If you’re wondering what to do when transcranial magnetic stimulation (TMS) doesn’t work, you might be:
- In the middle of treatment, and not seeing the results you hoped for.
- Considering TMS and researching potential outcomes.
- Someone who completed treatment but hasn’t experienced meaningful improvements.
No matter where you are in the process, it can be disheartening to face uncertainty—especially if you’ve already tried multiple medications or therapies with little relief.
When TMS doesn’t deliver the expected benefits, it’s easy to feel discouraged or even hopeless. But you’re not alone—and you’re not out of options.
In this article, we discuss:
Why TMS Therapy Might Not Be Working
TMS can be a life-changing treatment for many people, but it’s not effective for everyone. Here are some potential reasons why TMS may not be producing the desired results:
1. Misdiagnosis
TMS is FDA-approved for major depressive disorder (MDD) and treatment-resistant depression (TRD). If a patient is misdiagnosed—for example, they have bipolar disorder or schizophrenia—TMS may be ineffective or even worsen depression symptoms. A comprehensive psychological evaluation is essential before starting TMS treatment.
2. Inaccurate Coil Placement
One of the most common technical reasons for poor outcomes is inaccurate placement of the magnetic coil. TMS works by stimulating a specific area of the brain known as the dorsolateral prefrontal cortex (DLPFC). The DLPFC as a whole isn’t hard to locate, but pinpointing the specific spot within the DLPFC that makes treatment work can be difficult.
The widely used “5 cm method” estimates coil placement based on external landmarks, which often fails to account for individual variations in head size, shape, and brain structure. As a result, the coil may stimulate the wrong part of the brain—leading to poor outcomes or even symptom worsening.
3. The TMS Dip
Roughly 20–25% of TMS patients experience a temporary worsening of symptoms during the first few sessions—a phenomenon known as the “TMS dip.”
This is a normal part of brain reorganization and often indicates that the brain is responding to treatment. Many patients who experience this go on to see meaningful improvements.
4. Mistaking Side Effects for Lack of Effectiveness
Common side effects like headaches, dizziness, or facial discomfort may be mistaken as signs the treatment isn’t working. These side effects are typically mild and temporary.
Severe side effects, such as seizures, are extremely rare (less than 1 in 10,000 sessions). TMS can trigger mania in patients with bipolar disorder, which is why proper screening is essential.
Further reading: Is TMS safe?
5. Missed Sessions
Missing occasional sessions is usually not a concern, but frequent or consecutive missed sessions—especially during the early stages—can reduce the effectiveness of treatment.
6. Severe Depression or Comorbid Conditions
TMS may take longer to work for patients with severe depression or co-occurring mental health conditions such as anxiety, PTSD, obsessive-compulsive disorder (OCD), or bipolar disorder. In these cases, combining TMS with other treatments (e.g., antidepressant medications or psychotherapy) may enhance outcomes.
7. High Expectations
If you expect dramatic improvements within days, slower progress can feel like failure. In reality, changes are often gradual. Some patients don’t notice significant improvements until weeks after completing the full course of treatment.
For example, one of our patients worried that her treatment may not have worked in the first few weeks after treatment. But then something shifted.
“I suddenly realized I hadn’t felt that cloud in days. Smiling was easier. Laughing was easier. It just crept up on me—and then it felt like the sun just broke through. I went five months without a single depressive crash. That was monumental for me.”
Read Sarah’s success story here.
What to Do If TMS Isn’t Working
1. Talk to Your Healthcare Provider
Your provider can reassess your diagnosis, treatment history, and coil placement technique. This review may reveal adjustments or alternative approaches that could improve outcomes.
2. Complete the Full Treatment
In general, sticking with your treatment plan will give you the best chance at responding to TMS. Everyone responds at a different pace. While some feel better after a few TMS sessions, others see changes only after completing the full 4–6 week course—or even several weeks later.
Exception: If TMS causes extreme anxiety, distress, or challenging side effects, your provider may recommend pausing or stopping treatment.
3. Optimize Your TMS Protocol
Ask your provider about adjusting stimulation intensity, coil angle, or target location. These changes can increase the comfort and effectiveness of TMS.
4. Consider Maintenance Sessions
If your symptoms begin to return some time after completing TMS, maintenance sessions (weekly, bi-weekly, or monthly) can help sustain progress.
5. Combine TMS with Other Treatments or Lifestyle Changes
-
Medication: Combining TMS with antidepressant medication may improve outcomes, though certain medications (e.g., tricyclics, some antipsychotics) may be contraindicated.
-
Psychotherapy: Talk therapy—especially cognitive behavioral therapy (CBT)—can enhance TMS effectiveness by reinforcing behavioral and cognitive changes. Studies suggest that combining TMS and CBT may be more effective than either treatment alone, particularly for patients with treatment-resistant depression. We follow this approach at Cognitive FX, and we’ll explain more below.
-
Lifestyle changes: Exercise, diet, sleep hygiene, and stress management all support brain health and can improve how your body responds to TMS.
