As you read this text, your brain is processing the incoming visual information and sending directions to your eyes so they maintain focus on what you want to read. But if you have post-traumatic vision syndrome (PTVS) and your eyes do not work together efficiently, you may have a hard time keeping track of what you’re reading and develop a headache from your efforts. You may have also noticed that everyday activities that should be automatic — like reaching for an object, driving, or going shopping — require more effort.
Vision problems are common after a concussion or other source of brain trauma (even many COVID-19 long-haul patients have vision issues) and can remain for months, or even years, if left untreated.
What many PTVS patients may not realize is that post-trauma vision syndrome is usually part of a larger condition known as post-concussion syndrome (PCS).
PCS occurs when patients experience long-lasting symptoms (including vision issues) for more than three months after a mild traumatic brain injury (TBI) or another cause of acquired brain injury.
Some examples of other PCS symptoms include difficulty concentrating, headache, brain fog, fatigue, emotional dysregulation (anger, anxiety, depression, teariness, etc.), short-term memory problems, sleep issues, and more.
That means getting treatment for PTVS is just one part of the solution. Vision therapy can and will improve your symptoms, but it’s not likely to be the only type of therapy you need.
In our experience, post-trauma visual deficits result from a constellation of long-term effects from trauma, including dysfunctional brain signaling, autonomic dysfunction, and more. Most of these conditions will not resolve with vision therapy alone; it needs to be combined with other therapies to address your symptoms holistically.
At Cognitive FX, we follow a multidisciplinary approach to treatment. We offer a combination of physical exercises to prepare the brain and other therapies to address your specific symptoms.
In this post, we answer common questions about PTVS, including…
On average, our patients’ symptoms improve by 60% after just one week of treatment at our center specializing in neuroplasticity-based therapy. To see if you are eligible for treatment, sign up for a consultation.
How Can a Head Injury Result in Post-trauma Vision Syndrome (PTVS)?
.jpg?width=1000&height=445&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(5).jpg)
After a concussion, it’s common for patients to develop post-trauma vision syndrome (PTVS). With more than 50% of our brain dedicated to vision, it’s not surprising that this type of injury affects the visual system in some way.
Studies show that more than two-thirds of patients experience some impairments related to vision, such as problems with focusing and eye movements. About half of the patients have more than one vision problem.
PTVS is often caused by damage to the regions of the brain that are involved in vision. They can be affected even if the blow, stroke, or other traumatic injury wasn’t in the back of the head where the visual cortex is. These changes are often functional rather than structural (as we’ll see later) and can be difficult to detect by medical imaging.
Further reading:
To understand this condition, it is helpful to understand how your eyes and brain work together. When you look at something — your mobile phone, for example — your brain controls the muscles in the eyes that allow you to focus your gaze on a specific point. The image on your phone reaches special cells in your eyes called rods (cells responsible for your peripheral vision and night vision) and cones (cells responsible for your color vision and vision detail). In turn, these cells send this information through the optic nerve to an area at the back of your brain called the occipital lobe.
The parietal lobe is also involved in the visual process and is responsible for making you aware of the physical distance between you and the phone, as well as giving you depth perception. Next, information reaches the temporal lobe, which is associated with memory. This area allows you to recognize what you’re looking at from the raw visual information coming from your eyes.
It’s important to note that vision is not just about “seeing” things; eyes are an important part of your balance system. Information from your peripheral vision travels to a part of the brain called the brainstem, which is involved in spatial orientation.
Spatial orientation includes information about your surroundings, where you are in the room, where objects are relative to you, and how you can move through the space. It’s also connected to the vestibular system (which you can think of as the ‘balance center’ located in your inner ears).
Further reading: Vestibular therapy for post-concussion symptoms
In simple terms, anything that affects the functioning of the areas described above (and more) may lead to PTVS. While there are many contributors to post-traumatic vision problems (such as post-concussion medication side effects), the four main causes are dysfunction of the autonomic nervous system (ANS), neurovascular coupling (NVC) disruption, pre-existing visual dysfunction, and mismatched signaling between the eyes, vestibular system, body, and brain.
