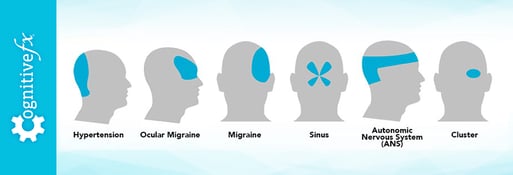
Many people have neck pain after a concussion or whiplash injury. It may show up immediately after your injury or weeks to months afterward. That pain may involve stiffness, tension, sharp pain, and pain associated with certain movements or behaviors (e.g., looking at your phone). The pain may feel deep or superficial.
There are many possible causes of neck pain after concussion and whiplash. If you’ve only been diagnosed with whiplash, realize that the force necessary to cause the whiplash is typically enough to cause a mild traumatic brain injury (mTBI, commonly called concussion).
And if you’ve hit your head, there’s a chance your neck was also affected. Many patients struggle with symptoms from both, which is why diagnosing the cause of your neck pain and treating it (along with any other symptoms from your injury) is a complex process.
If it’s been less than two weeks since your injury, there’s a chance your neck pain and other common symptoms will go away on their own. But if you’re still struggling with neck pain and other concussion symptoms three months after your injury, you likely have post-concussion syndrome (PCS).
Persistent post-concussion symptoms typically do not resolve on their own. At our post concussion clinic, Cognitive FX, we treat hundreds of patients every year who suffer from persistent concussion symptoms. Many of them complain of neck pain. Our job is to determine what’s causing that pain and then include therapies that will help them feel better in their treatment plan.
In this post, we’ll explain some of the many reasons you may be suffering from neck pain after a concussion or whiplash, along with what you can do about it:
If you have lingering symptoms from a concussion, you’re not alone. As many as 30% of concussion patients do not recover without treatment. 95% of our patients experience statistically verified restoration of brain function after natural therapy at our clinic. To learn if you’re eligible for the program, schedule a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
What Causes Neck Pain after a Concussion?
There are many post-concussion issues that can cause neck pain after a concussion. It could be a physical injury, or something more difficult to determine. For example, dysfunction in your vestibular system — the system that determines your orientation in space and helps you keep your balance — could also affect your neck health.
Here’s a list of the most common causes of neck pain after concussion and whiplash:
Potential Causes of Neck Pain after Concussion and Whiplash
|
Cause
|
Background
|
Most Likely Treatment(s)
|
|
Physical neck injury
|
Trauma to soft tissues or bones in the neck.
|
Physical therapy, massage, and, for more serious injuries, surgery.
|
|
Autonomic nervous system dysfunction
|
An imbalance between the sympathetic and parasympathetic nervous system that can cause neck tension, inflammation, blood pressure dysregulation, and more.
|
Neuromuscular therapy, neurointegrative therapy, psychotherapy, and more.
|
|
Vision and vestibular problems
|
Injury-induced vision and vestibular changes that put stress on muscles in the neck.
|
Vision therapy, vestibular therapy, neuromuscular therapy, massage, and more.
|
|
Altered pain perception
|
Dysfunctional neurovascular coupling in areas of the brain responsible for sensory processing, pain perception, and more.
|
EPIC Treatment (restoration of healthy neurovascular coupling).
|
|
Compensatory behaviors
|
Poor posture or repeated, unnatural head movements due to other concussion symptoms resulting in changes to neck musculature and structure.
|
EPIC Treatment to resolve other concussion symptoms, followed by additional physical therapy to improve functioning of neck muscles.
|
|
Spinal alignment
|
Misalignment of vertebrae in cervical spine (scientists are split on whether this causes symptoms).
|
Spinal adjustment from a reputable chiropractor.
|
While just one of these conditions might be causing your neck pain, most patients have several issues contributing to their discomfort. For therapy to be successful, it has to address most of the contributing factors — or, at the very least, the most serious ones.
Here’s some more information about how each of these issues causes neck pain after a concussive event.
