If you have post-concussion syndrome (PCS), then you likely know how difficult it is to get an accurate diagnosis and comprehensive treatment. Many medical doctors don’t have the resources to treat PCS effectively, or they rely exclusively on pharmaceuticals that help some symptoms while making others worse. So when you find a healthcare provider who (a) actually knows what post-concussion syndrome is, and (b) claims to treat it, then it’s worth following up.
In your search for good treatment, you may have come across chiropractic care as a possible solution. Some patients report relief from some or all of their symptoms after chiropractic adjustments.
So, should you see a chiropractor for post-concussion syndrome? That depends. Few chiropractors have the requisite knowledge to help post-concussion syndrome patients, but some can and do help patients suffering from symptoms after a concussion.
Because post-concussion syndrome is so complex, a chiropractor might or might not be able to help you specifically. It all depends on what’s causing your symptoms and whether that is something a chiropractor can fix. And if you would benefit from an adjustment, finding a chiropractor with the right skill set may take time.
At Cognitive FX, we treat hundreds of patients for post-concussion syndrome every year. 95% of them experience statistically verified restoration of brain function after the end of the week. Sometimes our treatment program is all that patients need, but other times we refer them to specialists (including, when appropriate, chiropractors) to continue working on specific areas, like vision, hormones, vestibular function, mental health, or neck pain.
We’re familiar with the ways that a chiropractor can and can’t help our patients. So, to help you determine whether you should see a chiropractor for your PCS, we explain the following in this post:
If you’re experiencing symptoms that won’t go away after a concussion, we can help. On average, our patients show up to 75% improvement after one week of treatment. To learn about diagnosis and treatment options, sign up for a consultation.
Note: Any data relating to brain function mentioned in this post is from our first generation fNCI scans. Gen 1 scans compared activation in various regions of the brain with a control database of healthy brains. Our clinic is now rolling out second-generation fNCI which looks both at the activation of individual brain regions and at the connections between brain regions. Results are interpreted and reported differently for Gen 2 than for Gen 1; reports will not look the same if you come into the clinic for treatment.
What Causes Post-Concussion Syndrome Symptoms?
PCS symptoms stem from brain trauma. That trauma can come from an external force (mild traumatic brain injury, or mTBI), whiplash, or an internal cause. Internal causes could include infections such as meningitis and COVID-19, events like TIA or stroke, carbon monoxide poisoning, or exposure to chemicals such as chemotherapy drugs.
What all these causes have in common is that they can interfere with communication pathways in the brain (dysfunctional neurovascular coupling, which we explain below). Depending on the injury, you might also struggle with dysautonomia, hormone problems, neck problems, and issues with your vision and vestibular systems. All of these issues can cause PCS symptoms. They are usually interrelated, which means it’s hard to resolve symptoms without resolving all of those causes at the same time. Here’s a closer look at each of those causes.
Dysfunctional Neurovascular Coupling
A concussion causes inflammation and microstructural damage in the brain. This damage can interfere with neurovascular coupling, the relationship between neurons and the blood vessels that supply them with the right amount of oxygen at the right time to do their jobs.
When a concussive force disrupts healthy neurovascular coupling (NVC), the affected brain regions may not work properly. They might be hypoactive (unable to do everything they normally should) or hyperactive (doing too much or taking up too many resources). In post-concussion syndrome, those affected communication pathways don’t revert to normal after the brain heals from the concussion.
Think of it as a big thunderstorm in your brain. Heavy rains cause areas of damage to bridges and roads, making them impassable for a time. After the storm, the waters recede, but not all the roads are usable.

For patients who experience persistent symptoms, it’s like the repair crews never show up. Those damaged roads — analogous to your brain’s pathways for passing nutrients and information to the right places — will stay dysfunctional until they’re repaired.
Repairing dysfunctional neurovascular coupling is key for a successful PCS recovery because NVC causes most symptoms. It can also cause associated problems (like issues with vision or hormone problems) which in turn cause additional symptoms.
Dysautonomia
The autonomic nervous system reaches into nearly every organ in your body. It’s responsible for (or at least, closely involved with) processes that happen subconsciously, like your heart rate, speed of digestion, and breathing patterns. A dysfunction in that system is called dysautonomia.