Dysfunction of the Autonomic Nervous System (ANS)
Disruption of the autonomic nervous system can affect the visual system in the brain and lead to PTVS. The two main branches of the ANS are the sympathetic nervous system (SNS), which prepares the body to face an emergency (fight or flight), and the parasympathetic nervous system (PNS), which maintains a resting state (rest and digest). v.jpg?width=552&height=515&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(8)v.jpg)
Under normal circumstances, these two sections work together to control a variety of bodily functions, such as breathing rates, heart rate, blood pressure, and pupil size.
Concussions can break this balance. For most patients, the SNS takes control more often than it should, keeping the body in a constant state of alert, which can be very stressful for the brain.
SNS dominance causes changes in how pupils react to light. For example, patients may experience slow pupil dilation, making it difficult to adapt quickly when the light changes, causing light sensitivity. v.jpg?width=552&height=582&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(2)v.jpg)
Disruption of the ANS can be responsible for a variety of other PCS symptoms, including fatigue, sleep disturbances, memory problems, and headaches.
Neurovascular Coupling (NVC) Dysfunction
PTVS and visual problems can also be the result of malfunction in the way that brain cells receive the resources they need. A network of blood vessels brings nutrients and oxygen to the nerve cells in a delicate, dynamic call-and-response relationship, called neurovascular coupling (NVC). However, if this mechanism is disrupted, the brain struggles to function normally.
If this disruption involves any of the areas of the brain linked with visual function (as described above), it may trigger problems with your vision. For example, damage in the area of the occipital lobe can cause difficulties processing visual information, while damage to the brainstem may lead to balance issues.
Mismatched Signaling
Some vision-related symptoms can come from how the brain, body (via proprioception, the body’s ability to sense movement), eyes, and vestibular system (inner ear) work together.
Normally, these parts of your body work together like GPS. Your inner ear, body, and eyes are like satellites and your brain is like the phone that’s triangulating your position. When all the information is consistent, your brain has a clear picture of where you are relative to everything around you.
But after a brain injury, signals from one or more of these sources may be mismatched (due to a variety of possible causes, including the neurovascular coupling changes discussed above).
Your brain has to work harder to figure out where you are in space and what’s around you. If your eyes and your vestibular system are sending conflicting information, it can result in vision-related symptoms.
Further reading: What causes dizziness after a brain injury
Pre-injury Visual Deficits
If you develop visual symptoms after a brain injury, it may be because you had pre-existing visual deficits that you were unaware of before your injury. The brain has an impressive ability to adapt and adjust to vision issues and can often compensate for them without you ever being aware of it.
But after a brain injury, it may be too difficult for your brain to continue compensating for those visual deficits. As a result, a condition that didn’t previously bother you can begin to cause obnoxious symptoms until it’s treated with vision therapy.
Symptoms of PTVS.jpg?width=1000&height=445&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(10).jpg)
Post-trauma Vision Syndrome can affect different areas of visual function in the brain, so that patients may experience many different symptoms. From a general point of view, PTVS may affect your ability to read, focus, and maintain attention. It can also cause symptoms that are indirectly related to vision, such as dizziness and headaches.