A Physical Problem with the Neck
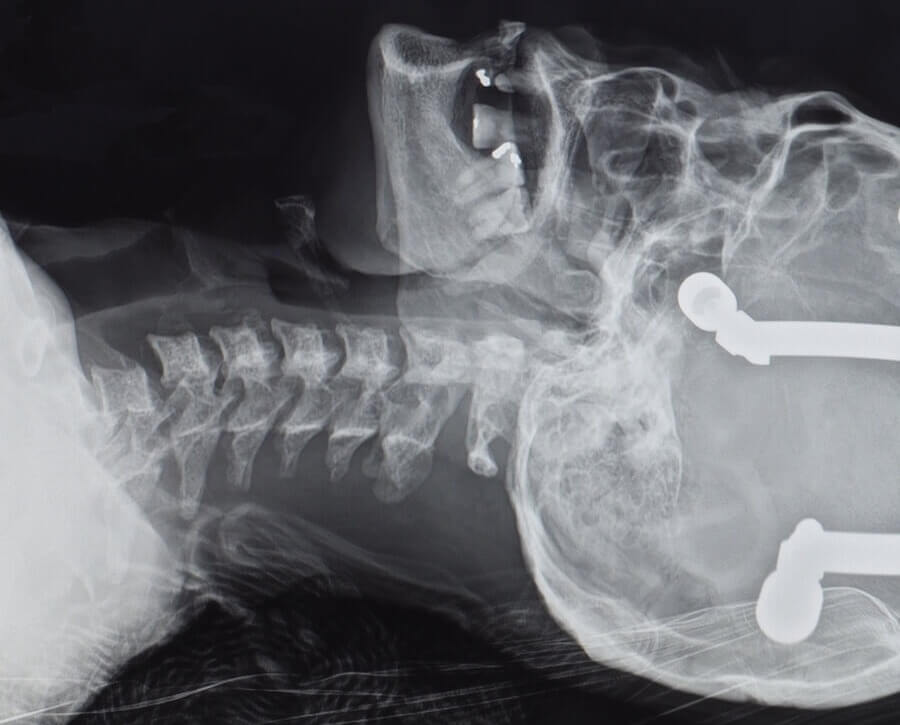
You might have any one of several neck injuries with traumatic brain injury: a bulging disc, cervical strain, ligament damage, herniated disk... the list goes on. These injuries are most likely with severe TBI but can occur with whiplash and concussion as well.
If you had an existing degenerative disorder — such as scoliosis — then a head injury could worsen it. TBI can exacerbate structure issues in your neck by putting more strain on the disks and vertebrae, leading to faster degeneration or even new or increased disk bulging or herniation.
If there’s any reason to suspect physical injury to the neck, you should visit a healthcare provider and consider diagnostic imaging.
What Are Warning Signs of Physical Neck Damage?
Here are four signs that your neck pain might stem from a physical injury:
- Sharp pain that is present all the time or occurs with certain movements.
- Worsening of neck pain and related symptoms over time.
- Difficulty turning the neck.
- Weakness in the legs, arms, hands, or fingers.
If you and your doctor suspect a physical injury but can’t confirm it with a physical exam, you may need diagnostic imaging. Many health care professionals will start with an X-ray; this can only show bone structure and will more often rule out any issues than diagnose them. A CT scan might not have enough detail to diagnose your injury.
An MRI of the cervical spine, on the other hand, will show soft structures (such as the cervical discs and whether they’re being squeezed) and bone. If you want just one scan, the MRI will most likely provide enough information for your doctor to make a diagnosis and recommend treatment. You can read more about the three main types of imaging and what they show here.
Autonomic Nervous System Dysfunction (Dysautonomia)
The autonomic nervous system regulates a host of involuntary processes throughout your body. Some examples include your heart rate, blood flow, breathing, digestion, and physiological threat response.
The ANS has two halves: the sympathetic nervous system (SNS, the “fight or flight” system) and parasympathetic nervous system (PNS, the “rest and digest” system). In a healthy person, one side of the system isn’t dominant over the other. They’re in a constant state of flux, deftly responding to the needs of your body at each moment.
But after a head or neck injury, the ANS may become less flexible and “stuck” in a state of sympathetic nervous system activation. And that can easily lead to neck pain.
Imagine you’re a cat. Something startles you, so you arch your back at it and hiss. But then, instead of returning to normal, you stay arched for days afterward. Being in that tense state all the time would really start to hurt!
That’s a bit what it’s like for many post-concussion patients who suffer from anxiety and autonomic nervous system issues after their injury. Like a cat arching its back, the ANS is clenching the muscles that connect the neck and shoulders (and sometimes the jaw as well) because it feels threatened.
Many patients who suffer from dysautonomia report neck muscles that just won’t relax no matter what they try. Being in that state all the time will result in tension, pain, and stiffness. They might also have cervicogenic headaches. If you suffer from post-concussion headaches, read this post.
In addition, patients with nervous system issues may also experience an overactive immune system. It may cause inflammation throughout the body, including the neck. In fact, the neck is extra susceptible to inflammation after a head injury because it is a key pathway for signals traveling to and from your brain.
Plus, the neck acts like a central train station for the ANS: All of the key connections between the autonomic nervous system, brain, and other organs meet in the neck! When something goes awry with the nervous system, you very well may suffer from inflammation in the neck, resulting in a sore, painful neck.
If you have persistent symptoms from a concussion, schedule a consultation with our team of experts.
