful for symptom management.
Here are some simple tips for pacing yourself and managing fatigue as you recover:
Further reading: What to do about post-COVID fatigue
Long COVID symptoms can be unpredictable. Patients often struggle to go back to work, complete daily tasks, or even go out with friends for social events. It’s not surprising that the long-term effects of COVID-19 can hurt not just physical health, but emotional health too, and that it lowers patients’ quality of life.
Typical signs and symptoms can include:
If you’re experiencing any of these, there are things you can do to manage your symptoms:
Look after yourself: Simple lifestyle changes can have a big effect on your mental health, including eating a balanced diet, engaging in regular exercise, and getting enough sleep.
Keep an active social life: Reach out to family and friends, and arrange to meet them in person or at least speak with them on the phone.
Take part in meaningful activities: When you feel low, you may not want to do your usual activities. Don’t give up on everything. Choose small activities you can complete that will give you a sense of enjoyment and accomplishment.

Especially if you have respiratory problems caused by COVID, breathing exercises can help relieve symptoms. Deep breathing exercises can help restore diaphragm function and increase lung capacity. These exercises also help fight feelings of anxiety and stress and promote sleep.
There are many different types of breathing exercises, but these two may be particularly helpful for patients with long COVID:
Further reading: Post-COVID shortness of breath
If you smoke (or vape), one way to reduce the severity of your symptoms during long COVID is by quitting. Several studies have shown that smoking increases the risk of developing long COVID and aggravates respiratory symptoms. This is not surprising given that smoking causes a wide variety of health problems, including lung disease, cardiovascular problems, and a poor immune system.
The good news is that once you decide to quit, the benefits for your body are almost immediate. You will notice how your lung function improves and associated health conditions become less severe.
It may appear counterintuitive, but one way to speed up your recovery from long COVID is to return to work (or school), even before all your symptoms have subsided.
A good time to return to work could be when:
If you have been off work due to long COVID and feel that you’re ready to go back to work, the first step is to meet with your employer. At this meeting, you can explain your current symptoms and what you still find hard to do. You may also want to discuss a phased return or a lighter workload as you slowly build back up to what you used to do. Coordinate with your healthcare professional as well; they can help you determine what’s realistic and make a plan for what to do if your symptoms are too oppressive.
Possible adjustments include:

Finally, recovery takes time. It’s not a linear process. You might have a good day or even three good days, but that’s no guarantee that you won’t then have a hard day and need a little extra give in your schedule to recuperate. This doesn’t mean you’re not improving over time.
That said, if you’re having more bad days than good days, you may be overexerting yourself. Rethink how much you can do each day.
Also, remember that long COVID can happen to those whose initial illness was entirely mild, not just to those who suffered severe COVID-19 needing intensive care and constant monitoring of their flagging oxygen levels. Post-COVID conditions can develop in anyone. If you feel alone in your journey to return to normal daily life, look for local and online support groups.
Want the support of a seasoned, multidisciplinary long COVID treatment team? Schedule a consultation to see if we can help.

Dr. Mark D. Allen holds a Ph.D. in Cognitive Science from Johns Hopkins University and received post-doctoral training in Cognitive Neuroscience and Functional Neuroimaging at the University of Washington. As a co-founder of Cognitive Fx, he played a pivotal role in establishing the unique and exceptional treatment approach. Dr. Allen is renowned for his pioneering work in adapting fMRI for clinical use. His contributions encompass neuroimaging biomarkers development for post-concussion diagnosis and innovative research into the pathophysiology of chronic post-concussion symptoms. He's conducted over 10,000 individualized fMRI patient assessments and crafted a high-intensity interval training program for neuronal and cerebrovascular recovery. Dr. Allen has also co-engineered a machine learning-based neuroanatomical discovery tool and advanced fMRI analysis techniques, ensuring more reliable analysis for concussion patients.

You lie awake at 2 a.m., exhausted but unable to sleep. When sleep finally comes, strange dreams jolt you awake. Morning arrives and you feel like you never rested at all.

If you're reading this, you've probably tried everything for the headaches that won't quit since your COVID infection. Maybe it's been three months. Maybe it's been two years. You've likely cycled...

It’s not uncommon for people in today’s society to be tired. The demands on our time seem to be never ending. However, there’s a difference between being tired from being on the go all of the time...

Most patients with COVID-19 recover within a few days or weeks after a brief acute infection. However,about 10%experience long-term symptoms such as brain fog, fatigue, headaches, shortness of...

Headaches are one of the most common symptoms after a head injury (studies show70%of mTBI patients experience them, though 84% of our patients report having them). They can develop after mild,...
“Eat right and exercise” – this advice is nothing new, you’re tired of hearing it and you’re tempted to tune it out right now – but it’s not going away. In fact, when it comes to brain health, this...
Published peer-reviewed research shows that Cognitive FX treatment leads to meaningful symptom reduction in post-concussion symptoms for 77% of study participants. Cognitive FX is the only PCS clinic with third-party validated treatment outcomes.
READ FULL STUDY