PTVS symptoms associated with vision include:
- Problems encoding, recognizing, and/or recalling visual information (poor visual memory)
- Double vision (diplopia) and binocular dysfunction
- Problems with ocular pursuits, including issues with eye movements and tracking ability (problems with saccades)
- Problems with focusing on an object (accommodative issues)
- Difficulties with shifting gaze quickly from one point to the other
- Problems with eye alignment
- Difficulty converging the eyes and maintaining binocular vision while focusing on a nearby target (convergence insufficiency)
- Problems accurately controlling eye movement accuracy and control (oculomotor dysfunction)
- Glare or light sensitivity (photophobia)
- Inability to maintain eye contact
- Blurry vision, especially nearsightedness (increased myopia)
- Perceived movement of print or stationary objects
- Asthenopia (eye strain or fatigue)
- Low blink rate
- Problems with depth-perception
- Visual-spatial distortions
- Exotropia (eye turned outward), exophoria (a tendency for the eyes to turn out), and other types of strabismus
- Difficulty searching and scanning for visual information (poor visual scanning)
- Visual snow (persistent dots in your vision)
Non-visual symptoms include:
Read how this patient overcame her difficulty reading, headaches, slow thinking, and more with treatment for post-concussion syndrome.
Let’s look at how some of these symptoms may affect your day-to-day life:
- Difficulty reading: PTVS can cause problems with the way the eyes work together, making reading and other activities that require focus extremely difficult. Patients often complain that words appear to be moving on the page or become blurred, which happens because the brain cannot control where the eye is focused. As a result, patients struggle to remember what they just read, even after several attempts.
- Poor hand-eye coordination: Patients with PTVS often experience problems with depth perception and the ability to shift focus on objects at different distances. As a result, they struggle to “see” where objects are around them, and stationary objects appear to move. This causes poor hand-eye coordination and complicates many daily functions, such as driving, climbing stairs, and reaching out to hold an object.
- Dizziness and poor balance: Vestibular, visual, and proprioceptive information (from muscles and joints) all need to accurately integrate together. If the visual system is not sending the right information to the brain, this will result in the same symptoms that occur with vestibular problems, including poor balance, nausea, and dizziness. Although the symptoms are similar, it’s possible to determine whether it’s a vision or a vestibular problem: If you feel dizzy after trying to switch focus between two objects, it’s more likely that it’s a vision problem. In contrast, if you have dizziness or disorientation while moving your head, it could be a vestibular issue.
- Headaches: Problems caused by PTVS, such as poor eye movement, eye tracking, and focusing, “force” the brain to put extra effort into visual function. Not surprisingly, patients experience headaches and migraines after tasks that rely heavily on vision, such as working on a computer or reading.
- Difficulty holding a conversation: PTVS can lead to difficulty concentrating on even simple tasks, such as holding a conversation. Most of the brain’s processing power is diverted to make sense of visual information, so there is less to allocate to other tasks.
Is It Possible to Treat PTVS with Glasses?
v.jpg?width=552&height=229&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(7)v.jpg)
Many patients come to us wearing glasses or eye patches to address their PTVS symptoms. This can be part of a neuro-optometric rehabilitation plan done to address specific conditions, like blurred or double vision.
- Corrective glasses: If you’re experiencing blurred vision, corrective glasses may help. If you already wore glasses before your injury, visit your optometrist and get your visual acuity checked. Even small changes can make a big difference in your eye care. If you need glasses for both near and distance, you may struggle to adapt to varifocals while you’re dealing with PTVS. In this case, it may be helpful to have two separate pairs of glasses.
- Specialized glasses such as prism glasses: These glasses have a prism added to the lens, which changes how the light comes into the eye. These are especially useful if you suffer from double vision or loss of visual field. These glasses are used only for short periods during the day (not all of the time like corrective glasses).
- Patching: This involves covering one eye or part of the visual field, and it’s used to help with double vision. The aim is to block the information that causes double vision from reaching the brain.
If done correctly to address specific symptoms, these glasses can be helpful for some patients. However, none of these specialized glasses should be seen as a stand-alone method to treat PTVS. They’re only one possible tool to address vision symptoms and should not replace a more comprehensive plan to rehabilitate your brain. Essentially, these glasses are like a crutch — they provide some assistance, but they do not treat the cause of your vision issues.