Two important parts of the ANS are the parasympathetic nervous system (“rest and digest”) and the sympathetic nervous system (“fight or flight”).
In a healthy ANS, the parasympathetic (PNS) and sympathetic (SNS) nervous systems are both in a state of flux. They balance each other throughout the day, responding to the needs of each moment. For example, you need the sympathetic system to dominate if you’re running a race. But when it’s time to calm down afterward, you want the parasympathetic system to engage more strongly.
After a concussion, many patients suffer from sympathetic nervous system dominance. It causes a host of weird symptoms, including difficulty exercising, blood pressure issues, heart rate problems, body temperature changes, and more.
You can read more about dysautonomia after a head injury here.
Hormone Dysfunction
The pituitary gland and hypothalamus are both located in easy-to-injure parts of the brain. Some patients experience neurovascular coupling dysfunction in and around these areas of the brain, resulting in a change in hormone production. While some patients may experience an increase in certain hormone levels, the most common is hormone insufficiency after a mild traumatic brain injury.
Commonly affected hormones include growth hormone, cortisol, thyroid hormones, sex hormones, and more.
You can read more about hormone dysfunction after a head injury and how that affects your symptoms here.
Neck Problems
Your neck can also be driving some of your symptoms, especially if you experienced whiplash. Whiplash injury can stretch the nerve cells in your neck excessively. Whiplash can affect your vagus nerve, which interacts closely with the autonomic nervous system. Concussion injuries could also have resulted in physical damage like a bulged disk or a strained ligament. Even inflammation in the neck could impact the many nerve signals traveling through your neck into and out of your brain.
Concussion and whiplash could also result in misalignment (“subluxation”) of your neck vertebrae, especially in your upper cervical spine. 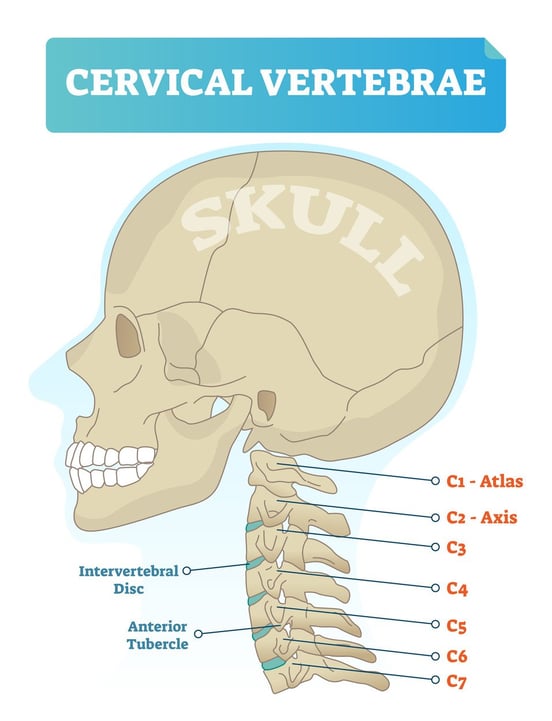 A chiropractor might adjust C1 or C2 to help with PCS symptoms.
A chiropractor might adjust C1 or C2 to help with PCS symptoms.
C1 or C2 misalignment can reduce blood flow to the brain, put pressure on the brainstem (impacting nerve signals traveling through it), and even impact cerebrospinal fluid drainage. C1 and C2 misalignment can drive headaches, eye strain, neck and jaw pain, balance problems or dizziness, and sometimes a sharp stabbing pain in the eye.
You can read more about neck pain after a head injury here.
Vision & Vestibular Issues
The vestibular system, a tiny organ located in each inner ear, is what your brain uses to determine your location in space. Both sides work together to keep you balanced and help your vision stay clear.
If you have vestibular problems after a head injury, it’s often because one side is sending a stronger signal than the other. When one ear is telling your brain one thing and the other ear isn’t quite corroborating the story, common symptoms like dizziness arise.
A concussion can affect your vision system as well. You might experience dysfunction in the optic nerves or the regions of the brain responsible for processing sight, for example. A concussion can affect eye focusing, eye teaming, eye tracking, peripheral vision, depth perception, and more. As a result, you could have blurry vision, eye pain, headaches, feelings of overwhelm in crowded spaces, and more.