Vision and Vestibular Issues
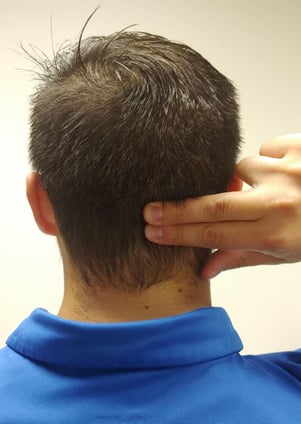
Place two fingers on the back of your upper neck (as shown in the image). Without turning your head, look as far left as you can, then as far right as you can. You should feel the muscles in your neck activate, even though you haven’t moved your head at all!
Every time your eyes move, your cervical muscles engage. If something is wrong with your vision, there’s a very good chance it will create extra work for your neck as it attempts to compensate. How that plays out depends on what type of vision problems you have and what your body tries to do to make up for them.
For example, one of our patients was so affected by gaze instability that, rather than turn her head to look at something, she would turn her entire body!
Several other patients have had cervical instability — neck muscles that were too loose and couldn’t keep their heads sufficiently supported. That resulted in not only neck pain, but an overwhelmed vestibulo-ocular system, which presented as nausea, cervicogenic dizziness and vertigo, headaches, balance problems, and more.
The neck, your vision, and your vestibular system all work closely together; when even just one out of the three isn’t functioning correctly, all three can be affected.
Pain Processing
Sensory signals from throughout your body travel through the nerves in your neck to the brain. If there’s any pressure on those nerves (say, from a disk that’s slightly out of place, or from inflammation), you may experience phantom pain signals or pain signals that are stronger than they normally would be.
Once those signals reach the brain, they are processed in the thalamus — the part of the brain that all sensory information passes through. Many patients have dysfunction in their thalamus. This is because the inflammation from head trauma puts more pressure on the deeper parts of the brain, which increases the chance they’ll be injured long-term. If that happens, the thalamus itself may not process sensory information the right way, resulting in more pain, feelings of overwhelm, poor hand-eye coordination, and more.
Compensatory Behaviors

Some people suffer from post-concussion syndrome for years before discovering our clinic. If you’ve been craning your neck at weird angles for 10 years trying to compensate for vision issues, for example, that can alter the structure of your cervical spine. Some of our patients have a straight neck (it’s supposed to be curved) because the muscles around it are so tight from years of bad habits.
We suspect that light sensitivity and vision problems are the most common culprits. Fortunately, the majority of postural issues aren’t permanent. They can be resolved with appropriate physical therapy and treatment of the underlying concussion-related problems that caused the postural issues in the first place.
Spinal Alignment
Some of our patients report relief (in full or in part) after visiting a reputable chiropractor. Chiropractors believe that small misalignment issues in the upper cervical spine may cause pressure and pain that can be relieved through spinal adjustments.
We’ll stay out of the debate on whether it makes a difference, and leave you with this: If you’ve tried other treatments unsuccessfully, consider visiting a chiropractor for help. Just make sure they have great reviews for their practice, and make them aware of your brain injury. If there’s any suspicion that you could have a physical neck injury, make sure you determine what that is first because a chiropractic adjustment could make certain injuries worse.
Diagnosis and Treatment for Post-Concussion Neck Pain
A physician you see for chronic neck pain after a concussion might refer you to physical therapy and order some imaging. While physical therapy may help, it is likely not enough to resolve your neck problems since there are so many factors that influence neck pain.
Many doctors will also prescribe pharmaceutical solutions such as muscle relaxants and pain medicine. Be very careful with the use of pain medications (even over-the-counter options such as ibuprofen). These medications can’t solve an underlying problem, but over time, they do put stress on your liver and could propagate more issues. Muscle relaxants are especially problematic — if your symptoms come from cervical instability, then taking a relaxant will actually make that problem worse.
So what can you do? Get evaluated by an expert in post-concussion syndrome. While some concussion clinics or sports medicine doctors can do this, few can provide a holistic approach to treating post-concussion syndrome. Many patients go from doctor to doctor for years before finding the right one.
So what should you look for in a provider when you have PCS and neck pain? A good evaluation of neck pain and related symptoms should include:
- Studying the patient’s gait, posture, balance, vision, and inner ear.
- Testing the nervous system in various ways.
- A cervical neck scan to identify any structural problems.
- Removing the need for compensatory behavior (by resolving those symptoms) and seeing what happens.
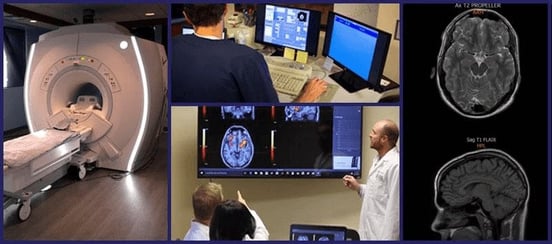
At Cognitive FX, we evaluate all of these aspects of post-injury health, including a standard MRI of the cervical spine to make sure there are no serious physical problems that could be causing the pain. Finally, we do a functional neurocognitive imaging scan (fNCI) on every patient.