In fact, over reliance on them tends to delay recovery rather than help. It’s not uncommon for patients to wear glasses longer than they should or even use them as their only way to cope with symptoms. We see this especially in patients who were prescribed the glasses without a long-term rehabilitation therapy plan or when patients decide to buy them without checking with their neuro-ophthalmologist or neuro-optometrist.
For an in-depth look at how these and other types of glasses can help PCS patients read our article on five types of glasses to help after a concussion.
Treating PTVS (and Other PCS Symptoms) at Cognitive FX
.jpg?width=1999&height=1333&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(4).jpg)
Instead of relying only on glasses or other approaches to treat specific symptoms in isolation, we believe that the best treatment plan to treat visual dysfunction is to tackle the root of the problem and resolve multiple PCS symptoms at the same time. The aim is to get the brain back to optimal functioning for each patient (or as close as we can get it).
Our treatment — called Enhanced Performance in Cognition (EPIC) — is a custom program designed to treat each patient’s specific symptoms, including vision problems.
Before treatment, each patient receives a Functional Neurocognitive Imaging scan (fNCI), which shows our team which regions of the brain were affected by your injury and how well they’re communicating with other brain regions.
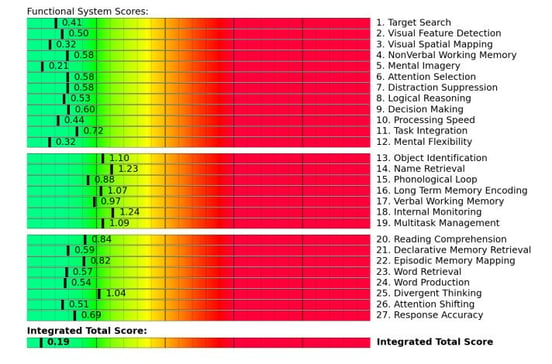 Overall fNCI results from a patient with neurovascular dysregulation.
Overall fNCI results from a patient with neurovascular dysregulation.
Using the information from the scan, we design a treatment plan tailor-made just for you. Ultimately, our treatment aims to restore normal neurovascular coupling and ANS function in the areas highlighted as dysfunctional by our evaluation.
During treatment, patients go through an intense regime of aerobic exercise and a variety of different therapies, including:
- Vision therapy
- Neuromuscular therapy
- Occupational therapy
- Vestibular therapy
- Cognitive therapy
- Sensorimotor therapy
- Neurointegration therapy
- Psychotherapy
- And more.
All of our therapies include a visual component, though some focus on vision more heavily than others. Some examples include Dynavision and the Brock string.
.jpg?width=1999&height=1333&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(1).jpg)
Dynavision is a computerized light board where patients push buttons as they light up in different patterns on the board. Sometimes, you’ll simply hit every button that lights up as quickly as you can after noticing it. Other times, you’ll need to exercise selective button-slamming skills by hitting only the red while avoiding the green, for example. Dynavision is great for oculomotor coordination and for activating a number of brain regions involved in movement, cognition, and vision.
We also use the Brock string for patients with visual perception issues. This tool helps retrain the eyes to work together when you focus on beads located at different distances along the string.
.jpg?width=1999&height=1333&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(3).jpg)
In neurointegration therapy, you’ll perform exercises designed to help the brain, eyes, inner ear, and body to work together harmoniously.
The overall effect of these therapies working in combination is greater than if you were just pursuing one type of therapy at a time. When you activate the whole brain, positive changes tend to happen faster and in larger bursts because of the way the treatment works as a whole. Sometimes, we’ll see patients who had been receiving vision therapy but who hit a plateau in treatment. When they come to Cognitive FX and have the neurovascular coupling component addressed, it’s much easier for their system to respond to vision therapy and resume improving.
That said, the eyes are slow to change. One week’s worth of therapy is often not enough to address all vision issues. The eyes can take anywhere from six months to a year of vision therapy to recover fully. Treatment at Cognitive FX can provide a significant reduction in symptom burden and resolve many of the underlying issues, but there is no replacement for consistency in vision rehabilitation. We can refer you to a vision specialist in your hometown and teach you specific exercises to do at home.