You can read more about vision problems after a head injury here and more about vestibular rehabilitation here.
How a Chiropractor Can Help with Post-Concussion Syndrome
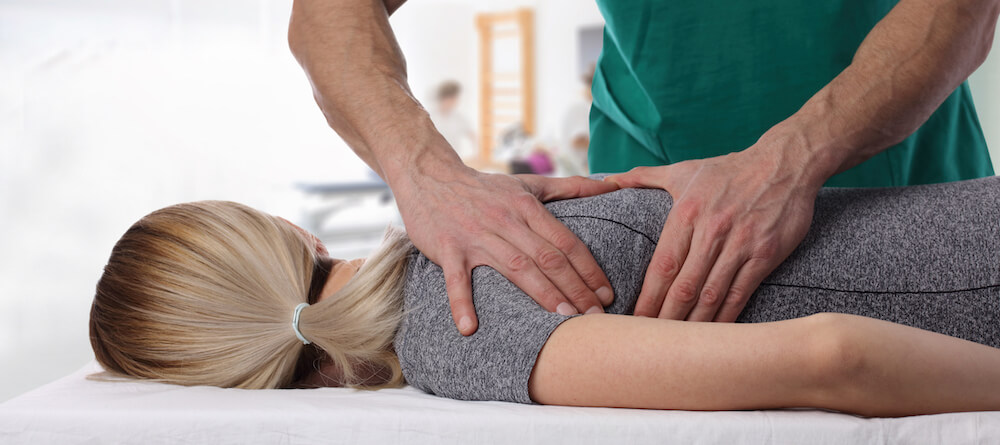
Spinal adjustments will help some patients and not others. That’s because not every patient has a spinal misalignment causing symptoms. As you saw in the section above, there are many possible causes for PCS symptoms and the neck is only one piece of that puzzle.
A chiropractor may be able to help reduce PCS symptoms via (a) gentle adjustment to C1 and C2, and (b) general assistance with neck pain, back pain, and muscle tension when those areas are contributing to symptoms.
If you do have a C1 or C2 misalignment, then a chiropractor might help. But not every chiropractor has the right training to adjust C1 and C2 properly. There are special techniques to manipulate those vertebrae safely. Because of their proximity to the brain stem, it’s dangerous to make sudden, sharp adjustments to them.
Let’s say that you find a knowledgeable chiropractor who adjusts C1 and C2 effectively. Often that is not the end of the story. After a concussion, there can be multiple forces acting on your vertebrae:
- NS dysfunction can cause the muscles in the neck to tighten inappropriately
- Muscles in the neck could be too loose, causing neck instability
- Vision or vestibular problems could cause you to move in unnatural ways, putting undue stress on your neck vertebrae and musculature
There are many pathways to and from the eyes and the vestibular system in charge of stabilizing the cervical spine. If those pathways don't also get rehabilitated, then the adjustments might not hold. It’s important to get the appropriate treatment (whether it’s physical therapy, vestibular therapy, vision therapy, etc.) to make sure adjustments “take.”
Without therapy to rehabilitate whatever is causing the neck problems, it’s common for patients to return week after week for the same adjustments. And while sometimes the adjustments will hold after a few sessions, repeated adjustments often result in hypermobility. The neck learns that it needs to rely on external adjustments to stay in place and the patient becomes dependent on weekly visits.
That is why it is so important to get appropriate therapy alongside upper cervical chiropractic adjustments for post-concussion syndrome.
In summary, chiropractic care can absolutely be beneficial for patients with post-concussion syndrome. But the adjustments need to be done in the right way and in combination with other therapies.
How to Find a Good Chiropractor
Two of our patients had very different experiences with their chiropractors, illustrating why it’s key to find the right practitioner.
Patient A went through our treatment program and made significant progress on most symptoms, but still struggled with headaches. Patient A then visited a chiropractor who diagnosed and adjusted a misalignment with C1 and C2. That adjustment is what the patient needed to finally stop having headaches.
Patient B had the opposite experience. Patient B went to a chiropractor who made an aggressive adjustment to C1 and C2, resulting in a new concussion. That patient then needed to visit our clinic for post-concussion treatment.