The fNCI shows us which regions of your brain were impacted by your injury and in what way. Post-concussion syndrome stems from a dysfunction in communication between neurons and the blood vessels that supply them with the oxygen and other nutrients they need to function well (a relationship known as neurovascular coupling, or NVC).
Brain functions that used to be easy suddenly become harder with dysregulated NVC. Your brain will have some regions that are hypoactive (not doing as much as they should) and some that are hyperactive (either because they’re compensating for the underperforming brain regions or because they’re pulling more and more resources to do simple tasks).
That dysfunction drives many of the other post-concussion symptoms you face. It’s often tied into the ANS, vision, and vestibular dysfunction we mentioned earlier. Identifying those injured brain regions with an fNCI gives us the information we need to deliver treatment tailored to each person’s injury.
Remember that the neck isn’t an isolated part of the anatomy. Many of the problems in your neck are likely caused by interrelated concussion symptoms. To treat the neck effectively, you need to treat the post-concussion syndrome itself.
What Treatment at Cognitive FX Is Like
After an extensive evaluation — including physical testing, fNCI, and a structural MRI of the brain and neck — your care team will put together a plan for your treatment period at the clinic. Treatment for post-concussion syndrome typically includes:
We also incorporate breathing exercises, relaxation techniques, and mindfulness. Each patient meets with our psychologist to help with the emotional aspects of therapy and recovery.

It’s this unique combination of multidisciplinary therapies combined with physical activity that makes EPIC treatment work. Aerobic exercise naturally provides extra oxygen to the brain, allowing it to benefit from what’s called the Post Exercise Cognitive Boost (PECB).
During PECB, essential neurotransmitters (such as BDNF) and proteins that help promote blood flow are released in the brain. This helps your brain perform cognitive tasks for longer periods of time.
These therapies challenge your brain, pushing it to abandon the inefficient pathways formed after injury and teaching it to revert to healthy neurovascular coupling. They also teach the autonomic nervous system how to better communicate with your brain and body. Once that happens, patients typically see a dramatic improvement in their symptoms.
After treatment, you’ll receive another fNCI scan to confirm the progress your brain has made. We’ll meet with you to discuss what to do at home to continue improving.
What You Can Do at Home

Nothing you do at home can replace getting the right therapy for post-concussion syndrome, but it can strengthen and improve the results you get from treatment.
After treatment at Cognitive FX, we may refer you to several specialists to help you continue recovering:
- If your neck pain is related to emotional stress, we will refer you to a cognitive-behavioral therapist.
- If you need to rebuild or correct neck musculature after years of compensatory behaviors, we’ll refer you to a physical therapist.
- If you have vision problems, we’ll have you work with a vision therapist since vision problems cannot typically be corrected in just one week and will take continued work to resolve).
If needed, we also offer follow-up, remote vestibular and vision therapy appointments when we can’t find a suitable provider near your residence.
Here are a few things you can do by yourself, with or without treatment:
- Work on your sleep posture. Many people don’t have an appropriate pillow size for their neck. A good pillow will keep your neck straight as you sleep. If your head is tilted up or down, then the pillow probably isn’t the right size. If you have pets, we recommend they stay out of the bedroom, as co-sleeping with animals can lead to some unhealthy sleep positions. Read this post if you suffer from sleep disturbances.
- Get more exercise! Exercise keeps the sympathetic nervous system in check and strengthens the connection between your brain and the rest of your body. Every time you exercise is like a system refresh. In addition, exercise will promote better blood flow and help fight inflammation. In turn, that will help you feel better and relieve some of the pain in your neck. Read this post if you struggle with post-concussion exercise.
- Stay fully hydrated and get proper post-concussion nutrition. Staying well hydrated will keep the discs in your neck healthy and full. Plus, good nutrition is a key component in post-concussion recovery. Read this post to learn more about nutrition after a brain injury.
- Stretch and massage your neck. You can give these neck stretches a try. And in our video below, we explain how to massage your own neck to relieve some pain and tension:
- Neck pain and tension often lead to headaches. If you experience recurring headaches, then this course is for you. It covers which types of headaches you can get after a concussion, as well as specific techniques for coping with those types of headaches. At the end of the course, you'll know how to manage your headaches at home.

Neck pain is stubborn. While many post-concussion symptoms resolve during or shortly after treatment, neck pain may take weeks to months to resolve fully. As long as you consistently work at your therapy and try to correct any conditions at home that might make your neck pain worse, you should continue to improve.
If you have lingering symptoms from a concussion, you’re not alone. As many as 30% of concussion patients do not recover without treatment. 95% of our patients experience statistically verified restoration of brain function after natural therapy at our clinic. To learn if you’re eligible for the program, schedule a consultation.