A second follow-up fNCI at the end of the treatment allows our team to see how brain function is improving. 90% of our patients experience improvements during treatment, and most continue improving at home.
After your follow-up scan, a member of our team will analyze your results and give you some “homework.” Your homework will include some combination of aerobic exercise, cognitive games, and cognitive rest as you continue your recovery journey.
Strategies to Manage Vision Problems at Home
.jpg?width=1000&height=445&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(9).jpg)
Attending treatment at Cognitive FX goes a long way to treat your visual symptoms, but, as we mentioned earlier, these will not disappear within one week, and you will likely need further vision therapy.
While you’re recovering, the following strategies may help you cope with your symptoms:
Take frequent breaks: Take frequent breaks, especially when doing tasks that rely on vision, such as reading or working on the computer.
- Follow the 20-20-20 rule: Look up every 20 minutes and focus on something at least 20 feet away to give your eyes a break.
- Increase the font size you use on the computer. This makes it easier to read and is less tiring on your eyes.
Further reading: Taking breaks is good for your brain
Make clever use of lights: Lighting can help improve vision when completing tasks. Some ideas include the following:
- Check the wattage of the bulbs in the home, and increase or decrease their power if needed.
- Experiment with bulb types to find the lighting that works best for you; many patients find fluorescent lights bothersome.
- Use natural or non-glare light as much as possible.
Avoid visual overload. Reducing visual overload can reduce the strain on your eyes and make things easier to find in your home.
- Cut down on clutter. Routinely pick up and put away items you don’t need so your living space is more clear.
- Find one specific place for a frequently used item, such as your car keys or mobile phone. Not having to search in multiple places for what you need will reduce overwhelm.
Reduce tripping hazards: Look around your house for items that can be a trip hazard. A few good ideas include:
- Removing area rugs
- Moving small furniture items, such as end tables, out of walking paths.
- Placing large furniture with wide spaces between them.
- Using nightlights in areas of the house you might walk through on the way to the bathroom or kitchen.
Make use of contrasting colors: Using contrasting colors can help you find objects more easily. For example:
- Use covers for plugs and switches that contrast with the color of your walls.
- Use a light or a dark cutting board to contrast against the food you’re cutting.
- Increase contrast on your TV and computer.
Clean your glasses: Dirty glasses can further add to visual distress. So can glasses that fit the bridge of your nose incorrectly.
Use blue light filters: Take advantage of blue-light filtering. You can:
- Use the nighttime settings on your computer screen and mobile devices to reduce blue light.
- Wear blue light-blocking glasses while working on the computer.
- Put away your cell phone and turn off the TV an hour or two before bed.
Try our at-home headache management course: Our course on improving your headaches at home also includes a section on addressing vision-related issues. You may find that it provides much-needed relief as you wait for your treatment program to begin.
On average, our patients’ symptoms improve by 60% after just one week of treatment at our center specializing in neuroplasticity-based therapy. To see if you are eligible for treatment, sign up for a consultation.

.jpg?width=1000&height=445&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(5).jpg)
v.jpg?width=552&height=515&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(8)v.jpg)
v.jpg?width=552&height=582&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(2)v.jpg)
.jpg?width=1000&height=445&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(10).jpg)
v.jpg?width=552&height=229&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(7)v.jpg)
.jpg?width=1999&height=1333&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(4).jpg)

.jpg?width=1999&height=1333&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(1).jpg)
.jpg?width=1999&height=1333&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(3).jpg)
.jpg?width=1000&height=445&name=Why%20Most%20Post-Trauma%20Vision%20Syndrome%20Treatment%20Falls%20Short%20(9).jpg)









.png?height=175&name=Vision%20Problems%20After%20COVID%20Causes%20and%20Treatment%20(1).png)