Chiropractic care is helpful when it’s needed, but it must be done safely. Those vertebrae are too close to the brain for an aggressive adjustment (which could cause a fresh injury). They can be adjusted, but only with gentle techniques which may require additional training and certification on the part of the chiropractor.
If you want to find a good chiropractor to help you with post-concussion syndrome:
- Look up reviews of the practice to read about other patients’ experiences, especially if they mention having post-concussion syndrome
- Ask the chiropractor how they handle C1/C2 adjustments. They should talk about gentle, slow techniques and avoid any sudden, sharp adjustments.
- Each adjustment should be reinforced by active movement. Ask if they will do this in-clinic with you or assign simple physical therapy exercises to help the adjustment hold and rehabilitate your neck muscles.
Finally, if the chiropractor claims to have functional neurology training, read our guide on the pros and cons of functional neurology for PCS.
How to Get Comprehensive PCS Treatment

Treating a brain injury isn’t one size fits all. Most programs provide the same set of therapies for every patient that comes through their program. Some get better, but many don’t. That’s because concussions don’t cause brain dysfunction in the exact same brain regions for everyone.
When patients come to our clinic, Cognitive FX, for treatment, we include an fNCI scan in their assessment (along with vision tests, balance tests, neurocognitive evaluation, etc.). An fNCI scan is a type of functional MRI that shows us which brain regions are dysfunctional and in what way.
Here’s an example of one of our patient’s scan results:
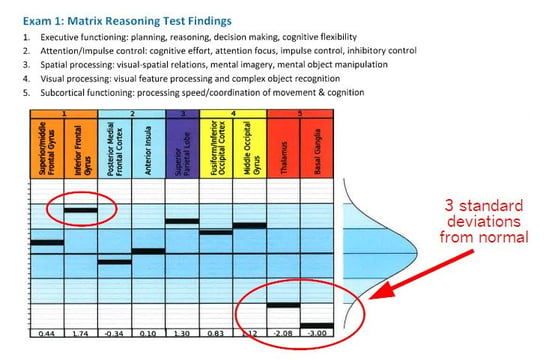
Olivia: “The fNCI showed that my thalamus was hypoactive and my basal ganglia were completely out to lunch. Three standard deviations from normal basically means that there was no activation seen in that area on the fMRI. All the work was being routed around it — causing fatigue and stress on the rest of my brain. The inferior frontal gyrus was trending toward hyperactive (using too many resources for given tasks).”
We use information from the scan to tailor your treatment plan to your injury. During treatment, we use a combination of exercise and multidisciplinary therapies, including (but not limited to):

Each patient’s therapy varies depending on their scan results, symptoms, and abilities. If you have issues affecting your upper neck, we’ll likely do some therapy exercises for the tongue because those muscles actually help stabilize the neck. We’ll often do exercises that work several systems at once, such as both vision and balance at the same time.
To make treatment as effective as possible, patients engage in supervised aerobic activity multiple times per day. Cardio exercise results in the Post Exercise Cognitive Boost (PECB): an increase of neurotransmitters in your brain that helps develop and promote healthy neurovascular coupling. Thanks to the PECB, your brain will be better able to tackle the challenges we give you in therapy and more disposed to neuroplasticity.
Neuroplasticity is at the heart of why this treatment approach works. The multidisciplinary exercises we use challenge multiple parts of your brain, pushing it to use more effective pathways to accomplish increasingly difficult tasks in therapy.
At the end of the treatment period, every patient gets a second fNCI scan so we can see how well their brains progressed. The average improvement on the second scan is 77%! If patients keep up with the homework we give them after treatment, they typically improve further at home.
If you’d like to discuss your injury with someone from our team, sign up for a consultation.
Should You See a Chiropractor?

Chiropractors are often criticized, but they can help certain patients with persistent symptoms of a concussion. It all depends on whether an alignment issue is contributing to those symptoms. When this is the case, the key is to find a good chiropractor who is trained to handle C1/C2 safely while seeking therapy simultaneously for the other causes of your symptoms. If your chiropractic care is in conjunction with a comprehensive care plan for your PCS, then it should help alleviate your symptoms.
If you’re experiencing symptoms that won’t go away after a concussion, we can help. On average, our patients show 75% improvement after one week of treatment. To learn about diagnosis and treatment options, sign up for a consultation.
