When Standard TMS Doesn’t Work: Consider Trying a Different Protocol
Typically, only about 50% of patients respond to conventional TMS (rTMS), and just over 30% achieve remission.
If you tried rTMS without success, it may be worth exploring a more advanced protocol.
The SAINT™ TMS Protocol
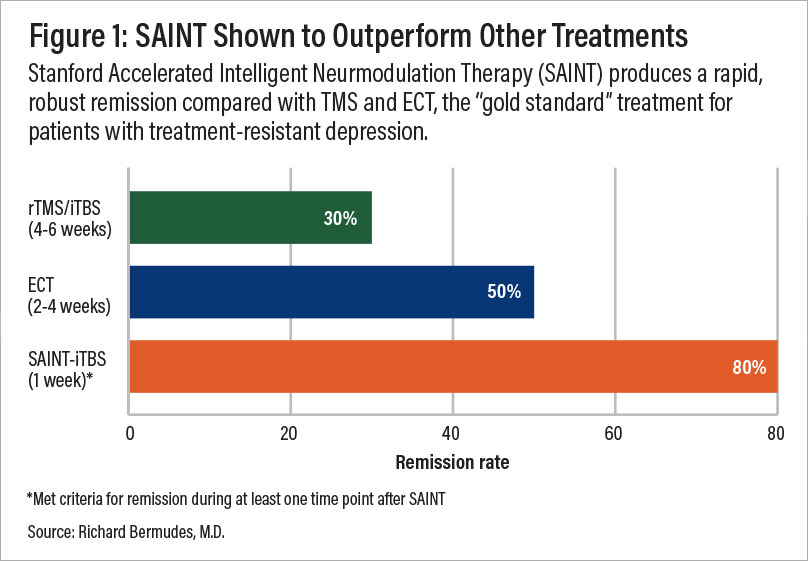
SAINT™ (Stanford Accelerated Intelligent Neuromodulation Therapy) uses intermittent theta-burst stimulation (iTBS), a more advanced brain stimulation that mimics natural brain wave rhythms, combined with fMRI-guided coil placement for precise targeting.
This ensures magnetic pulses hit the exact brain target, tailored to each patient’s head size, shape, and brain structure.
It delivers 10 sessions per day for five days—50 sessions total—compressing the typical 4- to 6-week treatment course into one week.
Clinical trials have yielded some of the highest depression treatment success rates to date:
- Response rate: ~86%
- Remission rate: ~79%
- One-month remission durability: ~60%
- Repeatability: 90% of patients who relapsed achieved remission again with a second round
While highly effective, SAINT™ costs roughly $30,000 and isn’t yet covered by most insurance providers.
A More Affordable Alternative to SAINT™ at Cognitive FX
At Cognitive FX, we offer a similar accelerated TMS protocol combining fMRI-guided targeting with theta burst stimulation—at a fraction of the cost ($9,000–$12,000).
Our team uses advanced fMRI post-processing to pinpoint each patient’s ideal DLPFC target based on functional brain patterns. You receive the same precision as SAINT™—but at a significantly lower cost.
We also include cognitive behavioral therapy during treatment, which can boost remission rates by up to 19% and support longer-term benefits.
Note: We do not treat patients under 18 or over 65, those with a history of seizures, or patients in immediate crisis.
To see if you’re a good fit for our accelerated fMRI-TMS treatment, take our good fit quiz. You can learn more about our approach here.
If TMS Still Doesn’t Work: Consider Other Options
Electroconvulsive Therapy (ECT)
- Pros: Fast-acting and effective (~80% response rate)
- Cons: More invasive; cognitive side effects (e.g., memory loss)
Further reading: ECT vs. TMS: side effects, effectiveness & cost
Vagus Nerve Stimulation (VNS)
- Pros: Implantable device provides ongoing stimulation; studies show over 80% of patients improve over time.
- Cons: Requires surgery; slower onset.
Further reading: Vagus nerve stimulation
Ketamine
- Pros: Fast-acting relief for many; can work when other treatments fail.
- Cons: Short-lived effects; lower remission rates over time.
Further reading: Ketamine vs. TMS
Healthy Habits to Support Your Treatment
Lifestyle changes can reinforce the benefits of TMS or other therapies:
- Exercise: Regular activity improves mood and brain health.
- Nutrition: Eat a balanced, low-sugar, anti-inflammatory diet.
- Sleep: Maintain a consistent sleep schedule and bedtime routine.
- Stress Management: Practice mindfulness, meditation, or breathing techniques.
- Social Support: Stay connected with friends, family, or support groups.
TMS Isn’t Always the End of the Road
If TMS hasn’t worked for you, there are still paths forward. Whether it’s completing your current treatment, adjusting your protocol, trying a more advanced method like accelerated fMRI-TMS, or exploring alternative therapies, there is hope.
At Cognitive FX, we’re committed to providing precision-guided, effective care for patients with treatment-resistant depression—without the price tag of proprietary protocols.
To see if you’re a good fit for our accelerated fMRI-TMS treatment, take our good fit quiz. You can learn more about our approach here.
Cited research